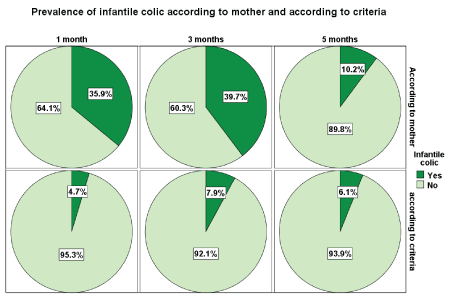
Figure 1: Pie charts of babies having infantile colic at 1, 3 and 5 month.

Muna Al Saadoon1* Syed Rizvi2 Ashfaq Khan1 Anwaar Khalifa Al Shuaili3 Maya Ali Al Mamari3
1Department of Child Health, Sultan Qaboos University, College of Medicine and Health Sciences, Muscat, Oman*Corresponding author: Muna Al Saadoon, Department of Child Health, Sultan Qaboos University, College of Medicine and Health Sciences, Oman, Tel: 00968 98882884; E-mail: salalah8484@hotmail.com
Infantile colic although is benign and self-limiting condition, it is distressing for both infants and care providers. Colicky babies cry from few minutes to hours per day, several days a week and last for weeks. The colic is more common among infants age 2 weeks to 4 months.
Aim: To assess the incidence of infantile colic among Omani infants, describe associated factors, mothers’ knowledge about infantile colic and common management methods used for the colic.
Methods: In this prospective cohort study, mothers who gave birth to healthy full term infants by vaginal delivery at the SQU hospital over the period (1 October- 31 December 2014) were invited to join the study. Those who accepted to participate signed written consent prior to data collection. Demographic data about the mother and family were collected from the mother after birth by self-completed questionnaire; Medical data was collected from the infant electronic medical records; data about the development of infantile colic were collected at the age of one month, three months and five months via telephone call using a structured questionnaire.
Results: Out of 64 infants only 49 have data up to the age of 5 months. A total of 7 babies (14.3%) satisfied the Wessel criteria for infantile colic when 25 babies (51%) were reported by the mothers to have this problem. The age at which the colic starts was found to range from 1-16 weeks and stops between the weeks 8-20 weeks (except for 2 babies, as at the time of completing the study were still having the infantile colic episodes). Some mothers expressed fears about their infant’s health and development due to infantile colic. Most mothers thought that their diet may affect infantile colic (69.2%) and some thought that their psychological state during pregnancy is related to infantile colic development (46.9%). No significant association was found between infantile colic and infants birth weight, order among siblings, sleeping pattern, feeding and defecation pattern. No statistically significant association was found between colicky and non-colicky infants according to family type, history of previous child with colic, mother’s age, working status and the family economic state.
Conclusions: The cumulative incidence rate for colic using the definition is far less than mother perception of the problem. According to this study, infantile colic is a common condition among Omani infants.
Infantile colic; Crying baby; Oman
One of the major distressing challenges of parenthood, especially the first timers, is an excessively crying baby [1]. Infantile colic, derived from the Greek word kolikos or kolon, is behavioral syndrome characterized by excessive crying, occurring mostly, in the evenings, without any identifiable cause. The definition of infantile colic given by Wessel et al, based on the characteristic of crying, following the rule of 3, is the most widely used which is; episodes of excessive crying lasting more than 3 hours per day, occurring > 3 days in any week for 3 weeks, in a 2 weeks to 4 months infants, in an otherwise healthy baby [2].
Infantile Colic is a benign self-limited condition that resolves with time, but is one of the commonest reasons of seeking medical advice in the first 3-4 months of life. Duration of the colic may last from a few minutes to three hours or more. The crying begins suddenly without any clear reason and is intense and high pitched. There may be flushing of face, postural changes like clenched fist, tense abdomen and is extremely difficult to comfort the baby during the episodes [3,4].
Due to the difference in diagnostic definition, study design, and family perceptions of “excessive crying”, its prevalence has a wide range of 8% to 40% [2,5,6]. The exact etiology of colic is not very clear. Upto 5% of babies can have an underlying organic causes which may be either in the central nerves system, gastrointestinal tract (constipation, gastro esophageal reflux, lactose intolerance, intussusceptions, rectal fissure) Infections, and Trauma which needs to be considered during the evaluation [7,8]. Babies with infantile colic are normal in growth and development, and have normal examination. Most of the organic causes of excessive crying can be excluded by the history and physical examination and they usually do not need any laboratory tests or imaging studies. There is no long or short term effect of infantile colic on the babies, but it can lead to child abuse [9], increased postpartum depression, and early cessation of breastfeeding [10,11].
Different studies have not reported any major difference in the incidence among term or preterm infants, males or females babies, breast-fed or formula-fed infants [12,13]. But some studies have shown an increased incidence in the first-born children and siblings with previous history of colicky children [14]. Marital relationship status, parental stress, lack of parental self-confidence, dissatisfaction with the delivery has also been found associated with higher incidence of infantile colic [15].
The aim of this study is to assess the incidence, associated factors, and mothers’ knowledge about infantile colic and to identify common managements methods used for colic among healthy full term Omani infants.
This prospective cohort study was performed at Sultan Qaboos University Hospital which is a tertiary teaching hospital in Muscat, Oman. The total number of births in the hospital during 2014 is 4563 babies. During the study duration 1358 babies were born (October, November, and December) (Squh.edu.om, 2015). 1020 was SVD for Omani mothers.
Omani Mothers who gave birth in SQUH during the study period were invited to join the study. It was decided to include only Omani healthy full term infants born by vaginal delivery. The study included deliveries during the period from October to December 2014. Random days during the study duration were selected to invite eligible mothers to participate in the study. Those who accepted to participate were invited to sign a written consent after explaining the purpose and method of the study. Some mothers accepted to participate and filled up the first study questionnaire but they did not complete all study stages either because of the difficulty to trace them (no or wrong telephone number), withdrawal from the study and some were not responding to telephone calls.
Upon agreement to participate in the study, data for every infant was collected from the mother after birth (self-completed questionnaire) as well as their hospital electronic files. The remaining data about the development of infantile colic were collected at the ages of one month, three months and five months via telephone call using a structured questionnaire. During each telephone contact the mothers were asked for information about their infant behavior in the previous duration and the development of infantile colic. Verbal consent was obtained again before each data collection via telephone call. Ethical approval for the study was obtained from the Ethics Committee of College of Medicine and Health Sciences.
The Data was collected using 2 questionnaires; recruitment and follow up questionnaires. The study instrument was developed by the research team based on the literature review. The recruitment questionnaire is composed of 5 sections:
Baby data obtained from the baby electronic medical record (gender, type of delivery, gestational age at birth, birth weight, birth height and head circumference).
Rest of data was obtained via self-completed questionnaire
The answers to the questions provided demographic data, health parameters and address the awareness and attitude of Omani mothers about infantile colic.
The follow up questionnaire is composed of 2 sections:
The questionnaires were piloted on 20 mothers to assess the clarity of questions and to assure that the responses reflect the intended objectives and modifications were done based on mothers feedback.
Database for the study was created in IBM SPSS Statistics 23. Frequency tables and Pie charts have been used to describe the categorized variables as percentages and Chi-square test for association is applied to test the significance of association of infantile colic with demographic and other categorized factors. P-value of .05 or less has been taken as significant.
A total of 64 mothers’ accepted to participate in the study and completed most study stages. The mean age is 29.5 years (SD 5.0, range 20-43 years). Most of the mothers (87.8%) were holder of high education degree, only 13.2% have only up to the high school education. Majority of the mothers (51.6%) were working women, none of the mothers was smoker but six of them (9.4%) reported having chronic health problems (one asthma, two diabetes, and three hepatitis). The total number of offspring’s ranged from 1-9 and total number of family members ranged from 3-19. Majority of the families (68.8%) were nuclear families. Almost all the mothers reported that they have stable families (98.4%) and their economic state is either good or excellent (96.8%) (Table 1).
| Variable | Number (%) |
| Age in years (mean, SD) | 29.5 5.04 |
| Education | |
| High education certificate | 56 (87.5) |
| High school | 07 (10.9) |
| Primary | 01 (1.6) |
| Occupation | |
| Working | 33 (51.6) |
| Not working | 31 (48.4) |
| Total number of children in the family | |
| 1-2 | 26 (40.6) |
| 3-4 | 31 (48.4) |
| ≥ 5 | 07 (10.9) |
| Total number of family members | |
| ≤ 5 | 29 (45.3) |
| ≥ 6 | 35 (54.7) |
| Type of family | |
| Nuclear | 44 (68.8) |
| Extended | 20 (31.3) |
| Economic state | |
| Poor | 02 (3.1) |
| Good | 25 (70.3) |
| Excellent | 17 (26.6) |
Table 1: Mothers and family socio-demographic data.
Among the 64 babies of the study group, proportion of males (59.4%) was more than females (40.6%). Mean gestational age was 39.13 weeks (SD 1.28, range 36-40 weeks) and average birth weight of the baby was 3.00 Kg (SD 0.37, range of 2.2 -3.85 Kg). Mean height of the babies at birth was 51.19 cm (SD 2.26, range of 46.0-56.0 cm) and an average head circumference was 33.09 cm (SD 1.33, range of 28.50-36.0 cm). All babies were born by normal spontaneous vaginal deliveries and among their siblings, ten (15.4%) were the first child of their mothers.
Among 54 mothers, who had previous babies; 29 (53.7%) reported that a previous baby developed infantile colic. The mothers stated that age of starting the crying episodes ranged between 1-20 weeks; (Majority of the mothers reported that crying episodes started during 2-4 weeks (55.2%), followed by week 5-8 (20.7%) and then week 10-20 (17.2%). Very few (6.9%) reported that it started within 2weeks; Most of the mothers (93.1%) stated that the crying episodes occurred in the evening or night. Highest frequency about the number of episodes per day was; ‘3-4 episodes’ reported by 48.3% of the mothers, followed by ‘1-2 episodes’ (37.9%) and then ‘5-7 episodes’ (13.8%). For duration of episode, each episode ranged from 5-60 minutes; (48.3% had the episodes from 5-15 minutes, 41.4% had it for 20-30 minutes and only 10.3% reported it for around 60 minutes). Abdominal colic and pain was reported to be the most frequent reason for the crying (44.8%) followed by abdominal gases and hunger (27.6%) and then abdominal colic and gases (17.2%). Only 10.3% mothers related it to abdominal colic and hunger. Mothers reported that they dealt with the infantile colic using different approaches (Table 2).
| Approach | Number (%) |
| Put the baby on prone position/massage abdomen | 13 (44.9) |
| Giving medicine | 7 (24.1) |
| Continue breast feeding (changing mother diet and drinking herbs) | 6 (20.7) |
| Giving herbal treatment | 2 (6.9) |
| Change to formula milk | 1 (3.4) |
Table 2: Approach to infantile colic in previous child.
As far as the stopped crying episodes at different ages is concerned; only 17.2% reported that babies stopped crying during 4-8 weeks, according to 37.9% mothers end of crying episode noticed during 9-19 weeks, and 41.1% reported weeks 20-36. When the definition of infantile colic criteria were applied to the description of the crying episodes only 4 of the previous babies were classified to suffer from infantile colic (according to frequency and duration of crying episodes). Hence the incidence of infantile colic in the previous babies according to mother report was 53.7% compared to 7.4% according to Wessel definition.
Among the total 31 infantile colic cases, reported by the mothers, majority of the babies (74.2%) developed the colic in the first month and 25.8% developed during the 3 months, and none developed the colic at 5 months of age (Table 3). However, 10.2% of the babies at the age of 5 months are still reported by the mothers to still suffer from infantile colic (Figure 1).

Figure 1: Pie charts of babies having infantile colic at 1, 3 and 5 month.
| Variable | At 1 month Number (%) | At 3 months Number (%) |
| Having infantile colic | 23 (35.9) | 08 (12.5) |
| Having infantile colic using Wessel definition | 3 (4.7) | 01 (1.6) |
| Age developing colic | ||
| 1-2 weeks | 15 (65.2) | - |
| 3-4 weeks | 07 (30.4) | - |
| 5-6 weeks | 01 (4.3) | 02 (12) |
| 7-8 weeks | - | 03 (12) |
| 9-10 weeks | - | 01 (4) |
| 11-12 weeks | - | 02 (8) |
| Timing of colic | ||
| Morning | 03 (13.0) | 03(37.5) |
| Evening | 09 (39.1) | 02 (25) |
| Nights | 11 (47.8) | 03 (37.5) |
| Frequency of colic per day | ||
| 1-2 | 05 (21.7) | 00 (0) |
| 3-4 | 09 (39.1) | 05 (62.5) |
| 5 or more | 09 (39.1) | 03 (37.5) |
| Episode duration in minutes | ||
| 1-<10 | 05 (21.7) | 04 (50) |
| 10-<15 | 13 (56.5) | 03(37.5) |
| 15-<30 | 00 (0) | 00 (0) |
| 30-<45 | 02 (8.7) | 01(28) |
| 45-<90 | 00 (0) | 00 (0) |
| ≥ 90 | 03 (13.0) | 00 (0) |
Table 3: Developing infantile colic at the ages of 1, 3 months in relation to factors associated with colic.
Table 3 illustrates the frequency and characteristics of crying episodes the babies are suffering from as reported by the mothers.
When mothers were asked about the possible causes of the crying episodes and the ways of handling the episodes at the age of 1 month, 30 of the mothers reported that the psychological status of the mothers during the pregnancy could result in infantile colic. Other causes and approaches to the problem at 1, 3 and 5 months are listed in table 4.
| Reason for the colic | At 1 month Number (%) | At 3 months Number (%) |
| Abdominal colic (± gases) | 14 (60.9) | 20 (80) |
| Constipation | 01 (4.4) | 0 |
| Diarrhea | 01 (4.4) | 0 |
| Gases | 06 (26.1) | 05 (20) |
| Hunger | 01 (4.3) | 0 |
| Approach to crying episodes | At 1 month Number (%) | At 3 months Number (%) |
| Continue breast feeding (changing mother diet and drinking herbs) | 6 (26.1) | 12 (48) |
| Change to formula milk | 2 (8.7) | 1(4) |
| Giving herbal treatment | 2 (8.7) | 1(4) |
| Giving medicine | 3 (13.0) | 1(4) |
| Put the baby on prone position/ massage abdomen | 9 (39.1) | 9(36) |
| Total | 23 | 25 |
Table 4: Reasons of the infantile colic and approach to the crying episodes as reported by the mothers.
The breastfeeding problems reported by the mothers include (abdominal pain, crying episodes, abdominal gases, milk is not enough, nipple problem, and refusal of feeding). Majority (82.8%) of the mothers reported that they put the children in prone position to get rid of the gases usually and nine (14.1%) sometimes. The results point to small number of the mothers stopping breast feeding and starting other feeding modalities to treat infantile colic (8.7%). However, table 5 point to decline in breast feeding from 50% at 1 month to 18.4% at 5 months.
| 1 month | 3 months | 5 months | |
| wake up in the night | |||
| 0 | 0 | 9 (14.1) | 1 (2.1) |
| 1-2 times | 17 (26.6) | 25 (39.1) | 31 (63.3) |
| 3-4 times | 32 (50) | 24 (37.5) | 12 (18.8) |
| 5 times or more | 15 (23.4) | 4 (6.3) | 5 (7.8) |
| Awaken by the mother for feed | |||
| Yes | 34 (53.1) | 28 (43.8) | 19 (29.7) |
| No | 30 (46.9) | 35 (54.7) | 30 (61.2) |
| Having defecation problems | |||
| Yes | 15 (23.4) | 12 (18.8%) | 7 (14.3) |
| No | 49 (76.6) | 51 (79.7) | 42 (85.7) |
| Frequency of opening bowel/day | |||
| 1-2 times | 26 (40.6) | 38 (59.4) | 30 (61.2) |
| 3-5 times | 22 (34.4) | 11(17.2) | 13 (26.5) |
| ≥ 6 times | 8 (12.5) | 1 (1.6) | 1 (2.1) |
| Not able to remember | 8 (12.5) | 13 (4.7) | 5 (7.8) |
| Having vomiting | |||
| Yes | 33 (51.6) | 33 (51.6) | 27 (55.1) |
| No | 31 (48.4) | 30 (46.9) | 22 (44.9) |
| Exclusive breast feeding | |||
| Yes | 32 (50) | 22 (34.4) | 9 (18.4) |
| no | 32 (50) | 40 (62.5) | 40 (81.6) |
| Having breast feeding problems | |||
| Yes | 10 (31.3) | 8(36.4) | 2 (22.2) |
| No | 22 (68.8) | 14 (63.6) | 7 (77.8) |
Table 5: Sleep pattern, feeding and bowel habits.
None of the factors was found to be significantly associated with the development of infantile colic (mother reports and applying definition criteria). The baby Gender, weight, order among siblings. Mothers’ age, education, working status, presence of chronic illness, had the experience of another baby complaining of infantile colic previously. The total number of children in the family, number of family members, type of family, economic status. Even the report of baby having defecation problem, frequency of opening the bowel, problem with breast feeding, vomiting, being exclusively breastfed did not show statistically significant association with the development of infantile colic (using mother perception of infantile colic and applying definition criteria).
At the age of one month, 21 (32.8%) of the mothers reported that the babies required a visit to a health facility due to health problems, but only 2 (9.5%) were due to infantile colic. At the age of 3 months, 32 (50%) mothers reported visiting the health services due to health problems and only 6 (18.8%) were related to infantile colic. 49% visited with their babies health facilities at the age of 5 months but none were due to infantile colic. 56.5%, 64% and 40% of the mothers also reported being anxious, worried and nervous about the crying episodes at the ages of one, three and five months respectively. On the other hand mothers also felt that the crying episodes of the baby is a source of fear and distress to her and the family at the ages of one (69.7%), three (44%) and five months (40%). At the age of 1 month 45 (70.3%) of the mothers did not have any information about infantile colic. The source of information for the rest was books (4), internet (4), health services (5), other mothers (4), and past experience (4).
64 Omani mothers who delivered healthy full term babies participated in the study. This study found that the prevalence of infantile colic in a previous baby was 53.75% and 7.4% after using definition criteria. In the follow up of the babies the prevalence was 35.9% at 1 month, 39.7% at 3 months and 10.2% at 5 months. The prevalence of Infantile colic dropped to 4.7% at 1 month, 7.9% at 3 months and 6.1% at 5 months when the definition criteria was used to classify the baby to have infantile colic or not. This indicates that the mothers over report infantile colic and many mothers assume that the babies are having colic when they do not have it. Many studies have pointed out that primiparous mothers tends to experience and report these episodes then others [16].
The results point that the episodes were reported more during the evening and nights which could be a feature of the problem, or simply noted more by the mothers as she might be the only person looking at the baby during these times of the day or having rest and the cry episodes disturb her. Most of the mothers are relating the infantile colic episodes to abdominal colic and presence of gases which is similar to other studies finding [4]. The approach of mothers to the problem was variable but similar to other studies reported approaches, the majority were massaging the baby abdomen and applying positioning maneuver to relieve the abdominal pain [17]. Unfortunately, few mothers changed breastfeeding to bottle feeding as a solution to reduce the crying episodes. The study also found the drop in breast feeding from 50% at the age of 1 month to reach 18.4% at the age of 5 months. This study reported drop in breast feeding similar to other countries report. Internationally and in spite of a ‘baby-friendly’ hospital initiative (BFHI), there is a drop in exclusive breastfeeding for the first few months of a baby’s life as well as further decrease of this rate by the age of six months [18]. This is an alerting finding that requires the attention of the concerned authorities in Oman. All family social and baby factors were evaluated but no statistically significant association were noted. This could be due to real absence of such association or due to the small sample size. Nevertheless, history of having a previous child who experienced infantile colic was positively associated with reporting infantile colic in the current baby but the p value was only 0.053.
Because of the lack of understanding about the pathogenesis and effective treatment of infantile colic, there are still no clear guidelines about the management. A thorough history and physical examination to identify the signs and symptoms is essential to rule out any organic cause and reassurance, self-limiting and the favorable nature of the infantile colic is the first step that should be advised to the parents. The different modalities of treatment of infantile colic are dietary, pharmacological and behavioral interventions including Herbal medicine, Homeopathy, Chiropractic, Acupuncture, and Aromatherapy etc.
Some Pharmacological agents that decrease gastrointestinal gas production might help some infants, but majority of the randomized controlled trials have shown no difference in reducing the overall episodes of infantile colic [4]. Moreover because of the side effects, these medications are not recommended for use in these small babies. Lately, use of probiotics have shown some effective results [19,20] as well as reducing maternal dietary allergen intake and changing the normal formulae to a hydrolyzed formula is an option.
We need to have more definite definition of Infantile colic and more research is necessary for improving our knowledge regarding oral probiotic supplementation, dietary approach and safe and effective pain relieving agents is needed.
Although it is evident that the impact of the problem is big on the affected families as many mothers reported psychological distress related to it. However, at the age of 1 months 45 (70.3%) of the mothers did not have information about infantile colic. And those how had some information the source of information was from health services only in 23.8%. The credential and accuracy of information obtained might not be optimal which necessitate active involvement of public health and pediatrician to provide new mother with required information to deal with this problem.
Limitations: Small sample size and drop out of some participants at 5 months age. Although the study tried to minimize recall biases by calling the mothers at 3 intervals to collect the data, but the possibility of forgetting cannot be completely eliminated which could affect the quality of data collected.
Mothers over labeled infantile colic as the prevalence dropped from 35.9% to 4.7% at 1 month, from 39.7% to 7.9% at 3 months and 10.2% to 6.1% at 5 months when the definition criteria was used to classify the baby to have infantile colic or not. Around two thirds of the mothers reported lack of information about infantile colic. This could explain the over labeling and wrong information about causes and approach to treatment in some of the cases. Those who have information about it their source was not health professionals in large which might through uncertainty on the safety of it. Considering the common labeling of this problem among infants it is important to provide mothers with adequate information about it with clear guidance about handling crying babies. There is also a need to have definite definition of infantile colic and more research to improve the knowledge regarding pathogenesis and the best safe and effective management options.
Download Provisional PDF Here
Article Type: RESEARCH ARTICLE
Citation: Al Saadoon M, Rizvi S, Khan A, Shuaili AKA, Al Mamari MA (2018) Prevalence and Associated Factors of Infantile Colic among Omani Babies. Clin Res Open Access 4(3): dx.doi.org/10.16966/2469-6714.139
Copyright: © 2018 Al Saadoon M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access