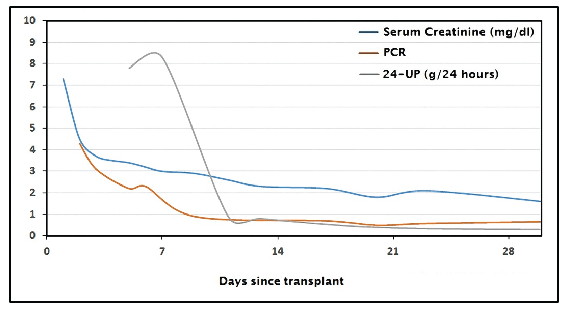
Figure 1: Trend of serum creatinine, PCR and 24-UP over the first 30 days post-transplant


Alejandra Mena-Gutierrez1* Ravinder Pal S Bhatti2 Lakshmi P Nadimpalli2 Sameh R Abul-Ezz2 Manisha Singh2
1Department of Medicine, Central Arkansas VA Healthcare System, USA*Corresponding author: Alejandra Mena-Gutierrez, McClellan Memorial VA Medical Center 4300 West 7th Street. Little Rock, USA, E-mail: alejandramenag@gmail.com
Urinary protein excretion is crucial to both diagnosis and treatment of many renal disorders as also critical for follow up of kidney allograft function after transplant. Random Urine Protein Creatinine Ratio (PCR) is commonly used to estimate proteinuria. However, there are concerns over diagnostic accuracy of PCR or its correlation with the extent of proteinuria noted on 24 hour urine collection (24–UP). We present a case of a 38 years old Caucasian man with history of end stage renal disease due to primary focal segmental glomerulosclerosis (FSGS). He underwent a deceased donor kidney transplant with immunosuppressive induction and maintenance per hospital protocol. His creatinine and proteinuria as measured by PCR improved progressively. With discharge planning underway, we tested a 24-UP. Unexpectedly, his 24 hour proteinuria was markedly higher than that suggested by the PCR calculated on a spot urine sample. A diagnosis of early recurrence of FSGS was made and the patient was successfully treated with plasmapheresis. In addition, his tacrolimus was changed to cyclosporine. We conclude that it is prudent to routinely monitor proteinuria by timed urine collection in the immediate post-transplant setting for recipients with primary FSGS to avoid delays on appropriate therapy that could impact graft function and survival.
Proteinuria; Protein creatinine ratio; 24 hour urine protein measurement; Focal and segmental glomerulosclerosis; Post-transplant recurrence
PCR: Protein Creatinine Ratio; 24-UP: 24 hour Urine Protein measurement; ACR: Albumin to Creatinine Ratio; FSGS: Focal Segmental Glomerulosclerosis.
Proteinuria is an early marker of inflammation and renal disease and predictor of allograft dysfunction after kidney transplant [1].Timed urine collection is considered the gold standard to measure proteinuria and albuminuria [2]. However, random Urine Protein Creatinine Ratio (PCR) is commonly used to estimate proteinuria and has increasingly replaced 24 hour urine protein measurement (24-UP) in clinical practice. This is attributed to considerations of simplicity, convenience, time and cost. Current literature also favors its use on the basis of significant correlation with 24 hour protein excretion, with an acceptable profile in terms of sensitivity and specificity and the improving global outcomes. Clinical Practice Guideline for Evaluation and Management of Chronic Kidney Disease published in 2012 suggest using urine Albumin to Creatinine Ratio (ACR) or PCR as initial testing for proteinuria [3].
However, there are concerns regarding the diagnostic accuracy of PCR and reliability, particularly at higher degrees of proteinuria [4]. Utility of PCR is also diminished in the immediate post-transplant period when GFR is not stable and rate of creatinine excretion is variable.
We present a case of an early recurrence of Focal Segmental Glomerulosclerosis (FSGS) in a renal transplant recipient where timely intervention could have been delayed unless 24 hour urine protein excretion quantification was utilized instead of PCR.
A 38 years old Caucasianman, with a past medical history of hypertension and end stage renal disease secondary to Focal Segmental Glomerulosclerosis (FSGS). He was diagnosed in 2004 and treated with Cyclophosphamide, Cyclosporine and steroids at that time with no sustained response, eventually leading to ESRD. Patient had been on peritoneal dialysis for over four years prior to transplant and had been an uric for one year prior to transplant. He was admitted for a deceased donor kidney transplant at our hospital.
Family history was notable for his father having coronary artery disease and hypertension prior to death by accident, mother having diabetes and elder brother having hypertension.
He was seropositive for Cytomegalovirus (CMV) and seronegative for Epstein Barr Virus (EBV). His calculated panel reactive antibody was zero percent. Initial evaluation showed BMI 31. He had a serum creatinine of 7.3 mg/dl and blood urea nitrogen of 52 mg/dl.
The donor was standard criteria donor, a 23 year-old Caucasian man who suffered brain death following a gunshot wound. His initial and peak serum creatinine had been 1.0 mg/dl and final creatinine was 0.7 mg/dl. He was seropositive for both CMV and EBV
Induction was carried out using Basiliximab, Methylprednisone and Mycophenolate Mofetil (MMF). He was transitioned to maintenance immunosuppression with Tacrolimus, MMF and Prednisone along with infection prophylaxis per protocol over the next few days.
Our patient had been a uric prior to transplant therefore we had no baseline proteinuria. His creatinine and proteinuria as measured by PCR on a random urine specimen, improved progressively. Serum creatinine was 7.3 mg/dl and PCR was 1.1 post-transplant day 1, reaching 3.4 mg/dl and 2.2 respectively by day 5 (Figure 1).

Figure 1: Trend of serum creatinine, PCR and 24-UP over the first 30 days post-transplant
With discharge planning underway, we decided to check 24-UPand unexpectedly, his 24 hour proteinuria was noted to be markedly higher than that suggested by the PCR, being 7.8 grams (Table 1).
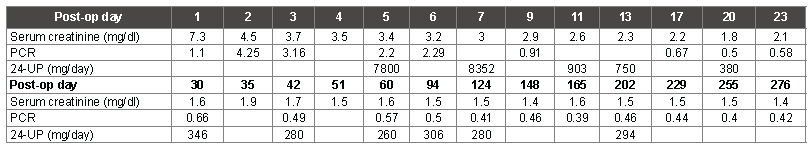
Table 1: Changes in serum creatinine, PCR and 24-UP over the first nine months post-transplant
A presumptive diagnosis of early recurrence of FSGS was made. An allograft biopsy was withheld to avoid delay in timely management and due to high risk of bleeding with plasmapheresis which was immediately initiated. Additionally, his Tacrolimus was changed to Cyclosporine (CsA) since plasmapheresis and high doses of CsA remain the mainstays of therapy per current literature. For follow-up, both PCR and 24-UP were monitored.
The patient responded well to treatment with plasmapheresis alone, achieving partial remission by the fourth session and complete remission by five weeks. At that time, serum creatinine was down to 1.6 mg/dl and 24-UP had decreased to 280 mg/24 hours, PCR was 0.13. Plasmapheresis was then stopped. He continued maintenance immunosuppression with Prednisone, MMF and Cyclosporine and remained in remission upon follow-up at 6 months.
Convenience and logistical considerations have led to PCR being increasingly used in assessment of proteinuria. PCR has shown to have acceptable correlation with 24-UP and also good sensitivity and specificity among transplant recipients. Although, the validity of random urine protein measurements remains unclear in this particular population and further randomized trials are needed [5]. Therefore, caution is advised when using this test for follow up in the immediate post-transplant setting.
The ability of PCR to accurately predict 24-UP has been shown to be modest at higher levels of proteinuria. Additionally, as in the case of acute kidney injury, the immediate post-transplant period is not a steady state for creatinine excretion which limits the utility of PCR. The correlation is also effected by body mass index and muscle mass. In this particular case the difference between level of protein excretion by PCR and 24-UP is statistically significant in the initial post-transplant period (P=0.025) (figure 2). There are not enough data to valuate correlation since treatment was promptly initiated and level of proteinuria declined appropriately along with improvement on renal allograft function.
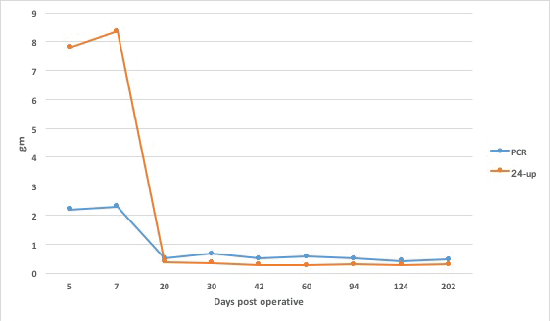
Figure 2: Protein excretion by PCR and 24-UP post renal transplant
Underestimation of proteinuria by PCR as allograft function is established can be avoided by testing PCR only after the serum creatinine has reached a plateau. Initial improving numbers can falsely lead to a sense of security regarding recovery of the patient. Such an approach can prevent the timely recognition of rising proteinuria, which may be the earliest clue to allograft dysfunction and is associated with transplant loss and mortality [2].
The clinical picture is sometimes obscured by other problems that may be going on simultaneously. Early post-transplant proteinuria in a patient with residual native kidney function can mislead the assessment of allograft dysfunction and often prompts to further work up including an allograft biopsy. However, proteinuria originating from native kidneys usually declines precipitously in the first few weeks after transplant, even in those with high levels of proteinuria. Thus, persistent or worsening proteinuria during this period can be considered to be of allograft origin, indicating and justifying additional diagnostic testing.
This case highlights the marked discordance between the degree of proteinuria measured by PCR and 24-UP in the early post-operative period of a patient with primary FSGS. Detecting this allowed us to make a timely decision regarding the patient’s management.
Based on this experience we conclude that UPC may not be an accurate measure in the early post-transplant period to monitor patients at risk for FSGS recurrence. Current literature supports the use of PCR as a screening test due to high level of sensitivity but should be used with caution to monitor response to treatment or to guide major clinical decisions.
It is prudent to routinely monitor proteinuria by timed urine collection in the immediate post-transplant setting, more so on recipients with primary FSGS until renal function and protein excretion has stabilized. Revision of the current guidelines may be necessary in this particular clinical setting if findings are confirmed on a larger cohort of patients. Randomized trials are needed in transplanted patients and also in nontransplant populations with FSGS.
Download Provisional PDF Here
Article Type: Case Report
Citation: Mena-Gutierrez A, Bhatti RPS, Nadimpalli LP, Abul-Ezz SR, Singh M (2016) Post Renal Transplant Follow Up in Focal Segmental Glomerulosclerosis with 24 Hour Urine Protein Collection - Traditional and True. Int J Nephrol Kidney Failure 2(4): doi http://dx.doi.org/10.16966/2380-5498.134
Copyright: © 2016 Mena-Gutierrez A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access