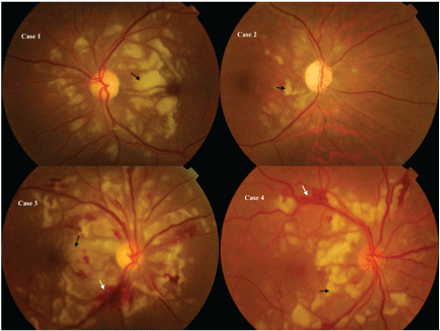
Figure 1: Black arrow: Purtscher flecken; White arrow: retinal haemorrhage


Rajya Laxmi Gurung*
Department of Vitreo-retina, Biratnagar eye hospital, Biratnagar, Nepal*Corresponding author: Rajya Laxmi Gurung, Department of Vitreo-retina, Biratnagar eye hospital, Rani Mills area-17 Biratnagar, Nepal, E-mail: rajya82@yahoo.com
Purtscher’s retinopathy is a rare and severe angiopathy associated with non-ocular crush injuries. Several ophthalmic reference sources describe it as occurring in either one or both eyes. Descriptions of monocular cases are rare. This retrospective review of four cases of purtscher’s retinopathy highlights the unilateral clinical presentation of purtscher’s retinopathy.
Purtscher’s Retinopathy; Monocular; Angiopathy
Purtscher’s retinopathy also known as angiopathia retinae traumatica is a rare and severe angiopathy first described by Otmar Purtscher in the year 1912 associated with non-ocular crush injuries [1]. Several reports describe it as occurring mostly binocular [2]. Descriptions of monocular cases are rare [3]. We report 4 cases of unilateral purtscher retinopathy with an aim to evaluate the clinical presentation; management and visual outcome.
Method
The present case series is a retrospective review of 4 patients of monocular purtscher’s retinopthy who presented between March 2014 to April 2015. The data were compiled from evaluation of clinical records to document the clinical course, details of management and visual outcome. Diagnosis of purtscher’s retinopathy was based on history of non-ocular trauma with any of the following:
Detailed slit- lamp examination with fundus evaluation was done in all the cases at the time of presentation, 1 month follow up and 3 months follow up. Fundus photography, fluorescein angiography was done according to availability of machine.
All the patients were managed conservatively with close follow up. No forms of oral or intravenous steroids were given.
The age of the patients ranged from 30 - 45 years with a mean of 37.25 years (Table 1). Male predominated with a ratio of 3:1. Road traffic injury was the cause of impact in all the 4 cases. Right eye was affected in 3 eyes whereas left eye in 1 patient. All the patients were symptomatic presenting with best corrected visual acuity (BCVA) hand movement (HM n=2), 6/60 (n=1) and 6/36 (n=1). The mean interval between trauma and seeking consultation was 24.75 days (range: 10 days - 60 days). Anterior segment evaluation was un-remarkable in all the cases. Fundus evaluation revealed classical multiple polygonal areas of whitening (purtscher flecken), between the retinal arterioles and venules affecting the posterior pole (Figure 1). Retinal hemorrhages and cotton wool spots were also present. Fluorescein angiography revealed capillary non-perfused areas, retinal oedema, occluded retinal arterioles and perivenous staining (Figure 2). Final BCVA improved in all cases by a minimum of two snellens line at 6 months follow up with subsequent improvement in fundus findings.

Figure 1: Black arrow: Purtscher flecken; White arrow: retinal haemorrhage
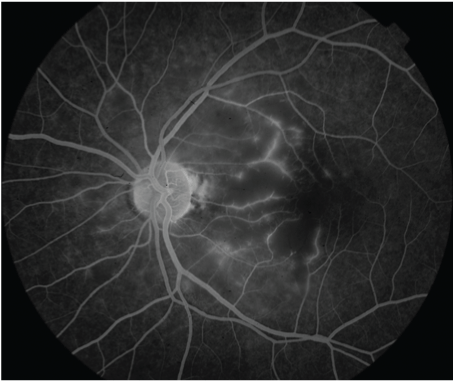
Figure 2: Fluorescein angiography
Table 1: Demographic profile and clinical features of the patients
RTA: Road Traffic Accident; RE/LE: Right Eye/Left Eye; PF: Purtscher Flecken; CWS: Cotton Wool Spot; RH: Retinal Haemorrhage; HM: Hand Motion; BCVA: Best Corrected Visual Acuity; FA: Fluorescein Angiogram; CNP: Capillary Non-Perfusion; NA: Not Available
This retrospective review summarizes our 2 years experience of clinical presentations and management of unilateral purtscher’s retinopathy. Purtscher’s retinopathy was first described by Otmar Purtscher in 1912 [1]. Since its original description, purtscher and purtscher like retinopathy has been associated with compressive chest injuries, long bone fractures, acute pancreatitis, [4] strenuous child birth, [5] connective tissue disorder, retrobulbar anaesthesia, haemodialysis. Though the exact pathogenesis of purtscher retinopathy is controversial, the commonly accepted mechanisms include complement activation, embolism theory and the transmission of hydrostatic shock waves resulting in endothelial damage [6].
In the present series, all patients presented with unilateral blurring of vision following road traffic accident. Purtscher’s retinopathy is usually bilateral, [2] and there is some dispute in the literature concerning its unilateral presentation. Unlike reported by Agrawal et al, [2] the four cases in this series clearly had only one eye involved. Madsen, [7] reported 6 cases, 3 of which were unilateral. Blodi et al, [8] reported a case of unilateral involvement of purtscher-like retinopathy after retrobulbar anaesthesia. Unlike Agrawal et al where, only 33% of cases of RTA had unilateral purtscher’s retinopathy, all cases in our series had monocular presentation following RTA. The pathognomonic purtscher flecken [1,2], and cotton wool spots were recognised in all cases and retinal hemorrhages were seen in 50% of cases. There are only few fluorescein angiographic descriptions of purtscher’s retinopathy [3]. The fluorescein angiography in one of our series showed capillary non perfused areas, retinal oedema, arteriolar occlusion and perivenous leakage. A potential weakness of our series is lack of fluorescein angiography in all cases.
The treatment of purtscher’s retinopathy is of debate [2]. Isolated case reports of improvement in vision with intravenous methylprednisolone have been reported [9], however other published case series have reported improvement in visual function without any specific treatment [2]. None of the patients in our series were given intravenous methylprednisolone, all were managed conservatively with close follow up. All the patients had a minimum of 2 line improvement in BCVA at final follow up with resolution of all posteror pole findings.
In conclusion we would like to emphasize that purtscher’s retinopathy is rather rare. The case series presented here clearly demonstrates that the disease may be monocular. Spontaneous visual recovery can be seen without any treatment.
Download Provisional PDF Here
Article Type: Case Series
Citation: Gurung RL (2017) Unilateral Purtscher’s Retinopathy; Review of 4 Cases. J Ophthalmic Stud 1(1): doi http://dx.doi.org/10.16966/2639-152X.102
Copyright: © 2017 Gurung RL. This is an openaccess article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access