
Figure 1: Clinical situation of the patient at the first visit, where the lack of implants can be observed in the posterior region of the mandible on the left side.

Rafael Manfro1* Vinícius Fabris2 Gislaine Felipe Garcia3 EstevoDerech Anderson Fernandes Felipe3 Marcelo Carlos Bortoluzzi4
1Chief, Departament Implantology, SOEBRÁS; ITI Fellow, Brazil*Corresponding author: Prof. Rafael Manfro, Presidente Coutinho 264/903, Florianópolis, Santa Catarina, 88015-230, Brazil, Tel: +55 48 32061410; E-mail: manfroimplante2@hotmail.com
The article presentsa case of mandible fracturecaused by the lossof an implantina protocolprosthesis increasingcantilever, causingbone lossaround the implant. The fracturewas treatedbyrigid fixation, fourimplantsanda new prosthesis. The authors discuss the possible causes and prevention of this complication.
Dental implants; Complications; Mandibular fractures; Clinical report
The use of protocol type osseointegrated implants and prostheses is the main treatment alternative for mandibular edentulous patients [1]. Despite the high rate of success [1-3], this treatment can present some complications with postoperative infection [4], sensorineural disorders, hemorrhaging [5], implant loss [2,3], fractures or loosening of the prosthesis [2,3] and more infrequently, mandibular fracture [4,6,7].
Mandibular fractures normally occur in women with atrophic mandibles in menopause [4,5,8-11].
The objective of this paper is to show a cast of late mandibular fracture, after 3 years of implant function, as a result of factors common to mandibular fractures treated by implants associated with biomechanical problems that occurred after a fracture of one of the implants.
Female patient, 47, who came to the Implantology department at SOEBRÁS-FLORIANÓPOLIS/SC complaining of pain in the more distal region of the implant, on the right side, and mobility in the prosthesis over the implants.
According to the patient, she was rehabilitated with a lower protocol, with 5 implants, 3 years before, after I year of function, there was a distal implant fracture on the left side.The professional responsible for treatment affirmed there would be no need to replace the implant or to conduct repairs on the prosthesis, which had an increase in the distal cantilever.
During the visit, an increase in volume was observed in the posterior region of the mandible on the right side and mobility in the region of the most distal implant, where it was impossible to diagnose whether the mobility was from the implant or resulting from the mandibular fracture (Figure 1). After the images were examined, a radiolucent line was observed beginning at the crest of the flap and continuing to the basal at the implant, characterizing a mandibular fracture without detachment of fragments. It was also possible to observe that this was a mandible with little bone height and the other implants revealed marginal bone loss with the exception of one (Figures 2 and 3).

Figure 1: Clinical situation of the patient at the first visit, where the lack of implants can be observed in the posterior region of the mandible on the left side.
Surgical treatment of the fracture was indicated with removal of 3 of the implants since they presented bone loss, clinical mobility and installation of new implants and new protocol type prosthesis.
The patient underwent general anesthesia and through an extra-oral access, the mandibular fracture was reduced and affixed with a straight plate and 2.4 mm fixation screws (Synthes-Oberdorf/Switzerland), previously individualized in a prototype model (Figures 4 and 5).
Using an intra-buccal incision, the implants were removed with the exception of the central implant which was in good clinical conditions. The fragment of the fractured implant was also removed.Three more 4.3 x 10 mm internal hexagon and Vulcano surface implants (Prosthesis Connection System – Arujá/SP-Brazil) were installed, in which the two distal implants had an inclination of about 450 as per the al-on 4 technique (Figure 6). The implant installed near the fracture region had little primary stability and for that reason it was decided to not use immediate load treatment.
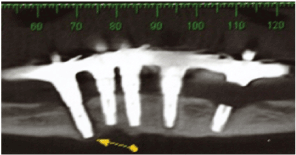
Figure 2: Tomographic cuts where the fractured implant can be observed on the left side of the mandible and the radiolucent peri-implant of the distal implant on the right side, suggesting mandibular fracture.
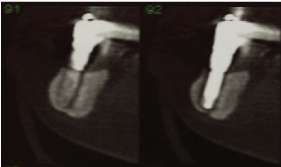
Figure 3: Tomographic cuts of the distal implant where the mandibular fracture can be confirmed without detachment.
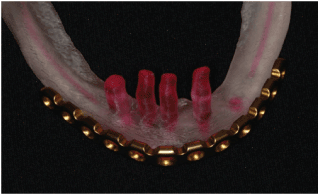
Figure 4: Prototype with the individualized reconstruction plate and the four remaining implants. The linear arrangement of implants compromising rehabilitation biomechanics can be observed.
The postoperative occurred without any intercurrences and after 60 days of osseointegration, a reopening was done with installation of 3 mm straight, metallic band micro-unit pillars (ConexãoSistema de Prótese – Arujá/SP-Brazil) and molded with a multifunctional guide.
After the prosthetic tests, a protocol-type prosthesis was installed with a metallic infrastructure cast in nickel-chrome, acrylic, artificial gingiva and acrylic teeth (Classic Heraeus-Kulzer/Germany).
Clinical controls were conducted after 15 days, when a new occlusal adjustment and check of screw torque was made.After 3, 6 and 9 months, clinical controls were conducted and after 12 months a clinical and radiograph control.In all these controls and images, clinical normalcy was observed (Figures 7 and 8).
The patient is currently under 15 months of control and the treatment conducted has proven successful this far
Mandibular fractures resulting from treatments with osseointegrated implants are rare [4,6,7] and normally are related to the installation of implants in mandibles with severe atrophy [4-11], where fixations penetrate the cortical basal region [4,7,10] and in women with menopause [5,7-10]. The fractures normally occur during installation of implants or the first days after surgery [4].
The authors believe that in the case presented in this paper, besides transfixing the fixations to the mandible, the distribution of force after fracture of one of the implants was fundamental for the occurrence of the fracture.
After the loss of the distal implant on the left side, prosthetic rehabilitation was anchored in 4 implants. Despite the positive results presented in literature in inferior protocols with four implants [2,3,12,13], the arrangement of the remaining implants resulted in a very big distal cantilever on the left side, since the last implant was in the region of the lower, lateral incisor and the polygon formed by the arrangement of the implants was also very unfavorable since they were in a linear position. Literature states the success of the protocols with 4 implants is directly tied to the positioning of the implants and the size of the cantilever [3,13,14].
The result of the rehabilitation force after loss of the implant caused excess force in the last implant on the right side, causing progressive, peri-implant bone resorption. Despite the patient’s complaints that the prosthesis presented mobility and pain at the site, this diagnosis was not conducted and since the prosthesis remained in use, bone resorption increased and reached the apex of the implant. Since it was transfixing the mandible, this progressive bone loss led to mandibular fracture in the implant position.
Treatment of atrophic mandibular fractures as a complication of the treatment with implants is a difficult task since multiple factors are involved [4,10]. The direction of the fracture line, detachment of the segment, use of the implants and type of access need to be carefully planned [4].
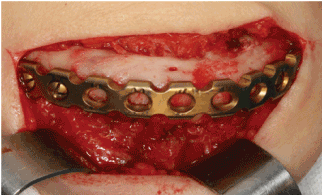
Figure 5: Surgical aspect of the extra-oral access, with the installed plate. In the region anterior to the mandible, screws were not placed to permit installation of the implants.
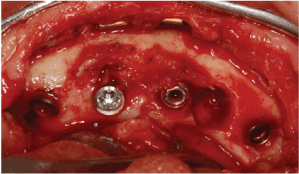
Figure 6: Implants installed and maintenance of one of the already existing ones.
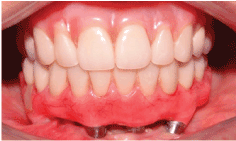
Figure 7: Clinical aspect showing the arrangement of the implants, reducing the cantilevers and the normal aspect of peri-implant soft tissue.
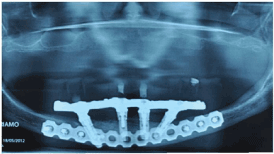
Figure 8: Control radiograph at 12 months where a situation of normalcy can be observed in fracture treatment and around the implants.a
The initial treatment option was the installation of new implants and rehabilitation of the patient in immediate load with ferrulization of implants through a cast metallic infrastructure in order to achieve an excellent fixation associated with the reconstruction plate affixed in the vestibular of the flap, while also favoring repair by early function.
Although there are fewer implants that in the original treatment, the distal implants were installed at an inclination, reducing the distal cantilever for both sides and increasing the resulting polygon between implants.
This case permits concluding that the arrangement of the implants is much more important than the number of fixations and is fundamental for the success of mandibular rehabilitations with protocol type prostheses.
Download Provisional PDF Here
Article Type: Case Report
Citation: Manfro R, Fabris V, Garcia GF, Derech E, Felipe AF, et al. (2015) Mandibular Fracture in A Patient Treated with A Protocol Prosthesis after 3 Years of Function due to Biomechanical Complications - Clinical Case Report. Int J Dent Oral Health 1 (2): doi http://dx.doi.org/10.16966/2378- 7090.112
Copyright: © 2015 Manfro R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Publication history:
All Sci Forschen Journals are Open Access