Abstract
A middle-aged woman with symptomatic paroxysmal atrial fibrillation refractory to pharmacological treatment was referred for catheter ablation.
During the procedure, a left atrial thrombus was visualized within the left atrium attached to a transseptal sheath. In our case we used a different
approach for extraction of thrombus.
Keywords
Catheter ablation; Intracardiac echocardiography; Transseptal catheterization; Intracardiac thrombus; Atrial fibrillation
Abbreviations
ACT: Activated Clotting Time; AF: Atrial Fibrillation; ICE: Intracardiac Echocardiography
Introduction
Cardioembolic events are one of the most serious complications during
atrial fibrillation (AF) ablation. According to studies with intracardiac
echocardiography, the incidence of thrombus associated with sheaths or
catheters is about 9-10% in left atrium ablation procedures [1], and up to
2% of systemic embolization has been observed [2]. Several strategies have
been published for extraction of thrombus including direct withdrawal of
the sheath [3] or vigorous aspiration of the thrombus [1]. We report a
case in which we used a different approach for extraction of a thrombus
attached to the distal tip of a sheath placed in the left atrium.
Case Report
A 41-year-old woman smoker with symptomatic paroxysmal AF
refractory to beta-blockers and flecainide was referred to our institution for
pulmonary vein ablation. She was not taking anticoagulants. Transthoracic
echocardiography showed normal ventricles and valves and a moderately
enlarged left atrium (45 × 52 mm). A preprocedural transesophageal
echocardiogram confirmed the absence of intraatrial thrombus.
Prior to the trans-septal puncture a bolus of 3000 IU of heparin was
administered. A first transseptal puncture was performed without difficulty
guided by ICE (AcuNav catheter, Siemens Medical Solutions, Mountain
View, CA, USA). An 8.5 F transseptal sheath (SL1, St. Jude Medical, St.
Paul, MN, USA) and a BRK1 puncture needle (St. Jude Medical) were
used. Immediately after puncture, a bolus of 5000 U of heparin was
administered. The sheath was continuously flushed with heparinized
saline (2 units/mL) at a rate of 30 mL/h . Approximately 5 minutes later
and before performing a second transseptal puncture, a mobile thrombus
attached to the distal tip of the sheath (0.9 cm long × 0.3 cm wide) was
observed (Figure A; Supplementary Video). An additional 6000 U of
heparin was administered obtaining an activated clotting time (ACT) of
288 s. Given the persistence of the thrombus after waiting 20 minutes, it
was attempted to aspirate it vigorously through the sheath but this was not
effective. Since the thrombus was strongly attached to the distal tip of the
sheath, it was decided to advance the dilator to trap the thrombus between
the dilator and the sheath. Dilator size was similar to the width of the
thrombus. This manoeuver involves some risk of thrombus embolization
and was performed under continuous monitoring with ICE with special
attention to cross the distal portion of the sheath. The dilator and sheath
were then withdrawn as a single unit allowing complete extraction of the
thrombus outside the patient (Figures B and C). After the four pulmonary
veins were successfully isolated under intense heparinization and ACT
values above 300. The intervention was completed without incidents and
the patient did not experience any cardioembolic complication in the
periprocedure .
Discussion
Thrombus formation during left atrial ablation procedures is relatively
common and the use of ICE plays a very important role in its early
detection, which is essential to adopt therapeutic measures. Possible
causes of thrombus formation include the presence of spontaneous echo
contrast; prothrombosis induced by the sheath or catheter itself, delayed
or insufficient heparinization, and vascular injury [4]. Several strategies
have been published for extraction of thrombus. One is direct aspiration
through the sheath [1] but in our case it was not effective, probably because
the thrombus was strongly attached to the distal end of the sheath. Another
technique is simple withdrawal of the sheath and thrombus as a single
unit. Ren et al. [3] used this technique for the extraction of 30 thrombus.
Of these, 27 were removed successfully to the right atrium and 2 remained
trapped in the interatrial septum. It should be noted that only 8 of the
30 thrombi were extracted outside the patient and the rest presumably
remained at the level of the venous system, suggesting a high percentage
of dislocation during the maneuver of simple withdrawal. Finally, some
cases of intraatrial thrombolysis have also been reported [5].
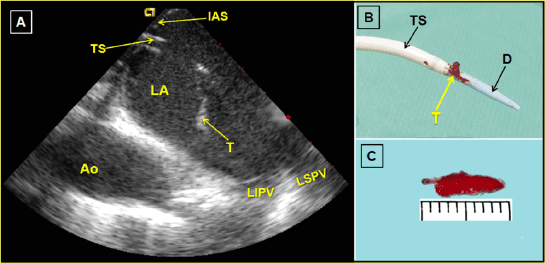
Figure 1: A-Intracardiac echocardiography image demonstrated a thrombus (T) attached at the transseptal sheath (TS) in the left atrium (LA).
IAS=Interatrial septum. Ao=Descending aorta. LIPV=Left inferior pulmonary vein. LSPV=Left superior pulmonary vein. B- Image showing thrombus (T)
between the transseptal sheath (TS) and dilator (D). C- Caliper thrombus size in millimeters
In our case, after the impossibility of aspirating the thrombus, we
considered simple withdrawal of the sheath and thrombus. However,
we thought there was a high risk of thrombus dislocation during this
maneuver either in its passage through the interatrial septum or through
the lower venous system. Thrombolysis was ruled out due to the high risk
of bleeding and thrombus fragmentation and embolism. Finally, we opted
to advance the dilator through the sheath to trap the thrombus between
the sheath and the dilator thus reducing the risk of thrombus dislocation
during the withdrawal maneuver. To our knowledge, this is the first
reported case using this modality of extraction.
Conclusion
Thrombus entrapment attached to transseptal sheath during atrial
fibrillation ablation guided by intracardiac echocardiography can be an
alternative when other thrombus extraction techniques have not been
successful.
Acknowledgement
This project was funded in part by Grant TIN2012–37546-C03-02 from
the Ministerio de Economía y Competitividad (Spain).
Download Provisional PDF Here
Article Information
Aritcle Type: Case Report
Citation: Doblado-Calatrava M, SánchezQuintana
D, Cruz JM, Vega CF, García-Guerrero
JJ, et al. (2015) Extraction by Entrapment of
a Thrombus attached to Transseptal Sheath
during Atrial Fibrillation Ablation guided by
Intracardiac Echocardiography. J Hear Health
1 (4): doi http://dx.doi.org/10.16966/2379-769X.117
Copyright: © 2015 Doblado-Calatrava M, et al.
This is an open-access article distributed under the
terms of the Creative Commons Attribution License,
which permits unrestricted use, distribution, and
reproduction in any medium, provided the original
author and source are credited.
Publication history:
Received date: 06 Nov 2015
Accepted date: 24
Nov 2015
Published date: 30 Nov 2015


