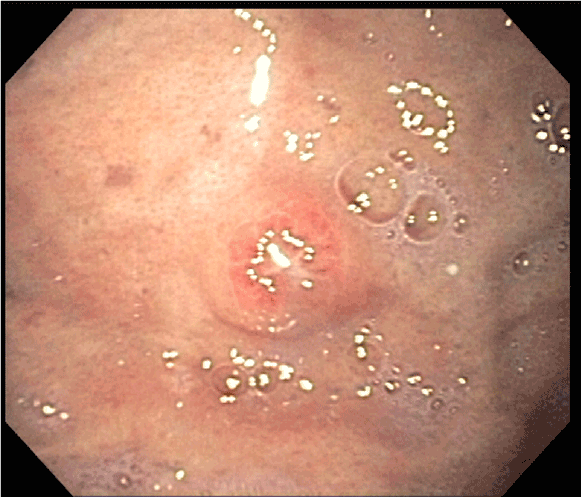
Figure 1: A single diminutive nodule with erosion in the gastric fundus.
Stephanie Judd1* Alyssa Liubakka2 Edi Levi3 Fadi Antaki1
1Division of Gastroenterology, Department of Internal Medicine, John D. Dingell VA Medical Center and Wayne State University School of Medicine, Detroit, Michigan, USA*Corresponding author: Stephanie Judd, Division of Gastroenterology, Department of Internal Medicine, John D. Dingell VA Medical Center and Wayne State University School of Medicine, Detroit, Michigan, USA, E-mail: E-mail: sjudd@med.wayne.edu
While upper GI bleeding from primary gastric tumors is relatively common, bleeding arising from metastatic foci is rare. Here we present a case of metastatic lung adenocarcinoma to the stomach presenting with upper GI bleeding.
A 57- year-old man with stage IIIB adenocarcinoma of the lung status post chemo radiation therapy presented with 5 days of melena and dizziness. Orthostatic hypotension was noted; physical examination was otherwise unremarkable. Laboratory evaluation showed nadir hemoglobin of 6.3 g/dL from a baseline of 11.9 g/dl. EGD revealed a small nodular lesion with erosion in the fundus (Figure 1). Forceps biopsies showed a focus of metastatic carcinoma associated with a lymphocytic infiltrate (Figures 2 and 3). Tumor cells stained positive for p63 and negative for TTF-1, consistent with metastatic non-small cell lung cancer (Figures 4 and 5). Hemoglobin improved after blood transfusion, and he had no recurrence of gastrointestinal bleeding. Given rapid disease progression with brain metastasis, he was discharged with home hospice.
Gastric metastasis from lung cancer is rare with an incidence of 0.2%-0.5% [1]. As in our case, the most common type of lung cancer to metastasize to the stomach is non-small cell with the usual sites of metastasis being the fundus and cardia [2]. Metastatic lesions to the stomach are difficult to diagnose endoscopically. The classic “bull’s eye sign,” which is a sub mucosal tumor with a central depression, is found in only 44% of cases [3]. Multiple lesions are seen in up to one third of cases [3]. Diagnosis is usually confirmed by endoscopic biopsy [3]. As in our case, the majority of non-small cell carcinomas express p63 [4]. Thyroid transcription factor 1 (TTF-1), an immune histochemical marker, is often used to confirm primary lung cancer. Its specificity is approximately 90% with a positive predictive value of 83%; however, the sensitivity is only approximately 60-82%and, as in this case, can be even lower in previously treated lung carcinomas [3,5-7]. In addition to TTF-1, cytokeratin 7 (CK7) and cytokeratin 20 (CK20) have been used to distinguish primary from metastatic lung adenocarcinoma [8]. CK7 expression appears to be more frequent in adenocarcinomas originating from a pulmonary primary with CK20 expression more common in adenocarcinoma originating from the GI tract [8]. Our case demonstrates that stomach metastasis, though rare, should be considered in individuals with primary lung cancer presenting with upper GI bleeding. Immunohistochemical markers, in addition to endoscopic clues, can be helpful in distinguishing primary versus metastatic lung carcinoma.

Figure 1: A single diminutive nodule with erosion in the gastric fundus.
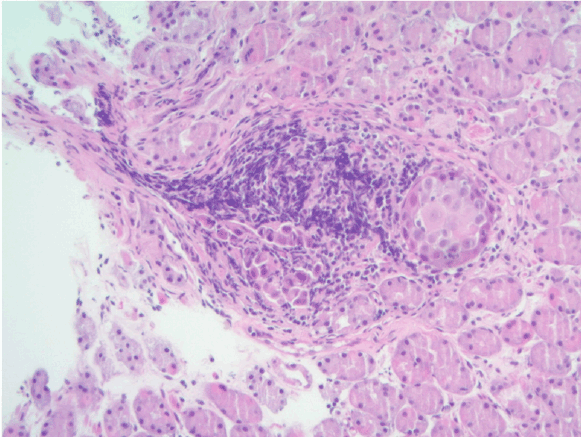
Figure 2: Low power image showing tumor nests associated with a lymphocytic infiltrate (H&E, original magnification, × 200)
This material is the result of work supported with resources and the use of facilities at the John D. Dingell VAMC, Detroit, Michigan. The content does not represent the views of the Department of Veterans Affairs or the United States Government.
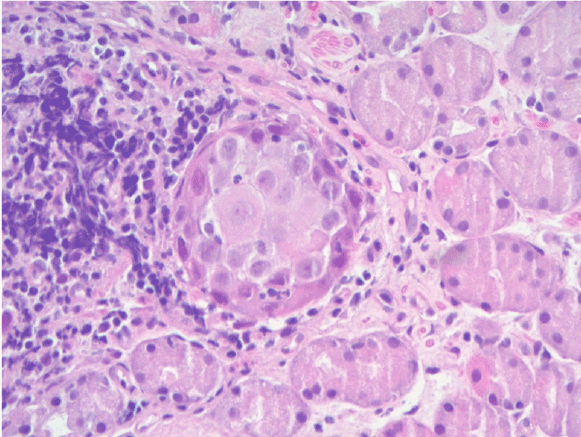
Figure 3: High power image showing tumor nests with prominent nuclei and nucleoli with intracellular bridges surrounded by normal fundic glands (H&E, original magnification, × 400).
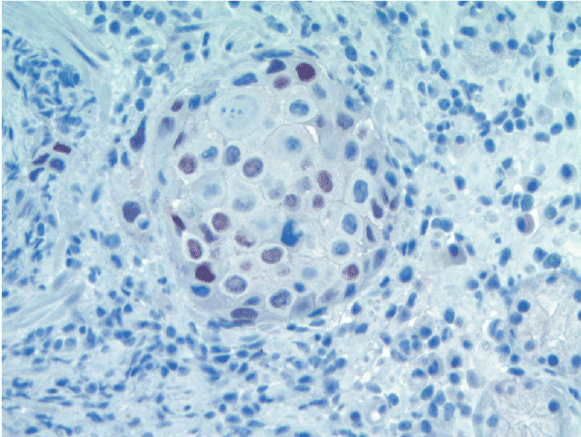
Figure 4: Immuno histochemical staining for p63 is positive (brown) (× 400).
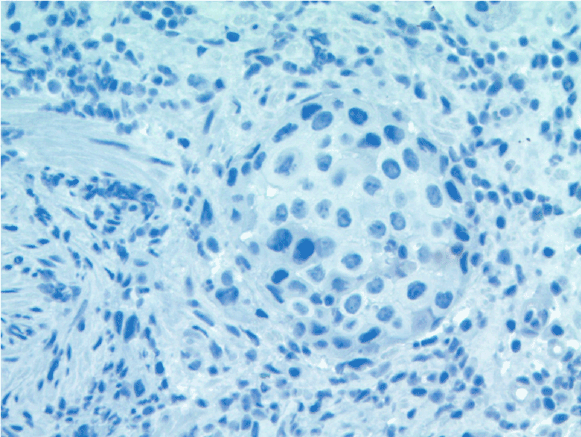
Figure 5: Immuno histochemical staining for TTF-1 is negative (× 400).
None of the authors have any commercial association that might represent a conflict of interest in relation to the submitted manuscript.
None
Download Provisional PDF Here
Aritcle Type: Case Report
Citation: Judd S, Liubakka A, Levi E, Antaki F (2015) A Rare Cause of Upper GI Bleeding: Gastric Metastasis from a Primary Lung Cancer. J Gastric Disord Ther 1 (2): doi http://dx.doi. org/10.16966/2381-8689.106
Copyright: © 2015 Judd S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access