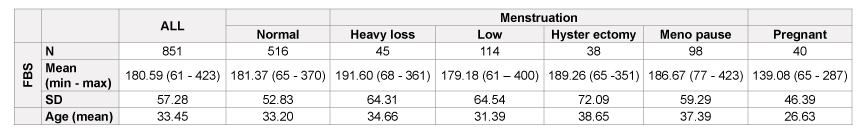
Table 1: Fasting plasma glucose and age in relation to menstrual patterns

Menstruation in Diabetes Mellitus: A Study from South India
Nagamani G1 Venkata Putcha2 Marcus Lind3 GR Sridhar4*
1Dept of Obstetrics and Gynecology, Andhra Medical College, Visakhapatnam*Corresponding author: GR Sridhar, Endocrine and Diabetes Centre, 15-12-15 Krishnanagar, Visakhapatnam 530 002, India, E-mail: sridharvizag@gmail.com
Menstrual disturbances are associated with insulin resistance, diabetes and presage cardiovascular risk. Here we assess menstrual pattern in adult women with type 2 diabetes mellitus and correlate with the fasting plasma glucose (FPG). Among 851 consecutive women 516 had normal cycles, 45 menorrhagea, 114 oligomenorrhea, 38 underwent hysterectomy 98 reached menopause and 40 were pregnant. The mean age (yrs) in each group respectively was 33.45 yrs, 33.2, 34.66, 31.39, 38.65, 37.39 and 26.63. Applying Poisson regression risk rate, sedentary women with normal menstruation, amenorrhea and menopause, had higher FPG. Body mass index: lean subjects (<20 kg/m2 ) had higher glucose levels in those with (a) normal cycles (b) oligomenorrhea and who reached menopause. A similar pattern occurred in the overweight and obese (viz those with menorrhagea and oligomenorrhea). In summary, menstrual irregularity, as a surrogate for cardiovascular risk was common in Asian Indian diabetic women from our Centre.
Disturbances in menstrual pattern have been linked to type 2 diabetes mellitus. A number of operating factors operate, such as were suggested including, obesity and metabolic abnormalities including inflammatory mediators. Large epidemiological studies focused on pattern of menstrual cycle as a forerunner of type 2 diabetes mellitus and of coronary artery disease [1-3].
However, there have been few studies on the pattern of menstruation among women with type 2 diabetes when they present for management of diabetes. The purpose of this study is to evaluate menstrual status among women with diabetes mellitus who presented to our Centre between the years 1994 and 2004. The data was extracted from our large electronic medical record currently comprising more than 50,000 subjects with diabetes [4]. The trends (age group, gender) of subjects presenting have been published [5].
From our electronic medical records, the following parameters were extracted and evaluated in women who presented with diabetes between 1994 and 2004: current age, age at diagnosis of diabetes, pattern of physical exercise, family history of diabetes, and pattern of sleep [6], body mass index and menstruation at the time of presentation.
Normal menstruation was taken as self reported cycles between 26 and 41 days and delayed or irregular cycles as those of more than 40 days [1,7]. Cycles of fewer than 26 days were considered short. Menopause was considered when the last menstrual period occurred at least 12 months ago. A history of hysterectomy was elicited.
Hotelling T-square test was employed to tabulate the ages and Poisson regression was performed to derive the incidence risk ratios for other variables.
Among 851 women, 516 reported normal menstrual cycles (Table 1). Forty were pregnant. The fasting plasma glucose was elevated across all pattern of menstruation except in those who were pregnant (Table 1). The mean age of non pregnant women ranged between 33.2 and 38.65 among all groups of menstrual pattern, except pregnancy (Table 1).
Among the other parameters evaluated, subjects with self reported disturbances in sleep in those with normal menstrual cycle had a higher incidence risk ratios (p<0.005) (Table 2). Similarly women with a lower body mass index (<20 kg/m2 ) had a lower incidence risk ratio of shorter and heavier menstrual cycles (p<0.05) (Table 2). Similarly among those who reached menopause, those in the obese group (BMI >29 kg/m2 ) had a lower incidence risk ratio (Table 2).
In this study of relatively young group of women with type 2 diabetes who presented to our Centre, majority reported having normal menstrual cycles. Risk of having shorter menstrual cycles was lower in those who were lean. Those in the highest BMI range had a higher incidence risk ratio of reaching early menopause.
Studies reporting on irregular menstrual cycles being a risk factor for type 2 diabetes reported that leanness was not protective; both lean and obese women with irregular cycles were at risk of developing diabetes mellitus [1]. In contrast among Pima Indian women, the diabetes and menstrual irregularity significantly associated with the least obese women, with a BMI less than 30. In those who had a BMI more than 30 absence of irregular menstruation was not protective of diabetes [2]. It was interpreted as This was ascribed to obesity being associated with insulin resistance and hyperinsulinemia, the latter, besides causing hyperandrogenism and irregular menstrual cycles, are known to predispose to diabetes [2]. Cooper et al reported that long or irregular menstrual cycles were not a risk for diabetes mellitus in the post menopausal age, although there was a trend for longer bleeding duration to be associated with postmenopausal diabetes [8]. A more recent study showed that women with a history of irregular menstrual cycles were at risk both for type 2 diabetes and coronary heart disease, although the risk could not be explained by conventional metabolic risk factors or altered hormone levels [9].

Table 1: Fasting plasma glucose and age in relation to menstrual patterns
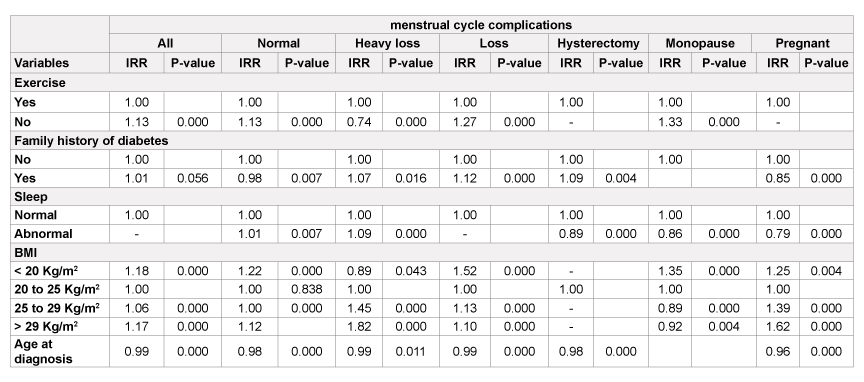
Table 2: Incidence risk ratios of all, normal and menstrual patterns
There have been some reports of type 1 diabetes mellitus being associated with an earlier menopause and a shorter reproductive life [10] and of a central mechanism at the hypothalamo-pituitary cause for menstrual abnormalities [11].
One of the first studies on menstrual function among women with diabetes on Pima Indians was published in 1994 [3]. In a retrospective analysis, 20 women with hyperinsulinemia and 20 control women (age: 18-45 years) were studied. From a review of medical records, and by measuring hormone levels in stored serum samples, women with hyperinsulinemia were shown to have had irregular menstruation when compared to controls. Irregular menses was associated with elevated testosterone levels, when compared with to hyperinsulinemic women with regular menses. Occurrence of obesity, hyperinsulinemia, irregular menstruation and elevated testosterone level, (the components of polycystic ovary syndrome) was reported in this cohort [3].
Pathogenetic evidence linking menstrual irregularity with diabetes mellitus was described in later years. Obesity is associated with enhanced peripheral adipose tissue conversion of androgens to estrogens [12]. The hyperestrogenemia was postulated to result in menstrual abnormalities acting via negative feedback at the level of the hypothalamo-pituitary axis [3]. In addition insulin can stimulate ovarian androgen production (as found in PCOS), which may explain the relation between the two conditions. Hyperinsulinemia also inhibits the hepatic production of sex hormone-binding globulin (SHBG), thereby leading to higher levels of free testosterone levels [13]. Lower levels of SHBG are a known risk factor in women for development of diabetes mellitus in women [14].
What is significant in this study of relatively young women with diabetes is, more than 15% (n: 114) a significant proportion underwent hysterectomy (n:36) or had reached menopause (15.98%; n: 136). In addition, 13.4%. This is consistent with studies from India where leanness did not protect from insulin resistance; young women presenting with PCOS had greater intimal medial thickness, a surrogate for future cardiovascular events compared to weight matched controls [15].
In addition there is gender disparity in psychosocial stress, with women having diabetes experiencing greater difficulty in coping with the disease [16]. Stress is a well recognized predisposing factor to the cause and management of diabetes mellitus [17]. Besides, women with PCOS were also reported to have greater mental distress in a south Indian population [18]. It is all the more understandable that a variety of factors operate in the menstrual irregularity of these group of women with diabetes mellitus from south India.
One may speculate that the threshold for performing hysterectomy is low, leading to surgical treatment for a condition that must have been more carefully evaluated and perhaps treated by lifestyle and medical measures. The current study therefore lends support to the need for physicians treating women with PCOS to be aware of the increased risk of diabetes mellitus. And Advise must be provided about lifestyle changes in addition to measures along with treatment of cosmetic and reproductive presenting features [19]. Finally one must carefully assess the cause of menstrual irregularity in type 2 diabetes to identify and initially medically manage causative conditions before performing hysterectomy.
Download Provisional PDF Here
Article Type: Research Article
Citation: Nagamani G, Venkata P, Lind M, Sridhar GR (2015) Menstruation in Diabetes Mellitus: A Study from South India. J Dia Res Ther 1(1): doi http://dx.doi.org/10.16966/2380-5544.103
Copyright: ©2015 Nagamani G. et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access