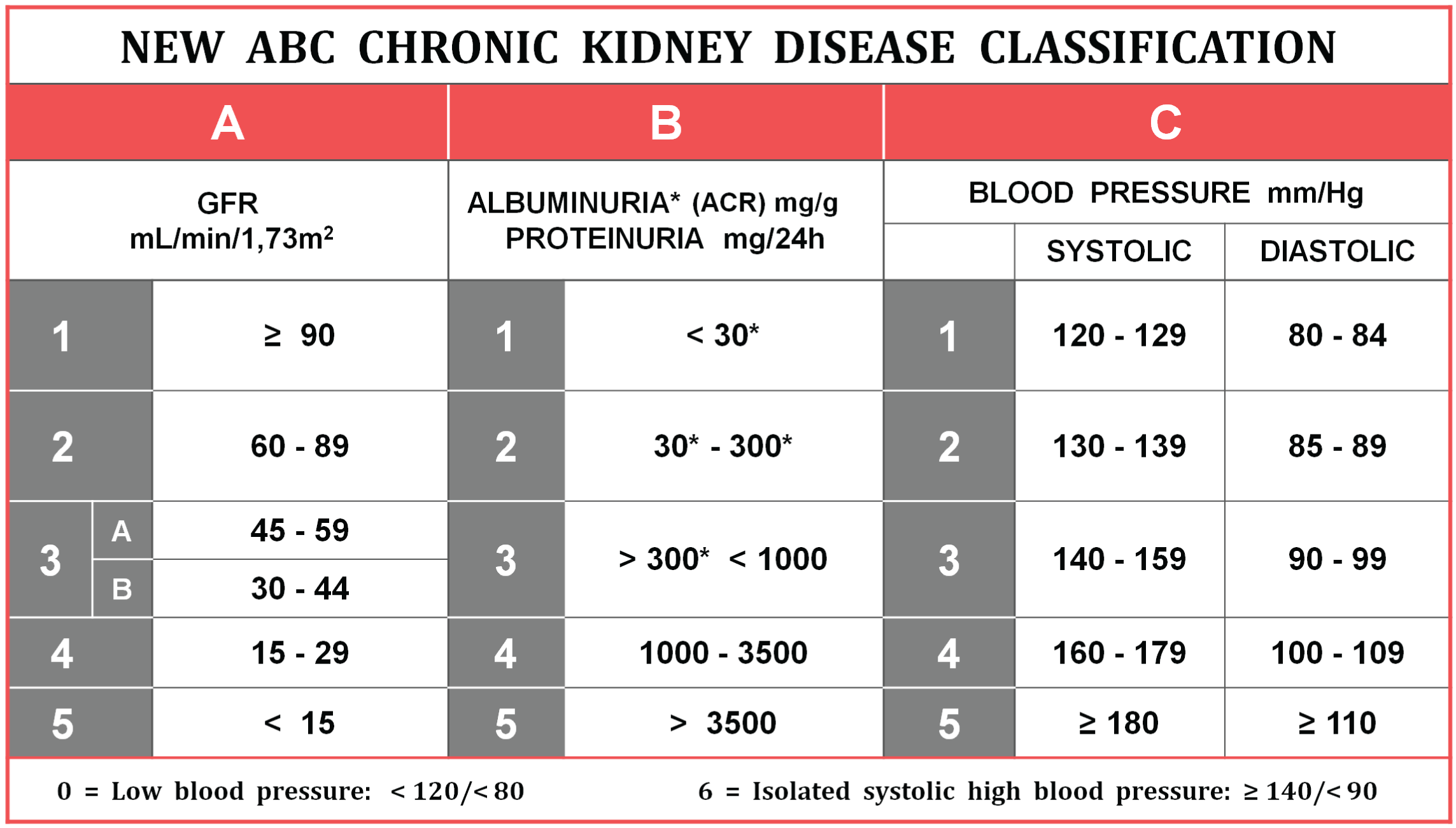
Table 1: New ABC Chronic Kidney Disease Classification


Jaime Arturo Jojoa1* Carolina Enríquez Rivera2 Edison Muñoz Delgado3 Harold Mauricio Casas4 Giovana Marcella Rosas55 Carol Yovanna Rosero6 Franco Andrés Montenegro7
1Nephrologist Fundación Hospital San Pedro and Hospital Universitario Departamental de Nariño - Dialisur, Pasto, Colombia, Professor of Nephrology and Internal Medicine of Universidad Cooperativa de Colombia, Pasto, Colombia*Corresponding author: Jaime Arturo Jojoa, MD. Calle 22A # 41A-57, Apto 302, Edificio Arcadia, Barrio Morasurco, Pasto - Colombia, South America, E-mail: jaimearturojojoa@gmail.com
Since 2002, KDOQI and KDIGO groups have searched the best way to assess, define and classify Chronic Kidney Disease (CKD) to facilitate their diagnosis and optimize treatment. Growing evidence in recent years has shown a strong link to albuminuric (proteinuric) diseases and High Blood Pressure (HBP), risk factors that when integrated in a single classification, offer us a new way to define and classify CKD, which in addition to showing us the severity of the disease also suggest a prognosis value according to the level of albuminuria (proteinuria) and HBP.
Chronic Kidney Disease (CKD); New ABC Classification; Glomerular Filtration Rate (GFR); Proteinuria; Albuminuria; Albumin Creatinine Ratio (ACR); Protein Creatinine Ratio (PCR); 24-hour urine protein collection; High Blood Pressure (HBP); Diabetes Mellitus; Progression.
Based upon the following considerations we propose a new way to classify Chronic Kidney Disease (CKD), which is universal, easily applied, does not exclude any type of patient, is low cost, has great impact on the interpretation, diagnosis, prognosis and treatment of the disease, does not underestimate the multiple achievements obtained thus far by clinical research, widens the conceptualization of the disease and optimizes economic resources without neglecting the health and welfare of individuals who are the principal objectives of any system of health care.
Classification of a disease is proposed because several elements of confusion exist which impede diagnosis, severity, treatment or prognosis; therefore, principal characteristics or factors which identify and determine it are employed for initially establishing useful parameters. In 2002, the National Kidney Foundation Kidney Disease Outcomes Quality Initiative (NKF KDOQI) group introduced a conceptual model for defining and classifying 5 states of CKD depending upon the quantification of Glomerular Filtration Rate (GFR), which permitted the unification of nomenclature and guided the development of multiple clinical research studies and public health policies throughout the world [1]. In 2004, the Kidney Disease Improving Global Outcomes (KDIGO) group backed this reference system, emphasizing some specific conditions with the utilization of letters as sub-indexes; for example, patients with kidney transplant were recognized with the letter T, those with dialysis with D and the letter P was utilized for patients who had proteinuria, clarification which did not have the expected impacts since it only mentioned the associated condition [2].
Motivated by the validity of the classification based upon GFR, research in the following years focused on finding a method which would permit exact measurement [3]; in this way estimative forms to measure kidney function was validated by systems like Modification of Diet in Renal Disease (MDRD) and later, Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI). These attained their objective since they achieved values which were very close to standard reference [4]; besides, in this analytical process and with the publication of new clinical results, state 3 was subdivided into A and B to better specify cardiovascular risk [5].
People who develop kidney disease usually present certain characteristics of genetic and racial susceptibility, which when associated with diseases like diabetes mellitus, high blood pressure or autoimmune diseases, initiate a pathological process which usually accelerates in the presence of proteinuria [6]. Other factors such as obesity, dyslipidemia, and tobacco consumption are associated even more with cardiovascular risk and other alterations like anemia and acidosis which constitute complications in advanced stages of the disease, more than causal risk factors.
Albuminuria-Proteinuria: Since albuminuria or proteinuria is one of the principal factors in progression of CKD, great effort has been dedicated to the method to quantify as exactly as possible urinary elimination, for this reason, and considering the difficulties of collecting and measuring urine for 24 hours and the high risk of improper realization of the procedure, it was necessary to find a standardized specific, reliable and reproducible method for quantifying the excretion of albumin or proteins in urine. The Albumin Creatinine Ratio (ACR) in urine has shown great exactitude in the quantification and correlation with important adverse events in the progression of kidney disease, mobility, cardiovascular mortality, general mortality, among others [7]. In 2009, due to the great correlation between albuminuria and important adverse events, its inclusion was proposed as a second classificatory parameter in prognostic and progression factors of CKD [8,9].
After a decade of continuous advancement, attempting to discover a better way to interpret the concept and management of CKD, in 2012, various studies demonstrated that by combining the relative risks of GFR and albuminuria, a series of adverse events were presented, such as the progression of CKD, cardiovascular mortality, general mortality, among others. Therefore, the KDIGO group published a new classification which conserved the values of GFR organized vertically, combined with 3 quantitative ranges of albuminuria measured as ACR, located horizontally and denominated A1 (less than 30 mg/g), A2 (between 30 mg/g and 300 mg/g) and A3 (above 300 mg/g), thus generating a table of risk classification [10].This form of CKD classification permitted us to identify patients with low, medium and high risk of presenting adverse events related to a lower GFR and a greater quantity of albumin in urine; while this classification recognizes high-risk patients for evaluation and specialized management referral, it does not establish a specific therapeutic strategy to be followed.
It is important to recognize that this system interprets the concept of CKD better, demonstrating different degrees of severity, influenced by a modifiable variable like albuminuria determined by ACR, which has been validated in various clinical studies. However, this type of classification does not include values of albuminuria or proteinuria in ranges superior to 300 mg/g in the ACR [11]; this underestimates the consequences of severe proteinuria, cases in which therapeutical objectives aim to diminish the level at least below the nephrotic range (3.5 gm. of 24 hour urine protein collection) or when possible less than 1 gm. of 24 hour urine protein collection, a condition which has not been sufficiently analyzed in previous studies.
High Blood Pressure: In addition, in recent years there is growing evidence of the association between high blood pressure, above all systolic, and progression towards more advanced stages of CKD [12,13]. Anderson AH et al. [14] in a cohort of 3708 patients, followed during a period of 5.7 years, demonstrated that systolic blood pressure above 130 mm/Hg is closely associated with a greater progression of this pathology. Similar findings have been made by Hillel S et al, Geogi Abraham et al. [15] among others, with higher arterial pressure values, especially above 140/90 mm/Hg].
If we analyze the final results of these two pathological processes, which generate tubular interstitial damage through apoptosis induced by proteinuria and glomerular sclerosis with tubular interstitial fibrosis due to barotrauma, endothelial dysfunction, vasoconstriction and chronic hypoxia secondary to high blood pressure [15,16], we have a great physiopathological support for redefining the concept of CKD, above all, taking into account that other factors, while not to be ignored, do not have an impact of this magnitude.
In recent years the lines of research generated around CKD has emphasized molecular, genetic and ultra-structural aspects, looking for new biomarkers of damage and progression of the disease; equally, computerized systems have been developed which combine multiple clinical variables, trying to identify those patients with kidney disease who remain stable or progress to more advanced stages. This objective has been difficult to achieve in light of the fact that the presentation of the disease in particular and can change its characteristics as time passes [17].
We know that this classification has permitted the unification of concepts, identification of risk, location of regions with high incidence of End State Renal Disease (ESRD) like Taiwan, Jalisco (Mexico), United States, Singapore, Thailand, China [18], among others. However, due to the growth of affected population, it is necessary to propose a new classification which includes a greater number of elements which permit a better orientation in therapeutic decision-making to change the natural history of the disease. This objective appears not to have been achieved; taking into account the incidence of CKD in the majority of countries of the world has a persistent yearly increasing curve, according to the registered database of USA [19].
Looking at only one example, en 2005 the program for promotion and prevention of CKD was implemented in Colombia, resulting in an ascendant curve in the number of patients in the chronic dialysis program, which increased from 21.572 cases in 2008 to 30.844 in 2015. This figure evidences the existence of an uncorrected problem impeding modification of disease evolution, although, being skeptical it could be thought that factors such as the increase of in health coverage, greater and better register of patients, significant population increase, among others, were responsible for these findings [20].
Besides the impact of quality of life for the patient, economic effects of the disease on health systems must be taken into account; spending superior to 1 trillion dollars annually for the care of ESRD patients, shows that we face a serious unresolved problem. Therefore, in 2015, Olivier J. Wouters et al.[21] emphasized that the available tools to diagnose and intervene CKD have great limitations which must be re-conceptualized as part of primary health attention.
Given the progressive increase in the incidence of ESRD and the persistent difficulty to achieve better control of CKD, in November, 2016, we proposed a novel multifactor concept of the disease [22], which includes previous parameters (GFR), albuminuria amplified to higher ranges and the addition of high blood pressure as a classificatory variable, due to the physiopathological factors previously mentioned and since it is the second cause of CKD in the world [23,24]. To facilitate its comprehension and clinical management, each variable has been assigned a letter which identifies the parameter being measured; A: glomerular filtration rate, B: proteinuria and C: high blood pressure.
The concept of inter-relating three quantifiable variables generates a table of values in which each one is located horizontally and shows its respective reference values in the vertical form. Each column has 5 ranges according to concepts and modifications established in the present article.
In the case of variable A, parameter which identifies and defines the presence and severity of CKD, the KDIGO classification is conserved without modification, the B variable maintains the two initial values of the albuminuria of the 2012 KDIGO classification quantified as ACR and identifying them as 1 and 2, but adds and quantifies the proteinuria for higher ranges with numbers 3, 4 and 5, permitting better understanding of the proteinuria effect upon the kidney structure. For the C variable, we adopted the directives of the European Society of Hypertension and Cardiology since it quantifies values in a range of reference [25]. In this classification system, each variable performs as an independent characteristic, where the A variable, by definition has a non-modifiable character (related to cure); B and C variables give prognostic factors, depending upon the quantity or severity, with the connotation the these can be intervened and are therefore modifiable. At the moment this classification does not assume to be cumulatively numerical since we do not know which of the factors are influencing to a greater or lesser degree. Therefore, we have an ABC classification with numerical sub-indexes which will determine the degree of alteration in each of the parameters measured. A greater numeric value of each variable indicates greater alteration of the parameter measured and vice versa; in the case of the two modifiable factors (proteinuria and high blood pressure), their value will be related to a greater or lesser probability of progression toward a more advanced form of CKD. This risk has not yet been defined since no clinical studies exist of relative risks for each of these values interrelating together [26].
Since blood pressure below the physiological level or the presence of isolated systolic high blood pressure have shown important clinical implications, the C variable can include sub-indexes 0 referring to blood pressure<120/80 mm/Hg [27] or 6 for isolated systolic high blood pressure (blood pressure: ≥ 140/<90 mm/Hg), where 0 and 6 does not mean a numerical value but if a variable in the classification, which will be of great utility in the development of future clinical research studies [28].
This new classification (Table 1) besides being a diagnostic instrument and having the character of progression prediction is useful to us as a quantitative parameter for therapeutic success or failure, conceptually recognized, but apparently little applied in clinical practice.
Table 1: New ABC Chronic Kidney Disease Classification
In this classification, each of the patient’s three variables is compared
with corresponding reference values to obtain an ABC classification, with
respective sub-indexes which indicate the level of each of the evaluated
parameters. To facilitate application, we will soon publish on the internet
the application CKD ABC CALCULATOR, as shown in Figure 1, which
will permit one to enter the evaluation parameters and obtain the
corresponding classification for example, patient with GFR: 100 mL/min
1.72 m2, proteinuria: 4500 mg/24h, Blood Pressure: 145/94mm/Hg, its
classification will be as shown in figure 1.
Figure 1: CKD ABC CALCULATOR
It means that the patient classified as A1-B5-C3, have preserved renal function, their proteinuria is severe and the blood pressure is high, therefore must be give treatment for the proteinuria triggering factor and optimizing treatment to high blood pressure. As we can see there is more information that with current CKD classification with which the concept is more whole and the treatment is focused in specific targets.
In general terms Table 2 summarizes the principal similarities and differences between the KDIGO 2012 classification and the one proposed here.
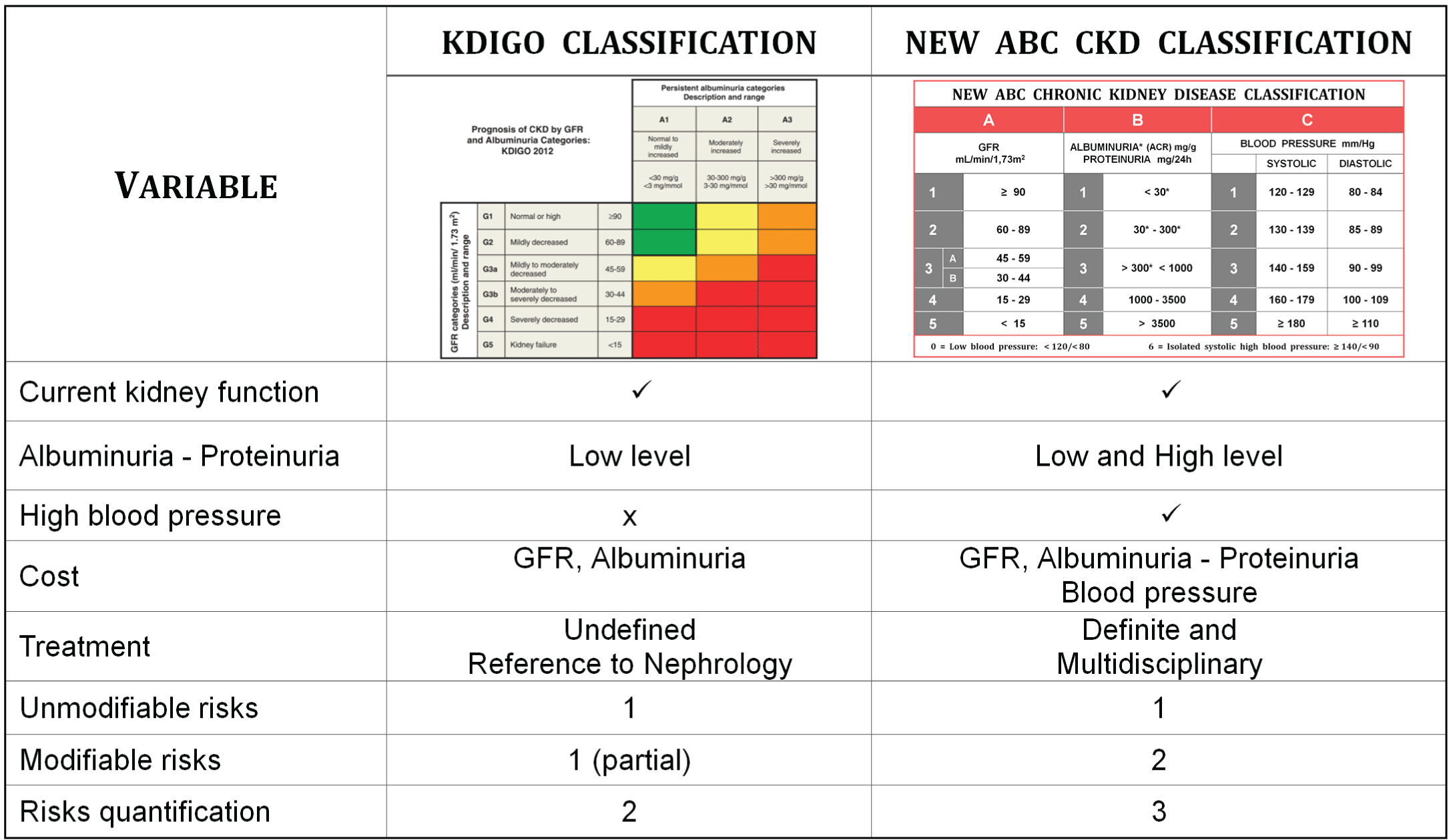
Table 2: Differences and similarities between KDIGO 2012 and the new ABC CKD classification
We recommend following the respective guidelines of clinical management existing for each variable, optimizing the control of the modifiable (proteinuria and high blood pressure) since by definition GFR only permits maintaining or diminishing speed of progression; an added advantage of this classification is that it facilitates therapeutic decisions because the diagnostic parameters are very clear and the management directives have already been established. This permits application in all levels of health attention without waiting for specialized medical remission; it also allows determination of therapy success or failure since follow-up is carried out based upon quantitative variables [29].
Finally, this new classification identifies the priority of attention and also orients the management of health resources for those in need, which are those with a more advanced disease, greater proteinuria, and high blood pressure.
As a starting point, we propose future prospective studies to validate their usefulness, clinical correlation, and statistical significance, of which we have some of them in the course and soon we will publish it their outcomes.
This new way of combining the factor that identifies the presence of chronic kidney disease (CKD) with the two factors that largely determine its prognosis, is a new way to have a much more comprehensive concept of the disease, which, by to have quantifiable prognostic risks factors, it will allow establishing a better and objective therapeutic strategy.
The authors declare that there is no conflict of interest regarding the publication of this paper.
Download Provisional PDF Here
Article Type: Opinion Article
Citation: Jojoa JA, Rivera CE, Delgado EM, Casas HM, Rosas GM, et al. (2017) New ABC Chronic Kidney Disease Classification. Int J Nephrol Kidney Failure 3(2): doi http://dx.doi.org/10.16966/2380-5498.144
Copyright: Jojoa JA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access