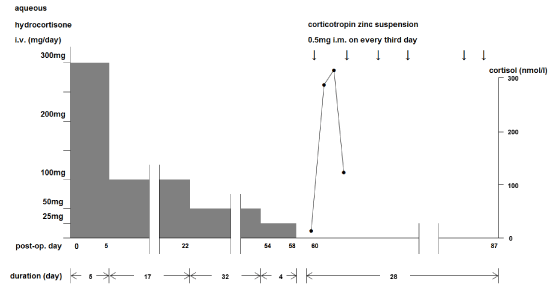
Figure 1: Schedule of Parenteral Hormonal Replacement for Isolated ACTH Deficiency
*Aqueous hydrocortisone, 300 or 100 mg, was supplied as continuous intravenous infusion and smaller doses, 50 and 25 mg, were given as 2-hour infusion.


Toshihide Yamamoto* Yoshihito Kakimoto Hiromasa Harada
Department of Internal Medicine and Surgery, Yao Tokushukai General Hospital, Yao, Osaka, Japan*Corresponding authors: Toshihide Yamamoto, Department of Internal Medicine and Surgery, Yao Tokushukai General Hospital, Yao, Osaka, Japan, Tel: 81729938501; E-mail: toshihide.yamamoto@tokushukai.jp
In contrast to type 1 diabetes mellitus and growth hormone deficiency, isolated corticotropin (ACTH) deficiency (IAD) has been treated by oral administration of glucocorticoids. Supplementation of IAD with ACTH preparation, however, could be an alternative under special circumstances. 69-year-old man, whose IAD had been proved by lack of cortisol response to corticotropin-releasing hormone and intact secretion of other five anterior pituitary hormones, had been supplemented daily with 10 mg of hydrocortisone by mouth until he became afflicted by perforation of the sigmoid colon. The perforation was treated by partial resection of the sigmoid colon and colostomy. Postoperatively, leak from the jejunum developed, which necessitated nil per os and supplementation of hydrocortisone intravenously for two months. As aqueous preparations of hydrocortisone were intendedly marketed for Addisonian crisis or septic shock and available as 100 mg~1,000 mg per vial, it was inconvenient to supply his daily maintenance dose with these preparations. It was decided to treat him with intermittent intramuscular injection of 0.5 mg corticotropin zinc suspension. Daily measurements of cortisol levels after the first injection proved modest blood levels of hydrocortisone up to the third day. Injections were repeated every third day for one month until oral intake became possible. Intermittent injection of corticotropin zinc suspension can be an alternative parenteral replacement therapy for IAD provided treatment is limited to short period, information of rare immediate-type allergic reaction is shared by medical team, and the treatment is carried out in hospital.
Isolated ACTH deficiency; Supplementation of hydrocortisone; Corticotropin zinc suspension
Hormone deficiency disorders appear theoretically better supplemented with respective deficient hormones, e.g. type 1 diabetes mellitus with insulin and growth hormone deficiency with growth hormone. In case of isolated corticotropin (ACTH) deficiency (IAD), oral administration of glucocorticoids has been employed for the supplementation [1,2]. Extraadrenal actions of ACTH of physiological blood levels and their loss have not been known in IAD patients. Oral glucocorticoid treatment is more practical than parenteral administration of ACTH. The circadian rhythm can be simulated to some degree by administration of hydrocortisone in three divided doses [3] or of modified-release preparation of hydrocortisone in patients with primary adrenal insufficiency [4] but restoration of ACTH circadian rhythm is not feasible with current ACTH preparations. Supplementation of IAD with ACTH preparation, however, could be an alternative under special circumstances.
IAD of this patient was diagnosed five years previously when he was admitted for the first time for pneumonia complicated by hypoglycemia and hyponatremia. The diagnosis was proved by lack of ACTH response, i.e. undetectable level (<0.22 pmol/l) before and after 30’, 60’, and 120’of intravenous injection of 100 µg human corticotropin releasing hormone (hCRH “Mitsubishi”, Mitsubishi Chemical Co., ltd., Tokyo). The ACTH levels were measured by ECLIA in ACTH EClusysTM (Roche Diagnostics, Inc., Tokyo) [5]. On the other hand, thyrotropin, growth hormone, and prolactin levels were raised 10-fold of the respective basal levels, luteinizing hormone was raised 5-fold, and follicular stimulating hormone raised 2-fold after injection of corresponding hypothalamic hormones. On a different occasion, cortisol level was proved to be raised from less than 5.5 nmol/l to 91.0 nmol/l at 120’ by intravenous injection of 0.25 mg of aqueous 1-124corticotropin (CortrosinTM, Daiichi-Sankyo Pharmaceutical Co. Ltd., Tokyo). The levels of anterior pituitary hormones and cortisol were measured by Biomedical Laboratories, Ltd., (Matoba, Japan).
Since then, he had been maintained on 10 mg per day of hydrocortisone (CortrilTM, Pfizer Pharmaceutical Co. Ltd., Tokyo) by mouth until he developed perforation of the sigmoid colon at the age of 69 years. The perforation was treated by partial resection of the sigmoid colon and colostomy. Postoperatively, leak from the jejunum developed. He had to be kept nil per os and maintained on total parenteral nutrition until the healing of the jejunal leak. The hydrocortisone supplementation had also to be supplied intravenously. Aqueous preparations of hydrocortisone are intendedly marketed for Addisonian crisis or septic shock and available as 100 mg, 250 mg, 300 mg, 500 mg, and 1,000 mg per vial. In the immediate post-operative period when he required pharmacological doses of hydrocortisone, there were no problems with hydrocortisone preparations. However, when his general condition became stabilized, it is inconvenient to supply smaller dose for daily maintenance, say, 10 mg of hydrocortisone. On the 49th post-operative day while being given hydrocortisone 50 mg per day intravenously, overdose of GC was suspected because of apparent euphoria despite unfavorable prospect. At this stage, it was discussed whether daily intravascular infusion of hydrocortisone could be replaced by intermittent intramuscular injection of corticotropin zinc suspension (1-24corticotropin acetate zinc suspension, distributed as Cortrosin ZTM from Daiichi-Sankyo Pharmaceutical Co. Ltd.). The patient gave informed consent to the change of treatment.
On the 60th post-operative day, the first intramuscular injection of 0.5 mg corticotropin zinc suspension was given. Cortisol levels were measured in the morning before the first injection and then every morning for subsequent three days. The levels were reported as <5.5, 268,290, and 102 nmol/l, which proved efficacy of the injection lasting for three days. The injections had been repeated every third day for a month until oral intake of hydrocortisone was re-initiated on the 88th postoperative day (Figure 1). At one time during this treatment, cortisol level before the injection was 11.0 nmol/l. Priming effect on cortisol secretion by repeated intramuscular injection every third day appeared unlikely. Immediate-type allergic reaction to corticotropin zinc suspension did not occur. He was discharged home on the 141st day with oral hydrocortisone supplementation.

Figure 1: Schedule of Parenteral Hormonal Replacement for Isolated ACTH Deficiency
*Aqueous hydrocortisone, 300 or 100 mg, was supplied as continuous intravenous infusion and smaller doses, 50 and 25 mg, were given as 2-hour infusion.
PubMed-NCBI database was searched using key words, isolated ACTH (or corticotropin) deficiency and treatment, 270 reports were found since 1968. No attempt of treating IAD with corticotropin was described in these reports.
A desirable scheme of hydrocortisone administration for primary or secondary adrenal insufficiency is restoration of circadian rhythm of cortisol levels in blood. When hydrocortisone is infused intravenously for a few hours, cortisol levels increase temporarily but decrease depending on the half-life of 66 minutes [6] or 76.5 ± 5.2 minutes [7] to the basal level four to five hours after finishing infusion. Circadian rhythm of blood cortisol levels cannot be produced by two or more hours’ intravenous infusion of 25 mg or 50 mg of hydrocortisone. Although intermittent intramuscular injection of corticotropin zinc suspension every third day cannot restore circadian rhythm of cortisol in patients with IAD, it can maintain modest levels of cortisol for three days.
One may be concerned with anaphylaxic reaction to corticotropin zinc suspension. One episode of immediate-type allergic reaction was described in a women with ACTH and beta-lipotropin deficiency: 10 minutes after intramuscular injection of 0.5 mg corticotropin zinc suspension for a diagnostic purpose, itching and diffuse erythema developed, hypotension and loss of consciousness followed, and recovery soon ensued after intravenous infusion of hydrocortisone in dextrose [8]. Provided information of possible occurrence of immediate-type allergic reaction to this agent is shared by medical team and the treatment is carried out in hospital, intermittent intramuscular injection of corticotropin zinc suspension could be used temporarily in lieu of parenteral hydrocortisone for IAD patients who have to be kept nil per os.
Intermittent intramuscular injection of corticotropin zinc suspension can be an alternative parenteral therapy for IAD patients if duration of treatment is limited to short period, information of immediate-type allergic reaction to this agent is shared in medical team, and the treatment is carried out in hospital.
The treatment was approved by the clinical study board of our hospital.
The authors have no commercial association that might be a conflict of interest in relation to this article.
Download Provisional PDF Here
Article Type: Case Report
Citation: Yamamoto T, Kakimoto Y, Harada H (2017) Supplementation of ACTH Deficiency with Corticotropin: A Case Report. Int J Endocrinol Metab Disord 3(3): doi http://dx.doi.org/10.16966/2380-548X.144
Copyright: © 2017 Yamamoto T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access