
Full Text
Boudewijn Catry* Karl Mertens Katrien Latour Barbara Legiest Els Duysburgh Theofilos Papadopoulos Eline Vandael Thomas Struyf Laure Mortgat Naima Benhammadi Helene De Pauw Herman Van Oyen
Healthcare associated Infections & Antimicrobial Resistance, Public Health and Surveillance, Sciensano, Brussels, Belgium*Corresponding author: Boudewijn Catry, Healthcare associated Infections & Antimicrobial Resistance, Public Health & Surveillance, Sciensano, Brussels, Belgium, Tel: +32 (0) 2 642 57 64; Fax: +32 (0) 2 642 54 10; E-mail: Boudewijn.Catry@sciensano.be
This activity report provides an overview of the most recent evolutions in healthcare associated infections and antimicrobial resistance in Belgium. The positive downward trend we have been observing for many years in the incidence of Methicillin Resistant Staphylococcus aureus (MRSA) in acute care hospitals appears to be stabilizing in 2016. The hand hygiene campaigns held biannually since 2005, which reduce -among many other initiatives- the spread of these bacteria through direct contact, contribute to this evolution. Also in intensive care units hand hygiene compliance increased significantly and the incidence of pneumonia following intubation has reduced remarkably.
Other resistant bacteria, mainly present as a reservoir in the digestive tract (gut), are however on the rise and can cause severe bloodstream infections. In particular, Carbapenemase-Producing Enterobacteriaceae (CPE) and Vancomycin-Resistant Enterococci (VRE) are increasingly being isolated and have caused outbreaks in several hospitals. The number of Clostridium difficile infections (severe enteritis and colitis) also slightly increased since 2014, although its associated mortality decreased. In long-term care facilities (among others nursing homes), similar evolutions are taking place (decrease in MRSA, increase in multi-resistant gut bacteria). Long term monitoring shows a recent slight decrease in antimicrobial consumption in the ambulant sector but alas not in the hospitals. Antimicrobial use should urgently be further optimized in our healthcare facilities in order to control the selection pressure for antimicrobial resistance.
Since 2014 and in collaboration with the inspection services of the competent authorities, assistance is being offered to hospitals and long-term care facilities that suffer from difficult to treat bacteria in the form of an outbreak support team (MDRO – OST; Multi-Drug Resistant Organisms - Outbreak Support Team). In the period 2014-2016, 13 out of 15 reported outbreaks where assistance was granted, containment was achieved within a reasonable time frame.
Healthcare associated infections; Antimicrobial consumption; Hand hygiene; ICU; Blood stream infection; Clostridium difficile; CPE; VRE; MRSA; ESBL
A healthcare associated infection, shortly care infection, is an adverse event not present at admission in a hospital or long term care facility (LTCF) and a large proportion can be prevented by appropriate infection prevention measures. In Belgium, the National Surveillance of Infections in Healthcare settings (NSIH) monitors risk factors and outcomes of healthcare associated infections. In charge is the service “healthcare associated infections and antibiotic resistance” of Sciensano, previously the scientific institute of public health (WIV-ISP). Antibiotic use is monitored as it remains the most important factor to influence resistance. Our service also assists in the biennial national hand hygiene campaigns that measure the compliance of hand hygiene. We also collect specific quality indicators related to infection prevention and control. Since 2014, the service formally provides assistance, in cooperation with the inspection services of the competent authorities, in the form of outbreak support [1] for hospitals that suffer from difficult to treat microorganisms (multidrug resistant organisms, MDRO, see table 1).
| Accronym | Microorganism | Antibiotic resistance | Habitat |
| MRSA | Staphylococcus aureus | Met(h)icillin | skin, upper respiratory tract |
| ESBL+ | E. coli, Klebsiella, Enterobacter | 3de generation cephalosporins | digestive tract |
| CPE | E. coli, Klebsiella, Enterobacter | Carbapenems | digestive tract |
| VRE | Enterococcus faecalis/faecium | Vancomycin | digestive tract |
| PSAR/ABC | Pseudomonas/Acinetobacter | Different classes | ubiquitous, skin |
| CDIF | Clostridiumdifficile | Intrinsic or natural resistant | digestive tract |
Table 1: List of major multidrug resistant organisms (MDRO) surveyed in Belgian acute hospitals and other healthcare settings, 2016.
Monitoring of healthcare associated infection focuses on different types of hospitals and chronic care institutions, required by federal and regional laws (see box) and / or within the framework of European projects. On the one hand, our service at Sciensano makes standard definitions and automated feedback systems available for care institutions. Secondly, national reference data are collected on the occurrence of healthcare infections and antibiotic resistance in Belgium. The Belgian Antibiotic Policy Coordination Committee (BAPCOC), established in 1999, is supervising these protocols and awareness campaigns in related areas.
The purpose of this review is to provide an overview of the most recent evolutions in occurrence of healthcare associated infections, antimicrobial resistance, antimicrobial consumption, sustaining hand hygiene campaigns, outbreak support results and related projects in Belgium.
Surveillance of bloodstream infections
Bloodstream infections (BSI) are very serious with often a fatal outcome. The surveillance of hospital acquired (synonym nosocomial, by definition >2 days after hospitalization) BSI exists in Belgium on a voluntary basis since 1992. Since 2014, participation became mandatory. The nationwide incidence for 2016 (7.8/10,000 patient days) is comparable with recent years [2]. As in previous years, in 2016 we found a large variability between hospitals. This suggests possibilities for prevention and a further need for data validation. BSIs are most commonly reported in tertiary hospitals (university character). The departments that are most frequently affected are the intensive care units (an approximately four times higher incidence in the intensive care unit in 2016 than the incidence for the entire hospital).
The most common origin of BSI acquired in the hospital was a central line (Central Venous Catheter; CVC), although these have been reported less since 2013 until 2016 [2]. Of all hospital-associated bloodstream infections, 40% was directly (CVC) or indirectly (urinary probe or endotracheal tube) associated with an invasive device in 2016. Compared to 2013, the hospital wide central line associated BSI incidence decreased in 2016. These infections associated with an invasive device are a priority for interventions [2]. Escherichia (E.) coli (23%) and Staphylococcus (S.) aureus (11%) were the most common microorganisms isolated from hospital-associated BSI in 2016. The incidence of hospital-associated BSI with E. coli and Klebsiella (K.) pneumoniae has increased continuously since 2000.
From 1 July 2017, the input of surveillance data for BSI will take place via a new ICT platform called Health data [3].
Intensive care units & surgical site infections
Since 1997, Sciensano has been organizing the national surveillance “Infections acquired on intensive care units (ICU, intensive care units)” and since 2000 the national surveillance “Post-operative wound infections (SSI, surgical site infections)”. Since 2003, the ICU and SSI surveillance use European definitions and data collection methods. These have been issued since 2008 by ECDC (European Centre for Disease Prevention and Control, Stockholm, SE). Due to the sporadic participation in the SSI surveillance during the last few years (annually <5), no national report was published in 2015. In 2017, both surveillance protocols and software (NSIH win) of the ICU and SSI surveillances were updated [4-6].
Results of the ICU surveillance are available up to and including 2015 [7]. In 2015, the average length of stay of the follow-up patients was 7.9 days for ICUs. The average use of respiration (via invasive intubation) and central lines (central vascular catheter, CVC) was 443 intubation days and 738 catheter days per 1000 ICU days, respectively. On average, 4.2% of the follow-up patients in 2015 acquired pneumonia (pneumonia) on ICU. The incidence of ICU-acquired pneumonia was 6.7 episodes per 1000 days of hospitalization, whereas that of intubation-associated pneumonia (IAP) was 8.5 episodes per 1,000 intubation days. In particular, the latter indicator is undergoing a declining historical trend, with the incidence of IAP in 2015 being only 30% of that of 1997 (Figure 1). The incidence of ICU-acquired BSI in 2015 was 2.2 episodes per 1000 patient days and for CVC-associated BSI the incidence was 2.1 episodes per 1000 CVC days. The incidence of BSI with “catheter” or “unknown” as documented origin was 1.3 episodes per 1000 patient days. Whereas the surveillance of BSI shows a downward trend in incidence, this decrease is not confirmed so far in the surveillance tailored for the intensive care department. Note that in addition to the classical microorganisms, Candida species (C. albicans and C. glabrata) have been reported almost continuously in the top 10 of most common organisms in recent years [7].
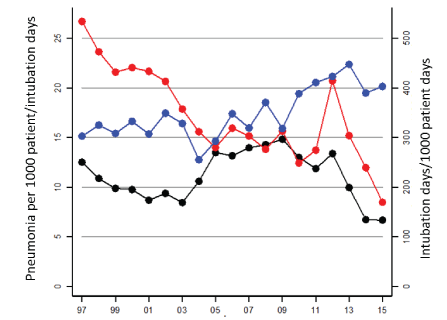
Figure 1: Evolution of Intensive Care (ICU) acquired (black line) and intubation-associated (red line) pneumonias, and intubation use (blue line) on intensive care units, Belgian surveillance, 1997-2015.
Surveillance of acquired antibiotic resistance
For 2016, the overall average methicillin resistance prevalence among all reported S. aureus isolates was 15.9% in hospitals. The mean incidence of nosocomial (not present at admission) Methicillin Resistant S. aureus (MRSA) was 0.9 cases/1000 admissions (0- 5.2/1,000) or 0.14 cases/1000 hospital days (0-0.57/1000). The trend of these resistant bacteria, favorable evolving since 2004, is presented in figure 2a. An opposite evolution is observed regarding the incidence and multi-resistance in Gram-negative microorganisms, with natural habitat in the gut (Table 1, Figure 2b). In 2016, the mean proportion of ESBL (extended spectrum beta-lactamase) production was 12.3%, 7.7% and 18.6% for Enterobacter cloacae (including screening samples), E. coli and K. pneumoniae, respectively. The mean incidence per 1000 admissions of ESBL-producing Enterobacteriaceae in 2016 was 1.06 for Enterobacter cloacae, 5.86 for E. coli, and 3.36 for K. pneumoniae. An increase in Carbapenemase-Producing Enterobacteriaceae (CPE) has also been observed since 2012 until 2016. The mean proportion of carbapenemase positive E. cloacae, E. coli, and K. pneumoniae in 2016 was respectively 1.4%, 0.1%, and 1.1%. Trends of antibiotic resistance in these organisms are similar to those observed in other EU countries [8]. Although an increasing trend in vancomycin resistant enterococci (VRE) is suspected, the optional surveillance is too young to be able to indicate a significant trend. Enterococcus (E.) faecalis was by far the most frequently reported species in 2016 (65.1% of all isolated enterococci in 95 hospitals), three times more frequent than E. faecium (19.5%). Resistance, however, was more frequent in the latter microorganism, with 1.5% resistant to glycopeptide (vancomycin + teicoplanin) compared with 0.03% in E. faecalis.
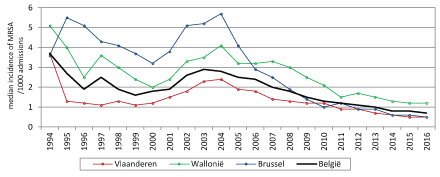
Figure 2A: Declining incidence of bacterial infections with methicillin resistant Staphylococcus aureus (MRSA) (for hospitals with at least 5 participations).
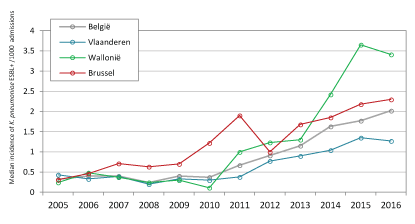
Figure 2B: Increasing incidence of extended spectrum betalactamase producing (ESBL +) K. pneumoniae (hospitals with at least 3 participations) per 1000 admissions for 1994-2016 in Belgium (national trend; dashed grey line) and stratified by regions (colored lines).
Surveillance of acquired antibiotic resistance in invasive pathogens
The European Antimicrobial Resistance Surveillance Network (EARS-Net) monitors the evolution of acquired antimicrobial resistance at European level [9]. This is done voluntarily on the basis of results that are communicated to Sciensano as standardized and automatically as possible by clinical laboratories [10]. To keep the European numbers as comparable as possible, the results are limited to those of invasive isolates (blood and cerebrospinal fluid) of eight pathogenic bacteria species: S. aureus, Streptococcus pneumoniae, E. faecium, E. faecalis, E. coli, K. pneumoniae, Pseudomonas aeruginosa and Acinetobacter species.
In 2016, 31 of 102 Belgian clinical laboratories provided data. The declining trend for non-sensitivity to meticillinin S. aureus (MRSA) between 2012 and 2015 stabilized at around 12.2% in 2016. The increasing trend of fluoroquinolone resistance of E. coli between 2012 and 2015 did not continue in 2016. Other findings, however, emphasize the need for further vigilance. Klebsiella pneumoniae is losing more and more sensitivity to cephalosporins of the 3rd generation and also to carbapenems, resulting in average resistance rates of 22.9% and 2.4% respectively. After a decline in gentamicin resistance in E. faecalis to 12.5% in 2015, we were able to see a strong increase in 2016 (19.8%). Resistance levels of P. aeruginosa versus ceftazidime, carbapenem, aminoglycosides, amikacin and fluoroquinolones all increased in 2016 compared to 2015. For more details and a detailed discussion of the results, we refer to the Belgian EARS-Net annual report [9].
Surveillance intrinsic antibiotic resistance – Clostridium difficile infections
Clostridium difficile (CDIF) infection is a major cause of diarrhea and pseudomembranous colitis, acquired often in the hospital and chronic care institutions, with an estimated 4,000 episodes in Belgian healthcare settings per year. Antibiotics, usually given for another bacterial infection, are by far the most important risk factor for contracting this infection because C. difficile is naturally (intrinsic) resistant to various antibiotics.
The C. difficile incidence in Belgian acute hospitals in 2016 was the highest incidence (1.99/1,000 admissions) reported since 2009. Approximately 60% is attributed as being ‘acquired in the hospital’ (Figure 3). Regional differences, still negligible in 2015, were found to be more pronounced in 2016. The highest numbers are found in Wallonia and the lowest in Flanders. Mortality has been constantly decreasing nationally since 2006. Note, however, that the mortality numbers are only available up to and including 2014.
Ribotyping is done on a selection of strains sent to the National reference centre (UCL, Mont Godinne, Michel Delmée). The hypervirulent strains BRO27 and BRO78 continue to circulate nationwide in hospitals and are reported in 26% and 38% of hospitals, respectively. Despite new diagnostics and the emergence new treatments like faecal transplantation [11], the cautious use of antibiotics remains the most meaningful and necessary way to keep C. difficile in Belgium under control.
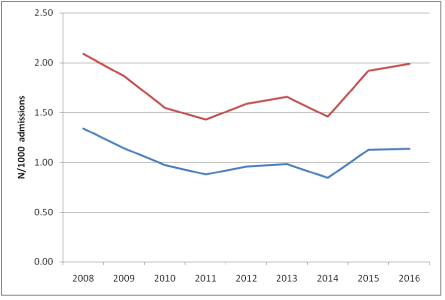
Figure 3: IAverage incidence (N/1000 admissions) of C. difficile infections (CDI) in Belgian hospitals, Belgium, 2008-2016. Only acute care hospitals (mean length of stay <14 days) providing data for the whole year were included in the incidence calculation. From these, the total number of CDI (red line) and healthcare associated CDI, i.e. symptoms present ≥2 days after admission (blue line), are shown.
Antibiotics, together with antimycotics (fungicides and yeastfighting agents) and tuberculostatica (anti-tuberculosis) belong to the group of antimicrobial medicines. Sciensano, in close cooperation with the RIZIV-INAMI (Belgian National Institute for Disability and Disability Insurance –Service Research, Development & Quality and Pharmanet), monitors the use of ambulatory practice (general practitioners) and intramural use (hospitals en large chronic healthcare settings). The emphasis on analysis of this consumption is currently on the antibiotic selection pressure at large, given that this is the most urgent resistance issue in Belgium and neighboring countries [12].
Selection pressure in ambulatory practice – (general practitioners, GPs)
ESAC-Net is the European network of national surveillance systems of antimicrobial consumption [13]. In Belgium, the RIZIV-INAMI consumption data were extrapolated for this to 100% for the entire Belgian population [14]. Use is expressed in the number of prescribed daily doses per 1000 inhabitants (DID). The ESAC-Net numbers for Belgium show that in 2016 the use of antibiotics for systemic use (J01) in the ambulatory sector declined compared to previous years (27.51 DID, 6.1% decrease compared to 2015). The trend of antibiotic use over the years, with a subdivision of the antibiotics subclasses, is shown in figure 4. The largest decrease in consumption was seen in the group of penicillins (J01C), specifically determined for penicillins in combination with a beta-lactamase inhibitor (J01CR, decline in 2016 of 14.5% compared to 2015). In addition, in 2016 there was also a decrease in the consumption of other antibiotics classes compared to the previous year, mainly for second generation cephalosporins (J01DC, -8.1%), fluoroquinolones (J01MA, -7.6%) and macrolides (J01FA, -2.1%). Nevertheless, the use of azithromycin (+ 4.7%) does continue to rise.
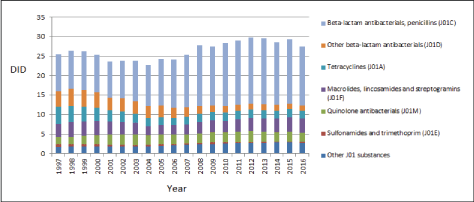
Figure 4: Trend of antibiotics use for systemic use (J01) in the ambulatory sector in Belgium between 1997 and 2016, expressed as incidence in prescribed defined daily doses (DDD) per 1000 inhabitants and per day (DID).
Selection pressure intramural – hospitals
The use of antibiotics for systemic use (J01 [15]) in acute Belgian hospitals (N=102) in 2016 is comparable with previous years with a median of 577.1 DDDs per 1000 days of hospitalization. The antibiotic use was higher in the tertiary hospitals (N=7, median: 715.0 DDDs per 1000 hospital days) in comparison with the other hospitals. The most commonly used antibiotics classes were ‘penicillins in combination with a beta-lactamase inhibitor’ (J01CR, 34.3% of the total number of DDDs in J01), followed by the ‘fluoroquinolones’ (J01MA, 11.0%). The top 3 antibiotics with the highest consumption consisted of amoxicillin in combination with clavulanic acid (J01CR02), ciprofloxacin (J01MA02) and cefazolin (J01DB04) (Figure 5).
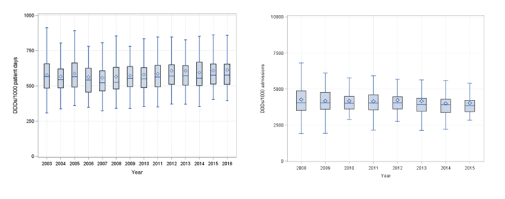
Figure 5: Evolution of antibiotic use for systemic use (J01) in acute Belgian hospitals (N = 102) between 2003 and 2016 expressed in daily defined doses (DDDs) per 1000 days (A. left), and between 2008 and 2015 expressed in DDDs per 1000 admissions (B. right). *Legend box plot: a. Maximum (without outliers, 1.5 × interquartile range), b. 75 percentile, c. Median, d. Average, e. 25 percentile, f. Minimum (without outliers, 1.5 × interquartile range).
Based on the current numbers for 2016, we can cautiously speak of a decrease in antibiotic use in the ambulatory sector. This, as well as the decrease for specific groups such as the fluoroquinolones, is in line with specific objectives of the national strategic plan to combat antimicrobial resistance [16]. Despite this decline, this consumption remains high compared to other European countries [17]. In hospitals, the use of antibiotics remains stable over time. Therefore, further use should be made of the responsible use of antimicrobial agents. A surveillance based on diagnoses (e.g. APR-DRGs: All Patient Refined Diagnosis Related Group) can help provide more focused feedback for prescribers.
Both national (BAPCOC-funded) and international (ECDCfunded) point prevalence studies on antimicrobial resistance and healthcare associated infections, respectively, are repeatedly done in Belgian long term care facilities, predominantly nursing homes, due to the specific risk factors and intervention strategies related to the residents. (Point prevalence surveys in acute care hospitals also are performed in Belgium, but will be reviewed in a European context elsewhere).
In 2015, a third national prevalence study on resistance to bacteria was carried out among 1,441 residents in 29 Belgian long term care facilities (LTCF). In 2015, 9.0% of the residents were diagnosed with MRSA carriers, 3.2% less than in the previous national prevalence study (2011). However, this study showed a clear increase in the number of residents, carriers of ESBL-producing Enterobacteriaceae (11.8% in 2015 versus 6.2% in 2011). E. coli was the most frequently isolated ESBL + species (82.7%), followed by K. pneumoniae (14.9%). Furthermore, 2.4% of the residents carried both ESBL + E. coli and ESBL + K. pneumoniae. The relative proportion of K. pneumoniae increased significantly in 2015 (17%) compared with 2011 (5%, p <0.001, linear regression in STATA). Only one resident was a carrier of a CPE and one resident of a VRE. The prevalence of these germs in LTCF residents was therefore very low (<0.1%).
In 2016-2017, a third European prevalence study was conducted on healthcare associated infections and antibiotic use in residential care centers (HALT-3, point prevalence survey on Healthcare associated infections and Antimicrobial use in Long-Term Care Facilities). The organization of the study in the participating European countries was outsourced to Sciensano by ECDC. Between September and November 2016, 165 institutions were recruited in Belgium on a voluntary basis: 158 nursing homes, three psychiatric institutions and four rehabilitation centers. Of the sample residents 4.5% suffered from a healthcare associated infection on the day of the study (minmax: 0.0-17.5%). The most common infections were respiratory tract infections (40.9%), urinary tract infections (29.5%), as well as skin and wound infections (17.2%). Of these, 77.3% of the care infections were linked to their own chronic care institution. The number of residents with at least one systemic antimicrobial treatment was 5.5% (min-max: 0.0-18.3%). The majority of the prescriptions were systemic antibiotics (code ATC J01, 94.4%) and 97.5% were products administered orally. These antimicrobials were prescribed in 82.5% of cases in the health care institution where the resident was staying. Of the prescriptions, 63.7% were curative (therapeutic) prescriptions. Of the preventive (prophylactic, 35.8%) prescriptions, 78.3% was for the protection of the urinary tract.
Thus, vigilance is needed in this type of care institutions and it is certainly useful to regularly repeat such prevalence studies [18].
Campaigns to promote hand hygiene
Every two years a nationwide monitoring of the compliance of the international guidelines on hand hygiene (HH) is organized. Compliance with the HH guidelines increased significantly from 69.1% in 2015 to 77.7% after the awareness period (national weighted average P <0.0001). The percentage of compliance increased for all types of healthcare professionals (around 6% to 12%), with the best results for nurses. Compared with previous campaign results, compliance with guidelines is still significantly higher for ‘after patient contact’ and ‘after exposure to body fluids’ compared to ‘before patient contact’. The possibility of automation systems (e.g. hand scans upon entry of a ward or room) of hand hygiene in particular for the indication ‘for patient contact’ should receive consideration for research projects.
With regard to the different specialties, there was a general increase in the compliance with hand hygiene with the best results on the services pediatrics/neonatology and ICU. Figure 6 shows the increase in compliance with hand hygiene on the ICU services. Note that in 2012 a new software application (NSIHweb2.0) was launched with an increase in both the number of observations (approximately quadrupled) and a significant improvement in hand hygiene [19].
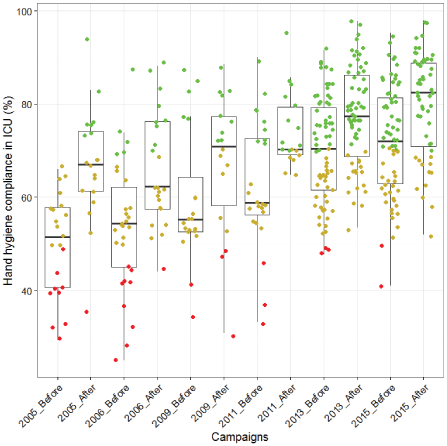
Figure 6: Evolution of hand hygiene compliance in Belgian intensive care units (ICU) from 2005 to 2015, measured during the biennial national campaigns prior to before and after an awareness period. Results were reported by participating hospital as a weighted mean adjusted for varying number of observed opportunities between hospitals. The median (represented by a horizontal line in each box), the interquartiles (height of the box), the maximum and minimum limits (vertical lines) of the compliance are indicated, as well outliers. Individual data points are not exact, but moved to better visualize the distribution across all hospitals with an arbitrary compliance level accessed via color code over consecutive campaigns; green: good; brown: moderate; red: low. Reproduced from reference [18] distributed under the terms of the Creative Commons.
Outbreak support team (OST)
The Outbreak Support Team for multidrug resistant organisms (MDRO-OST) was established in 2014 to support healthcare institutions in their management of an MDRO outbreak and strives for appropriate help. This assistance encompasses various levels: scientific advice, guidance on prioritization of measures, mediating role between different actors, intervention on the ground aimed at constructive dialogue, assessment of the workplace and sampling, and (exceptional) enforcement through formal writing of competent inspection services. The results of the NSIH-surveillances on antibiotic resistance and use are bundled and consulted and discussed with the hospital hygiene team and the care departments involved. The MDRO-OST consists of the health inspections or services infectious disease control of the federated entities, experts of Sciensano (NSIH) and is supported by the relevant national reference centers (NRC) and external experts.
The hospital or residential care institution itself decides to call in the assistance of the OST. This question is possible after the report of the outbreak to the communities/regions (Table 2). The number of here reported outbreaks and the subsequent visits are an objective observation. This does not reflect the complexity of each specific situation nor the efforts made, but these declarations allow an estimate of the national evolution of outbreaks in time and place in Belgium (etiology, severity and size). In the period 2014-2016, 13 out of 15 outbreaks of bacteria that were difficult to treat were timely brought under control by good cooperation between the Sciensano, the competent authorities and the hospital staff involved (Table 2).
| Request made | Region | MDRO | Resistance mechanism (virulence) | Bacterium involved (Genus species or family) |
| 12/18/2014 | Flanders | VRE | VanA | Enterococcus faecium |
| 1/9/2015 | Flanders | CA-MRSA, | (PVL+) | Staphylococcus aureus |
| 1/29/2015 | Flanders | CPE | VIM | Enterobacteriaceae |
| 3/23/2015 | Flanders | VRE | VanA | Enterococcus faecium |
| 5/21/2015 | Flanders | CPE | oxa-48 | Klebsiella pneumoniae |
| 6/10/2015 | Wallonia | CPE | oxa-48 | Klebsiella pneumoniae |
| 9/24/2015 | Brussels | PSAR | Pseudomonas aeruginosa | |
| 1/18/2016 | Flanders | CA-MRSA | (PVL+) | Staphylococcus aureus |
| 2/19/2016 | Wallonia | CPE | NDM | Enterobacteriaceae |
| 2/19/2016 | Wallonia | VRE | VanA | Enterococcus faecium |
| 4/25/2016 | Flanders | CA-MRSA | Staphylococcus aureus | |
| 5/23/2016 | Wallonia | CPE | oxa-48 + NDM | Klebsiella pneumoniae |
| 7/5/2016 | Wallonia | VRE | VanA | Enterococcus faecium |
| 7/1/2016 | Flanders | VRE | VanA | Enterococcus faecium |
| 12/7/2016 | Wallonia | CPE | Klebsiella pneumonia | |
| 1/18/2017 | Flanders | VRE | VanB | Enterococcus faecium |
| 1/30/2017 | Wallonia | CPE | oxa-48 | Enterobacteriaceae |
| 3/21/2017 | Flanders | CPE | Enterobacteriaceae | |
| 3/29/2017 | Flanders | VRE | VanB | Enterococcus faecium |
| 4/21/2017 | Wallonia | PSAR | Pseudomonas aeruginosa | |
| 8/2/2017 | Flanders | VRE | VanA | Enterococcus faecium |
| 9/1/2017 | Flanders | CPE | Klebsiella oxytoca |
Table 2: Overview of outbreaks of multidrug resistant organisms (MDRO) where the multidisciplinary outbreak support team (OST) was engaged, Belgium December 2014-2017.
*VRE: Vancomycineresistente Enterococcus; CA-MRSA: Community Associated Methicilline Resistente Staphyloccocus aureus; PVL: Panton-Valentine Leukocidine; CPE: Carbapenemase Producer End Enterobacteriaceae; VIM: Verona Integron-encoded Beta-Lactamase; oxa-48: Oxacillinase-48; NDM: New Delhi MetalloBetaLactamase; PSAR: Pseudomonas aeruginosa.
Quality indicators for hospitals
To stimulate accountability by the hospitals, quality indicators related to infection prevention and control (and scores per hospital) are available to the public since 2013 [20]. A second data collection round took place in 2016 (data 2015) and showed a clear improvement of some weak points compared with the previous data collection round (data 2013), e.g. the integration of a strategic infection control plan into the hospital’s strategic plan (39% versus 70%, respectively). Surveillance of SSI remains a point of improvement for a large number of hospitals. The disclosure of such process indicators proved to be a powerful tool for accountability. However, there was no external control of the data and the number of indicators was limited. The protocol will therefore be reviewed by the competent federal hospital hygiene platform of BAPCOC. Sciensano also aims for further harmonization with regional initiatives on transparency within the healthcare sector such as the VIP2 project (www.zorgkwaliteit.be) and PAQS (www.paqs.be).
Sciensano monitors various aspects of healthcare infections, which testify to previous research priorities in a historical context and later evolutions at regional and international level. Our services and research activities are no longer limited to specific healthcare infections or the environment of hospitals, but cover the widest possible range of sub-aspects, including residential care centers. The continuous changing software options offered by data providers and analysts also influence our operations. The immediate feedback of compliance with hand hygiene has greatly increased the number of observations and compliance, but new technologies need to be investigated for further and necessary improvement.
Favorable evolutions were noted for MRSA in all our surveillances and for all types of healthcare institutions. This germ is found on the skin (and in the nose) of carriers, and detection, contact isolation and decolonization with local treatments is possible. The hand hygiene campaigns also played a positive role here. After all, the compliance of hand hygiene has evolved very favorably in recent years and in particular in the ICU since 2013, where a sharp decrease in the number of respiratory healthcare infections has been reported simultaneously.
An unfavorable evolution is seen for healthcare infections that arise from the intestinal tract and this also in the various surveillance and types of care institutions. The intestinal tract is transformed into a multi-resistance reservoir under the influence of a large antibiotic selection pressure. Originally sensitive germs become resistant and originally less sensitive or resistant bacteria are favored. This is clearly reflected in the emergence of multiresistant Gram-negative (ESBL, CPE) and Gram-positive (C. difficile and VRE) bacteria. Such trends are also noticeable in other countries [21,22], and the alertness for the problem is therefore increased.
These two opposite evolutions are also seen in chronic care institutions, and the prevalence of ESBL carriers in 2015 in these settings was even higher than that of MRSA carriers. Fortunately, the absolute numbers of the difficult to treat intestinal bacteria CPE and VRE remain very limited. Another selection pressure (other antibiotics classes) in LTCF probably lies at the basis here. In the medium term, however, the exchange between different types of care institutions is unavoidable given the percentage of incontinent people in this age group combined with the fact that these germs are stored in the digestive system, unreachable for decontamination and disinfection by hand hygiene. Additional measures on gesture of excreta and environment cleaning are required [23].
Further integration of our surveys within Health data (data collection) and Health stat (feedback) is in full preparation and this in collaboration with competent working groups (technical unit (TC) MDRO and BAPCOC). In this respect, consideration is given to organizing a quicker feedback and also enabling new threats (e.g. Candida bloodstream infections) to be followed up more quickly. As evidenced by the survey on quality indicators, the surveillance of SSI must be stimulated in Belgium.
The outbound support and cooperation with the competent authorities is good to excellent in the majority of the reports and should be further consolidated with an even quicker feedback of surveillance data from antibiotic use. In the long term, a more restrictive antibiotic policy, of which we are fortunate to notice the first signs (decrease of different classes of beta-lactams and fluoroquinolones) after a long period of increase, is the only sustainable approach to this problem.
At a local level, the service cooperates intensively with the following health partners: hospitals, residential care centers, reference and clinical laboratories. Nationally, we cooperate with the FPS Public Health, in particular the Belgian Antibiotic Policy Coordination Committee (BAPCOC), the RIZIV-INAMI, the Superior Health Council (HGR), Flemish and French communities, healthcare networks in Flanders (Zorgnet/ICURO) and Wallonia (PAQS), the Belgian Infection Control Society (BICS), the universities (including National Reference Centers), National surveillance or nosocomial infections in neonatal intensive care units in Belgium (NEOKISS), Belgian Federal Medicines Agency (FAGG-AFMPS) and AMCRA (Center of Expertise on Antimicrobial Consumption and Resistance in Animals). In addition, assignments are being carried out for the European Commission (DG SANCO), for international agencies: the European Center for Disease Control (ECDC), the European Medicines Agency (EMA), the European Food Safety Agency (EFSA) and the World Health Organization (WHO).
In addition to the already mentioned European projects (EARS-net, ESAC-net, HALT), we participate as a partner or subcontractor in various European initiatives (InterReg VL-NL i-4-1 Health, JAI-AMR, RONAFA, AMEG, (validation) ECDC PPS AB & HAI).
We wish to thank these and all our other external and internal partners (scientific and support services Sciensano (WIV-ISP), Health data member Jan Kips, Thaddé Mahmourian, Juan Quesada, Kris Vranken, Ines Pauwels, Daan Willems, Ludo Willekens, our excellent secretariat in particular Nathalie Verhocht, Yolande Prison, Hubert De Krahe and Tadek Kryzwania) for these collaborations in favor of patient safety.
- Royal Decree - Protocol Agreement on Multidrug resistantorganims (MDRO-protocol akkoord) - Koninklijk Besluit; c-2013/24362, Belgium.
- Duysburgh E, Lambert ML (2017) Surveillance of bloodstream infections in Belgian hospitals (‘SEP’) Report 2017 Data up to and including 2016, ed. Catry B, Sciensano, Brussel. PHS Report 2017-013 ISSN: 2506-9640. [Ref.]
- Healthdata project (2017) Sciensano, Brussel. [Ref.]
- Mertens K (2017) National Surveillance of Infections Acquired in Intensive Care Units – National Report 2015. Sciensano, Brussels. [Ref.]
- Mertens K (2017) National Surveillance of Infections Acquired in Intensive Care Units, HELICS Protocol Belgium, Addendum V23.3.2017. Sciensano, Brussels. [Ref.]
- Mertens K (2017) National Surveillance of Surgical Site Infections, NSIH protocol, Addendum V14/4/2017. Sciensano, Brussels. [Ref.]
- Mertens K (2017) NSIHwin software V4.11. Sciensano, Brussels. [Ref.]
- Albiger B, Glasner C, Struelens MJ, Grundmann H, Monnet DL, and the European Survey on Carbapenemase-Producing Enterobacteriaceae (EuSCAPE) working group (2015) Carbapenemase-producing Enterobacteriaceae in Europe: assessment by national experts from 38 countries. Euro Surveill 20. [Ref.]
- Struyf T, Mertens K (2017) European Antimicrobial Resistance Surveillance Network (EARS-Net) Belgium. Annual report 2017 (data referring to 2016), Sciensano, Brussels. [Ref.]
- EARS-Net Belgium 2016 protocol: Including data call, instructions for participating laboratories, data definition, reporting procedure. Version 7, 6/7/2017. Sciensano, Brussel. [Ref.]
- Hocquart M, Lagier JC, Cassir N, Saidani N, Eldin C, et al. (2017) Early Faecal Microbiota Transplantation Improves Survival in Severe Clostridium difficile Infections. Clin Infect Di. 66: 645-650. [Ref.]
- European Commission (2017) The new EU One Health Action Plan against Antimicrobial Resistance. [Ref.]
- European Center for Disease Prevention and Control (2017) – TESSy – ESAC-Net. Antimicrobial consumption (AMC) reporting protocol 2017. [Ref.]
- Eurostat (2017). [Ref.]
- World Health organisation (WHO) (2017) ATC-classification. [Ref.]
- BAPCOC (Belgian Antibiotic Policy Coordination Committee) (2015) Strategic plan 2014-2019. [Ref.]
- European Center for Disease Prevention and Control (2017) Antimicrobial consumption interactive database (ESAC-Net). [Ref.]
- Fonguh S, Uwineza A, Catry B, Simon A (2016) Belgian hand hygiene campaigns in ICU, 2005-2015. Arch Public Health, 74: 47. [Ref.]
- Duysburgh E, Dequeker S, Mortgat L (2017) Kwaliteitsindicatorenvoorziekenhuishygiëne in acute ziekenhuizenJaarrapport 2017 - Gegevens 2016 (ed.) Catry B. ISSN: 2466-6750. [Ref.]
- Jans B, Latour K, Catry B, Huang Te-Din D, Berhin C, et al. (2016) Nationale prevalentiestudie van dragerschap van resistente bacteriën bij bewoners van woonzorgcentra in 2015. Sciensano, Brussels. [Ref.]
- European Centre for Disease Prevention and Control (2009) The bacterial challenge: time to react. Stockholm. [Ref.]
- Carattoli A, Villa L, Feudi C, Curcio L, Orsini S, et al. (2017) Novel plasmid-mediated colistin resistance mcr-4 gene in Salmonella and Escherichia coli, Italy 2013, Spain and Belgium, 2015 to 2016. Euro Surveill 22: 30589. [Ref.]
- Bories Y, Catry B (2017) Een Oproep Voor Een Nieuw Zorghygiëne Kader
Download Provisional PDF Here
Article Type: RESEARCH ARTICLE
Citation: Catry B, Mertens K, Latour K, Legiest B, Duysburgh E, et al. (2018) Care Infections & Antibiotic Resistance in Belgium. J Epidemiol Public Health Rev 3(3): dx.doi.org/10.16966/2471-8211.165
Copyright: © 2018 Catry B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
SCI FORSCHEN JOURNALS
All Sci Forschen Journals are Open Access
