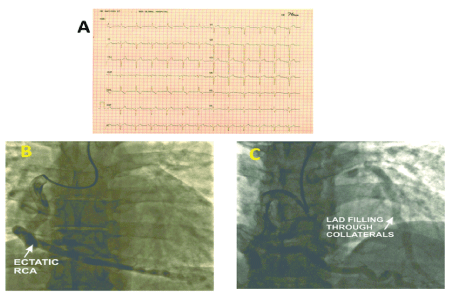
Figure 1: A -Electrocardiogram (ECG); B, C - Coronary Angiogram; RCA – Right Coronary Artery; LAD – Left Anterior Descending Artery.


Maruti HY1* Nareppa U1 Bhaskar BV1 Sharma G2 Shivaprakash S3 Hittalamani S3
1Department of Cardio-Thoracic and Vascular Surgery, BGS Global Hospital, Bengaluru, Karnataka, India*Corresponding author: Maruti HY, Department of Cardio-Thoracic and Vascular Surgery, BGS Health and Education city, #67, Uttarahalli Road, Kengeri, Bangalore-560060, Karnataka, India, Tel: +91 9900972599; E-mail: marusurg@gmail.com
Bland–White–Garland syndrome (ALCAPA) is one of the congenital coronary artery anomalies. Majority of cases present in infancy, however, few patients survive to adulthood. It can present as effort angina due to relative ischemia and coronary steal, and can cause diagnostic dilemma. It is important to be aware of this potentially lethal condition to prevent life threatening complications. We present a 34-year old male, who presented with atypical chest pain and was found to have ALCAPA on evaluation, and underwent successful surgical correction
Bland–White–Garland syndrome; Coronary artery anomalies; Collateral circulation
Bland–White–Garland syndrome or Anomalous origin of the left coronary artery from the pulmonary artery (ALCAPA) is a rare congenital coronary anomaly with an incidence of 1 in 300,000 live births (0.25- 0.5%).
Nearly 90% cases present within the first year of life due to myocardial ischemia and infarction or mitral regurgitation with congestive cardiac failure. However, few patients survive to adulthood because of adequate collateral blood supply to the left coronary circulation through the dominant right coronary artery [1].
They may present with dyspnea and exercise intolerance, severe heart failure, mitral valve insufficiency, angina or arrhythmias generated from myocardial scar tissue [2]. There are only few case reports of ALCAPA surviving into adulthood but without any LV (Left ventricular) dysfunction [3].
We present a case of Bland–White–Garland syndrome, presented as an ischemic heart disease in a young adult, managed successfully.
A 34-years-old male presented with atypical chest pain since two years, which was insidious in onset. There was a history of coronary artery disease in the family (Mother had undergone CABG at 55 years). He had no other cardiac risk factors.
His clinical examination, cardiac biomarkers and laboratory investigations were within normal limits. ECG showed normal sinus rhythm with left axis deviation, poor “R” wave progression in precordial leads and “T” wave inversion in leads I and a VL (Figure 1A).

Figure 1: A -Electrocardiogram (ECG); B, C - Coronary Angiogram; RCA – Right Coronary Artery; LAD – Left Anterior Descending Artery.
Treadmill Stress Test (TMT) was negative at 10 METS. 2D Echo revealed akinetic and thinned out antero lateral segments of the left ventricle with normal left ventricular dimensions and ejection fraction (LV EF) of 40%, no MR. Also, origin of ectatic right coronary artery (RCA) was visualized.
Conventional Coronary Angiogram showed ectatic RCA arising from the right coronary sinus and filling retrogradely the left coronary artery (LCA) (Figure1B and 1C). There was no evidence of any lesion in the coronary arteries.
Computed tomographic (CT) coronary angiogram with 3D reconstruction showed ectatic RCA arising from the right coronary sinus and the LCA arising from the ostium which was located in the adjacent segment of the PA, next to the Aorta (Figure 2).
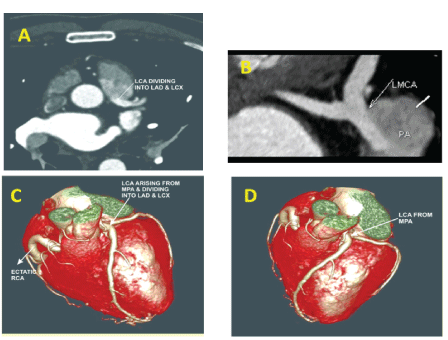
Figure 2: A, B - CT Coronary Angiogram ; C, D - CT Coronary Angiogram with 3D reconstruction; LCA- Left Coronary Artery; LMCA - Left Main Coronary Artery; PA - Pulmonary Artery; RCA - Right Coronary Artery; LAD - Left Anterior Descending Artery; LCX - Left Circumflex Artery; MPA - Main Pulmonary Artery.
Cardiac Magnetic Resonance (MR) imaging (Figure 3A and B) demonstrated thinning of anterolateral wall of the left ventricle with sub endocardial delayed Gadolinium enhancement.
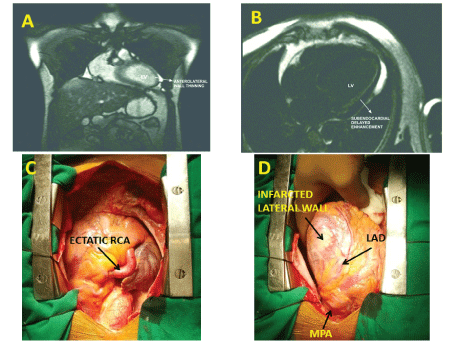
Figure 3: A, B - Cardiac MR Scan; C, D - Intraoperative pictures; RCA - Right Coronary Artery; LAD - Left Anterior Descending Artery; MPA - Main Pulmonary Artery.
A diagnosis of Bland–White–Garland (ALCAPA) syndrome was made and patient was taken up for surgery.
Examination of the heart revealed ectatic RCA and LAD arising from the left sided Pulmonary Artery (MPA) with a thrill over it (Figure 3C and D). Under Cardiopulmonary bypass (CPB) origin of the Left coronary artery (LCA) within the MPA was closed with a small autologous pericardial patch using 6-0 polypropylene continuous suture. This was followed by LIMA –RIMA“Y” anastomosis, and LIMA- LAD and RIMA - OM grafting.
Patient came off CPB in sinus rhythm with minimal inotropic supports. Perioperative period was uneventful. The patient was discharged home on postoperative day five. At one month follow up, patient is doing well and LV EF was 48% and no MR.
The first detailed clinical description in conjunction with autopsy findings of ALCAPA was described by Bland et al. in 1933, so the anomaly is also called Bland-White-Garland syndrome [4].
Approximately 10-15% cases of ALCAPA survive to adulthood. There is an estimated 80-90% incidence of sudden death at a mean age of 35 years in this group.
Surgical correction is the current standard whenever the diagnosis is made, as the medical management is supportive and is not associated with any significant survival benefit.
The development of electrocardiographically gated multidetector CT angiography and MR imaging have increased the accuracy of the diagnosis.
Various surgical techniques for ALCAPA have been proposed, but current surgical approaches are aimed at creating a two-coronary system. This can be achieved via ligation of the anomalous artery in combination with a bypass graft (mammary artery or saphenous vein) or the Takeuchiprocedure [5], where an intrapulmonary tunnel from the aortopulmonary window to the coronary artery is created or direct reimplantation of the left main coronary onto aorta by a button technique [6]. In general, the mortality rate after dual coronary repair of ALCAPA has been reported to range from 0% to 16% [7].
Alixi-Meskishvili et al. [7] studied four adult patients with ALCAPA aged 27, 35, 54 and 60 years in whom clinical improvement was seen in all patients and concluded that patients with adult ALCAPA get benefit from surgical establishment of a two coronary system even at older age [8].
In our case, reimplantation technique or Takeuchi-procedure was technically difficult because of the position of Anomalous LCA.
Raghuram et al. [9] used polypropylene suture to close the opening of LCA within the MPA. We used autologous pericardial patch to close the opening of the LCA.
A young adult patient presenting with symptoms of ischemic heart disease, ALCAPA has to be considered in the differential diagnosis. The availability of non-invasive diagnostic modalities such as, multidetector CT Angiography and MR imaging have increased the diagnostic accuracy. Surgery is the gold standard treatment for ALCAPA and is aimed at restoring a two-coronary-artery system. Prompt treatment may prevent life threatening complications, such as myocardial infarction or sudden death.
None
Download Provisional PDF Here
Article Type: Case Report
Citation: Maruti HY (2018) Bland-White-GarlandSyndrome: A Rare Cause of Ischemic Heart Disease in A Young Adult. J Hear Health 4(1): doi http://dx.doi.org/10.16966/2379-769X.142
Copyright: © 2018 Maruti HY, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access