Article Information
Article Type: Case Report
Citation: Romero A, Guillo V, Blanco A, Gutierrez A, Garcia J (2016) Electrical impedance tomography for respiratory monitoring during alveolar recruitment maneuver. J Clin Anesth Manag 1(5): doi http://dx.doi.org/10.16966/2470-9956.117
Copyright: © 2016 Romero A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Received date: 29 Apr 2016
Accepted date: 24 Sep 2016
Published date: 29 Sep 2016
Abstract
57 years old patient, with acute myocardial infarction that produces heart failure with an ejection fraction of the left ventricle of 20%, and hemodynamic instability where the implantation of a biventricular assistance was necessary. While entering suffered an impairment of respiratory function. Respirator ventilatory parameters were adjusted to prevent lung damage, low tidal volume (480 ml), respiratory rate of 13 and a level of positive end expiratory pressure of 8 cm H2O. By monitoring pulmonary tidal volume distribution with Electrical Impedance Tomography, bedside, we note that the distribution of tidal volume was not homogeneous. Alveolar recruitment maneuver under the control of the SIT allowed to observe the distribution of tidal volume and which were necessary to ventilate the lungs homogeneusly
Keywords
Image; lung protection; electrical impedance; Bedside
Abbreviations: ARDS
Adult Respiratory Distress Syndrome; EIT: Electrical Impedance Tomography; VT: Tidal volume; PEEP: positive end expiratory pressure; ARM: Alveolar recruitment maneuver; CT: Computer Tomography; Pplat: Plateau Pressure, Cdyn: dynamic compliance; I: E: Inspiratory: Expiratory
Introduction
One problem during hospitalization of patients is the impairment of respiratory function and hemodynamic instability. Before the onset of respiratory problems is difficult to transfer the patient to perform a chest CT because of their hemodynamic status. The lungs undergoing mechanical ventilation may have areas with atelectasis, which favors the distribution of VT is not homogeneous. This lack of homogeneity has been studied by computed tomography, magnetic resonance and isotope methods. However, these methods do not allow monitoring of mechanical ventilation bedside. EIT is used clinically for over ten years. It is free of radiation and has a high resolution, suitable for monitoring the volume distribution in the lung through the electrical impedance during each breathing cycle immediately helping us in selecting ventilator settings.
The more the air contains, lung tissue will be higher electrical resistance. To determine this impedance is incorporated around the patient’s chest a belt with 16 electrodes that are distributed around the chest diameter. A pair of electrodes applied a very low current, and the other electrodes measure the respective resulting tensions that change the content of air in the chest. The application of current rotates around the chest, and thus also changing the measurement points of stress.
Case Presentation
Male patient, 57 years old, 80 kg of weight and 173 cm tall, with a history of diabetes mellitus and hypertension who suffers an acute myocardial infarction involving severe heart shape, left with impaired myocardial function with a fraction 20% ejection. This necessitated the implantation of a biventricular cardiac assistance. During the stay in the critical care unit the patient suffered a deterioration of respiratory function with impaired gas exchange. Respirator ventilatory parameters were adjusted to avoid lung distension in the mode BIPAP with maximum pressure of 21 cm H2O and PEEP of 8, with resultant tidal volume of 480 ml, respiratory rate of 13 and an I / E 1 / 2. O2 saturation was 93% and pO2 was 73 mm Hg with FiO 2 50%, with pCO2 of 33 mmHg. The dynamic compliance was 38 ml / hPa. By monitoring pulmonary tidal volume distribution Electrical Impedance Tomography (EIT) (PulmoVista 500, Dräger), bedside, we note that most of the VT is not evenly distributed in the lungs. Most of the volume, 42% +29% (71%) for the right lung field and was distributed only 17% + 4% (21%) directed to the left lung. (Figure 1)
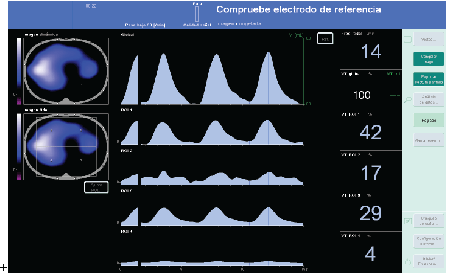
Figure 1: Image reference prior to Alveolar recruitment maneuver (ARM). To the left side of the image is observed the lung segment divided into four quadrants; 1 and 3 for the right lung field and 2 and 4 to left field. In blue color is represented normally ventilated area and in white possible alveolar distension.
In the right column, the percentage of tidal volume distributed in each quadrant is observed and found that the left lung only reaches 21% (17% + 4%).
Alveolar recruitment maneuver (ARM) under monitoring with EIT allowed to observe the distribution of tidal volume and what was the alveolar opening pressure needed to maintain the lung open. So far no evidence has been found which is the best alveolar recruitment maneuver. AMR was used in the patient described in ART study, which maintains a continuous pressure gradient which appears to be a variable protective of lung damage in patients with respiratory distress syndrome, although there is no evidence to the time [1]. The technique was used as AMR was to gradually increase the PEEP of 5 in 5 cm H2O, and the maximum pressure in parallel, maintaining a constant pressure gradient of 15 cm H2O. Each pressure rise during the we held for 10 respiratory cycles, with I: E ratio of 1: 2. Once recruited, we reduced pressures more progressively, 2 by 2 cm H2O in pressure controlled mode, to see that we observed maximum compliance PEEP. Then we repeated the AMR and we established a PEEP 2 cm H2O above PEEP from which the compliance began to worsen in the previous ARM. The recruitment maneuver was carried out in about 3 minutes.
During the AMR observed improvement in the distribution of VT up to a maximum of 25 cm H2O PEEP and plateau pressure of 40 cm H2O. EIT note with the VT distribution was more homogeneous, deriving 52% to the right lung and 37% to the left lung. We kept the I: E ratio of 1: 2 for the AMR, reaching VT of 550 ml and O2 Sat 99%. The maximum compliance achieved was 37 ml / hPa to decrease PEEP cm H2O below 8 during the expiratory phase of the AMR and this correlated with the image of the EIT in which percentage of ventilated left lung field is lost. We established as optimal PEEP 10 cm H2O, 2 cm H2O over the PEEP under which we look at the collapse with the EIT and the fall of the Cdyn. After the AMR, remained 10 cm H2O PEEP, blood gases, with FiO2 of 0.5%, I: E ratio of 1: 2, was 113 pO2 , pCO2 32. Cdyn was 60, with 25 cm H2O of maximum pressure, obtaining a VT of 530 ml and 99% Sat O2 . VT distribution at this time was more homogeneous, with improved ventilation of the left lung which went from 21% to 37% of the VT. (Figure 2,3)
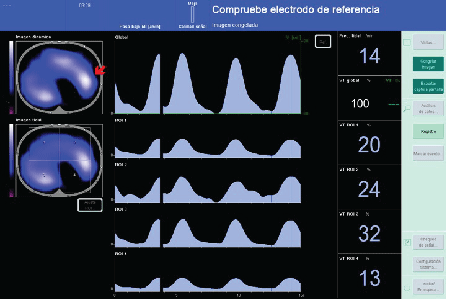
Figure 2: VT distribution after AMR was 52% in the right lung and 37% on the left, thereby improving 16% distribution VT in the left lung from the previous time the AMR. The red arrow indicates the area where VT percentage has been won.
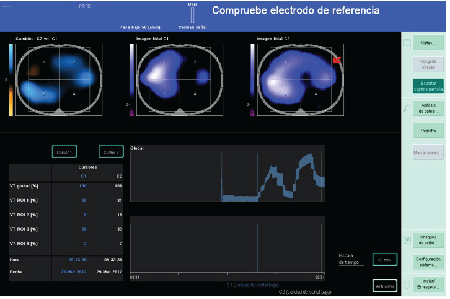
Figure 3: Comparison shows images before and after the AMR. In upper right graph (red arrow) shows that a larger percentage of lung ventilated once the AMR, to the central upper graph. (Image before the AMR)
Discussion
Mechanical ventilation can cause damage or increase the lung damage may already exist and that concept has been called lung injury induced by mechanical ventilation (VILI) [2,3].
The VILI relates to the application of a PEEP level insufficient to prevent alveolar collapse and reopening cyclic (atelectrauma) causing increased alveolar inflammatory infiltrate [4], the use high alveolar pressures (barotrauma) and causing perivascular and alveolar edema [5]; and high respiratory rates, repetitive cycling [6]. Also the high tidal volume (volutrauma) seems able to induce cyclical alveolar distension[7].
Preventing alveolar over distension can be achieved using VT ≤ 6 ml/ kg ideal weight and Pplat<30 cm H2O [8].
EIT is a technique that does not identify any such damages by inadequate mechanical ventilation. But it, lets see directly the effectiveness of the ARM, and therefore helps to establish what necessary for effective ARM and helps set the proper PEEP level, allowing a more homogeneous distribution of tidal volume pressures.
EIT has proven to be a technique that can monitor changes in lung volume during mechanical ventilation bedside [9].
In this case it identified the VT not distributed evenly throughout the lung fields, before making the ARM, and allowed to observe directly gain lung volume ventilated during ARM guiding the pressures of pulmonary open until they arrive during ARM.
EIT bedside could be an alternative to CT scans in evaluating the ventilation of lung regions [10].
Acknowledgements
Thanks to the doctors Maria Victoria Martinez, Jose Manuel Alvarez Avello y Pelayo de Merlo, for their assistance in this case report.
Conflict of Interest
The signatories authors qualify for authorship: Antonio RomeroBerrocal, Verónica Guilló, Angel Blanco, Alberto Gutierrez, Javier García. Each of the authors declare the absence of financial interest or conflict of interest.
Download Provisional pdf here




