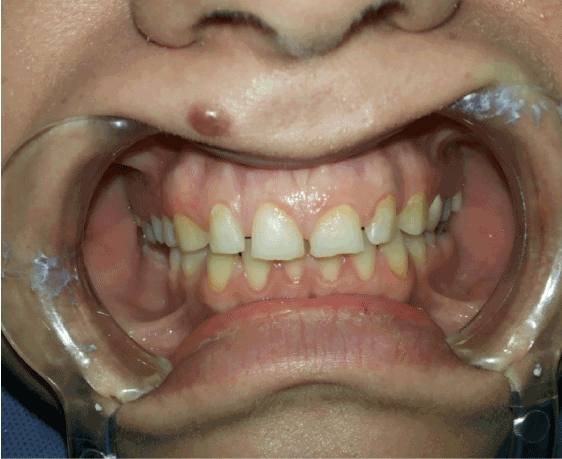
Figure 1: Diagnostic photo illustrating upper teeth Diastema

Raghad Al-Halabi1 Khaldon Al-Hroob1 Aous Dannan*,2 Talal Al-Nahlawi3 Hiba Abd Al-Aal3
1Fifth class undergraduate student, Faculty of Dentistry, Syrian Private University, Damascus, Syria*Corresponding author: Dr. Aous Dannan, Lecturer in Periodontics, Department of Periodontics, Faculty of Dentistry, Syrian Private University, Damascus, Syria; E-mail: aousdannan@yahoo.com
Indirect laminate veneer restorations provide a valid conservative alternative to complete teeth coverage (full crown) as they avoid aggressive dental preparation; thus, maintaining tooth structure.
The increased practice of veneering technique with indirect composites is due to improvement in the properties of composite materials in the last years.
This case report describes using indirect composite laminate veneer technique for a patient with esthetic problem related to generalized diastema in the upper anterior teeth. Starting with esthetic gingivectomy and ending up with laminate veneers being bonded on the teeth, a complete satisfying result was achieved. However, with no follow-up documentation yet.
Indirect composite laminate veneer restorations due to polymerization outside of the oral cavity, and thus being less affected by the fluids of the oral cavity with reduced effect of polymerization shrinkage and improved mechanical properties, are superior to direct composite veneers, and could give satisfying esthetic results. Maintaining good oral hygiene should always be advised to patients with such laminate veneers in order to keep prolonged esthetic results.
Veneers; Indirect composite; Gingivectomy; Diastema
For several years, aesthetically satisfying results in the reconstruction of anterior teeth have been achieved with full crowns. However, this treatment option is highly destructive as large amounts of sound tooth structure are sacrificed [1-3].
With the introduction of adhesive systems, more conservative treatment options have emerged. One of the most minimally invasive techniques is the application of laminate veneers made of either ceramics or particulate filler composites [4]. Composite laminate veneers, whether direct or indirect, provide other advantages over ceramic restorations including relatively low cost, inherently less brittleness, and, to a certain extent, easy to repair. The final quality of the restoration can be influenced by factors such as light-curing method and exposure time, type of indirect restorative material, and also by the luting agent [5, 6].
The increased practice of veneering technique with indirect composites is due to improvement in the properties of composite materials in the last years. These new composites have a volume percentage of inorganic ceramic fillers of approximately 66 % which result into improved mechanical properties with a flexural strength between 120 and 160 Megapascal (MPa) and an elastic modulus of 8.5 -12 Gigapascals (GPa) [7].In this case report, indirect composite laminate veneer technique used for a patient with esthetic problem related to generalized upper anterior teeth diastema is described.
A 28-year-old female patient visited the clinics of the Faculty of Dentistry of the Syrian Private University in Damascus complaining of esthetic problem related to a generalized diastema (spaces) in the upper jaw from right to leftcanine caused by size incompatibility between teeth and jaw (Figure 1).
Several solutions were discussed with the patient such as orthodontic treatment, which the patient refused, porcelain veneers, which were considered expensive to her, porcelain crowns, but they were no conservative, and direct composite veneers, which the patient refused due to her inability to keep the mouth opened for too long during treatment. Finally, the patient agreed to get the esthetic problem solved with indirect composite laminate veneers.
As a first step, and after teeth dimensions measurement and to achieve correct 75-80 % width to length ratio after diastema closure, esthetic gingivectomy was achieved on the centrals and canines (2mm each) to improve the final aesthetic result. No gingivectomy was done at the laterals due to the normal position and level of the gingival margins. All gingival sulcus depths were within the normal values (1-3mm) expressing a healthy non-inflamed gingival tissues. This procedure was achieved by means of a #15 scalpel starting with a 45 degree of inclination toward the gingival surface at each tooth to re-shape the marginal contour of the free gingiva, under local anesthesia (Lidocaine 2 % with Adrenaline 1/80000, Adrecaine, Syria) using the infiltration technique at each location. Aiming at re-contouring the gingival margins for better appearance (Figure 2).

Figure 1: Diagnostic photo illustrating upper teeth Diastema
10 Days later…after cleaning and shade determination of the teeth, the preparation began. The outline form included preparing all of the facial surface, extending approximately 0.5 to 1 mm cervical to the gingival tissue level and into the facial embrasures. The teeth were prepared with a coarse, tapered, rounded-end diamond by removing approximately one half of the enamel thickness (0.3 mm in the gingival region to 0.75 mm in the mid-facial and incisal regions, along with reducing the incisive edge to about 1 mm, and then impression was taken after retraction cord application (GINGI-PAK 00) using condensational silicon materials (Protesil Putty and Light condensation silicon) (Figures 3, 4). A temporary prosthesis was done directly with the aid of the preoperative impression and acrylic paste (direct layer of composite resin).
After making a cast for the prepared teeth, waxing up the veneers was done on that cast and then a silicon key was made to be used in building up the incisal edges of composite veneers (Figure 5). On the cast and after isolation with silicate, a gingival shade (Dentin composite #A2) (Composite Tetric-n-Ceram, IvoclarVivadent, USA) was applied with a hand instrument trying to cover the gingival third of the tooth properly. The gingival shade of the composite is feathered out at the middle third, smoothed, and cured. Next, the incisal shade (Enamel composite / translucent) (ICE restorative system SDI, Australia) was blended over the middle third and onto the incisal area to obtain proper contour and color. The facial contour is evaluated by inspecting from an incisal view with a mirror before the composite was polymerized by LED light for 20 seconds for each layer using with intensity of 850 mw/cm2 . General contouring was done at that point, but final finishing was delayed until all six veneers had been in place (Figure 6).
After building up the veneers, they were put in boiling water for 5 minutes to increase the degree of conversion. On the patient, a matrix was placed between every tooth being treated and its neighboring one. Etching the teeth surfaces was achieved by means of Phosphoric acid 37% (PrimeDent, USA) for 15 seconds. Teeth were then rinsed for 30 seconds with syringe water, and dried. A small brush was used to apply the bonding agents (Bonding resin , Prime-Dent,USA) in a very thin layer without curing (Figure 7).
The veneers were prepared by etching their inner surface using Hydrofluoric acid 10 % (Condacporcelana / FGM, Brazil) for 1 minute then rinsing for 30 seconds and drying. A thin layer of silant agents (SILANO Prosil / FGM, Brazil) were applied on the veneers and left for 1 minute and then dried with water and oil free air stream.
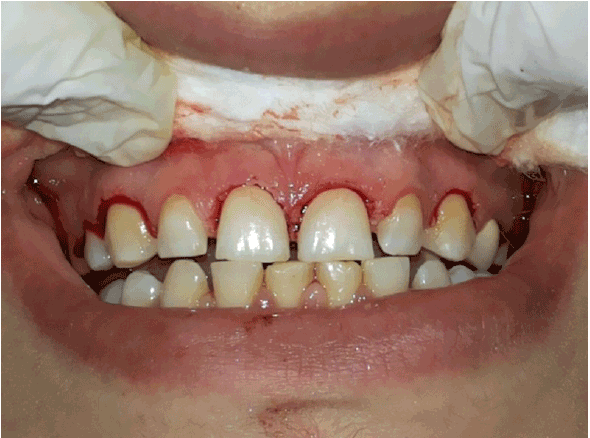
Figure 2: Gingivectomy on the upper centrals and canines
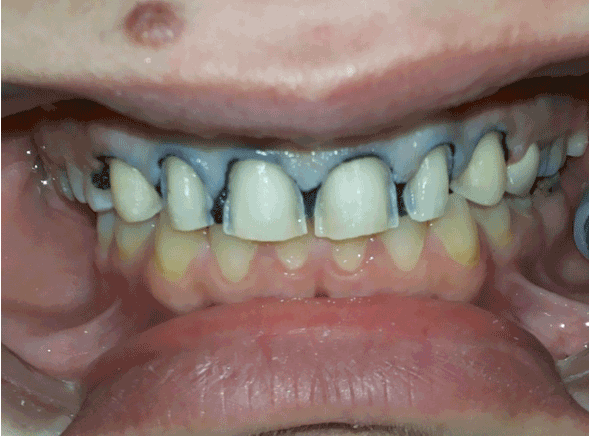
Figure 3: Preparation of teeth surfaces
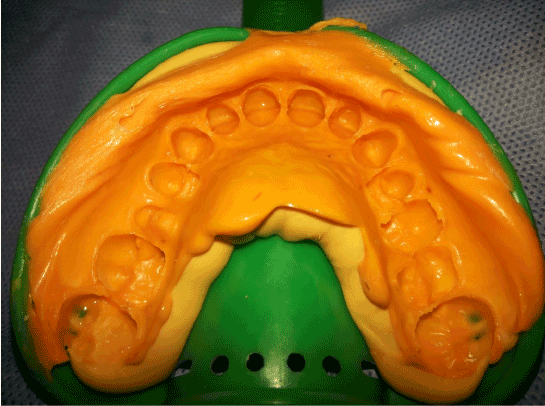
Figure 4: Impression was taken using condensational silicon material
The light-cured or dual-cured resin cement (Metacem resin cement / META) was mixed up and was put onto the veneers and then applied gently over the teeth followed by light curing from a 5 cm-distance for 5 second primarily to simplify the removal of cement residuals. Thereafter, each veneer laminate was cured for 40 seconds to get the final cured of the resin cement. Finally all extra residuals of the resin were removed, and composite finishing burs were used as well as Aluminum Oxide powder on a rubber bur to finish and smoothen the surfaces of the composite veneers. The final result was satisfying for the patient from her esthetic point of view, especially after closing all spaces between the frontal teeth (Figure 8). Certain advices were given to the patient in order to maintain the veneers and gain some primary stability (e.g. soft diet for 3 days), as well as advices related to oral hygiene maintenance.
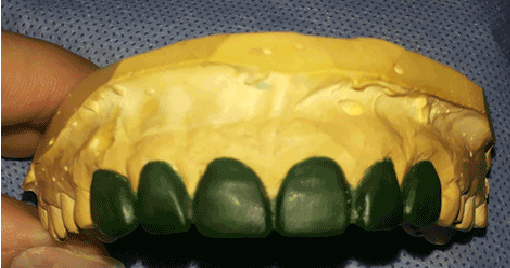
Figure 5: Waxing up the veneers
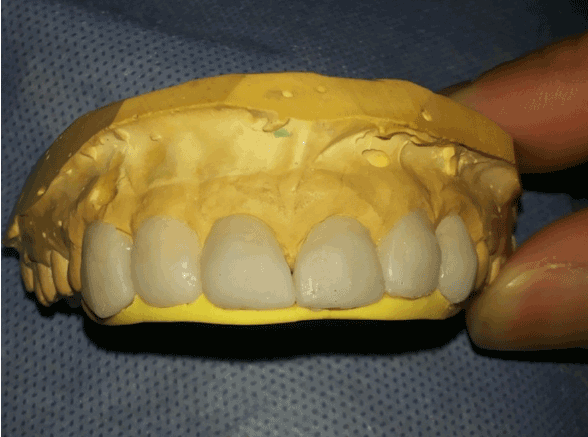
Figure 6: Building up the veneers extra-orally
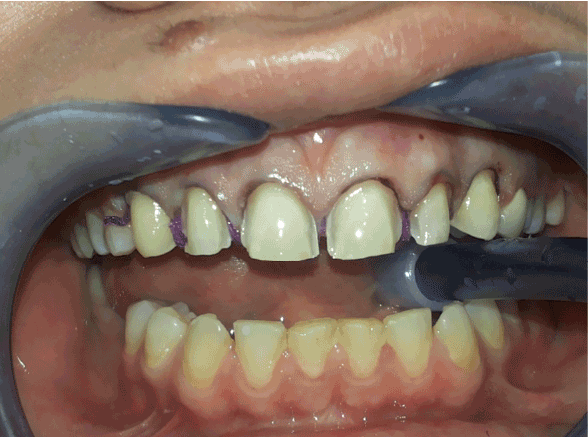
Figure 7: Preparing the teeth for veneer adhesion
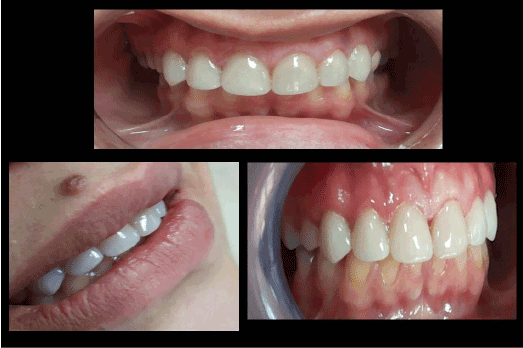
Figure 8: Final result
Today’s dentistry requires more conservative treatment options [8].Therefore, composite laminate veneer restorations, which require minimal removal of tooth structure, are one of the best treatment choices [8-10].With the advantages such as only one appointment for the whole treatment time, very low costs compared with the ceramics and no need for long laboratory procedures, direct composite laminate veneers are popular in today’s dentistry [11].
However, direct composite laminate restorations have still less resistance against abrasions and fractures compared with indirect composite laminate veneers and ceramic laminates [8, 12]. Furthermore, indirect composite laminate veneer restorations due to polymerization outside of the oral cavity, and ceramic laminate veneers due to better color stability because of being less affected by the fluids of the oral cavity, are superior to direct composite veneers [13].
In our case, in order to establish both functional and esthetic integrity, and considering more resistance and compressive strength than ceramics and similar abrasion rates compared with natural tooth structures, indirect composite laminate veneer restorations were considered. Fullceramic crown restorations were not considered because they result in excessive tooth structure loss as well as their high costs.
One of the first steps for achieving good esthetic results in our case was an esthetic gingivectomy. Traditionally, the physiologic gingival architecture has been described as having a scalloped contour [14] around the four surfaces of the tooth in accordance with the course of the cemento-enamel junction and thus, is concave apically in the free surfaces and convex occlusally at the tip of the papilla. Framing the teeth, within the confines of the gingival architecture, has a tremendous impact on the aesthetics of the smile. The impact on the beauty of a smile from an uneven gingival contour height can be dramatic and although the position of the zenith of the gingival tissue seems like a small detail, it can greatly influence the axial inclination and emergence profile of the teeth. These factors, some major and some minor, all add up to determine how pleasing the smile will be [15]. The instructions given to the patient in our case for maintaining good oral hygiene were important for a long-lasting esthetic results (e.g. gingivitis-free situation).Though the final result was satisfying for the patient, a follow-up is highly recommended.
With the development of new composite resins, indirect composite laminate veneer restorations can be a treatment option for patients with esthetic problems of anterior teeth, when applied with good patient’s oral hygiene motivation.
The indirect veneers have undergone considerable improvement and refinement over the past few decades, and have now matured into a predictable restorative concept in terms of longevity, periodontal response and patient satisfaction. These veneer restorations provide a valid conservative alternative to complete coverage as they avoid aggressive dental preparation; thus, maintaining tooth structure.
Download Provisional PDF Here
Aritcle Type: Case Report
Citation: Al-Halabi R, Al-Hroob K, Dannan A, AlNahlawi T, Abd Al-Aal H (2015) Indirect Composite Laminate Veneers for Upper Anterior Teeth Diastema Closure: A Case Report. Int J Dent Oral Health 1(4): doi http://dx.doi.org/10.16966/2378-7090.129
Copyright: © 2015 Al-Halabi R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access