Introduction
Mucopolysaccharidosis (MPS) is a rare and heterogeneous genetic
disease, caused by deficiency or absence of lysosomal enzymes
involved in the degradation of glycosaminoglycans. Abnormal and
progressive accumulation occurs in many tissues, giving a multisystemic
characteristic of this disease [1]. The main clinical manifestations
are hepatosplenomegaly; join stiffness; cardiopathy by valvular and
coronary artery impairment; respiratory, eye, ear and central nervous
system impairment. Neurological involvement is associated with more
severe forms of the disease and may not occur in almost all types [2].
However, phenotypic heterogeneity, variability and severity of clinical
manifestations can be distinguished from MPS within and among types
[3]. The incidence of MPS varies from 1.9 to 4.5 in 100,000 live births [4,5].
In Brazil, a study conducted in the state of Pará identified the incidence
of MPS I as 1:1.440,000 live births [6]. MPS Brazil Network [Rede MPS
Brasil] initiative that enhances the diagnosis and treatment of MPS in
Brazil, identified 1,000 patients with MPS until December, 2012 [7].
Anthropometry aims to investigate the way physical performance
can be altered by growth and development, with regard to body shape,
proportion and composition [8]. Anthropometric evaluation includes
variable measurements according to international protocols, which can
be obtained also by Dual-energy X-ray Absorptiometry (DXA), gold
standard health examination for body mass estimation in humans [9].
By obtaining data from body fat percent (BF%) and body masses, health
professionals can analyze and classify the growth and global status of these
individuals.
This study will allow body composition characterization of individuals
with MPS. The results present a great scientific and clinical relevance, as
several unpublished variables are studied and other hitherto little explored
in this group. The aim of this study was to describe the body composition
of individuals with MPS and, on the exploratory level, to verify the
agreement between the methods for assessing body composition.
Materials and Methods
A cross-sectional study was undertaken in three medical genetics
services in Rio de Janeiro, references in monitoring and treatment of
patients with MPS. A convenience sample of individuals with MPS,
of both sexes, who were regularly followed-up in those services, was
selected; all individuals who were followed-up and met the inclusion
criteria were invited (23 individuals). The study included individuals with
biochemical diagnosis of MPS, five years of age or older, followed-up by
medical staff between the years 2009 and 2010, and whose caregivers or
patients themselves, when older than 18 years, had signed the Informed
Consent (IC). The age of eligibility was due to the protocols used for
the tests. Individuals with MPS who had any physical deformity (joint
or muscle) that would prevent the full realization of the proposed
measures were excluded, besides the presence of associated syndrome
or other status that might also prevent the action of the study protocol.
If the patient (or his guardian) agreed to participate in the study, the IC
was signed and implemented, as well as an anamnesis with information
relating to the patient and study. After the clinical history, anthropometric
measurements began, so as to characterize the body composition of the
study group. The measurements were performed twice in succession and
always by the same investigator (skilled in the art) to decrease the chance
of measurement errors. Within availability of the exam, attendance for
performing DXA was scheduled. The study was approved by the Research
Ethics Committees of the institutions involved.
Body Composition
Body composition was assessed by anthropometric method and by
DXA.
Anthropometric Assessment
The International Standards for Anthropometric Assessment, published
by the International Society for Advancement of Kinanthropometry
(ISAK) were adopted [10]. A skinfold caliper (Cescorf/Top Tec - 0.1 mm
precision) was used to measure skinfold thickness at three anatomical sites
(triceps, subscapular and leg). For measurements of body circumferences
an anthropometric tape (Cardiomed/WCS – 1 mm precision) was used,
considering the following perimeters: head, neck, relaxed arm, waist,
hip and leg. Height measures were also registered using a stadiometer
(Cardiomed/WCS – 1 mm precision), total body mass using a scale
(Welmy/W110H – 100 g precision), length of limbs and bone diameters
using a segment caliper (Cardiomed/WCS - 1mm precision), considering
the following lengths and diameters, respectively: arm, forearm, thigh and
leg; biestiloid, biepicondilian of humerus and biepicondilian of femur.
Body Fat Percentage (BF%; %), Body Mass Index (BMI, kg/m2), Fat Body
Mass (FBM; Kg), Bone Body Mass (BBM; kg), Residual Body Mass (RBM;
kg), Muscle Body Mass (MBM; kg) and Lean Body Mass (LBM; kg) were
obtained from measurements [11].
DXA
The equipment used was the DXA Prodigy Advance Lunar / GE, which
measures the attenuation of x-rays beams emission between 70 and 140
kilovolts synchronized with the line frequency for each pixel of the image
taken by the body scanner. The values obtained in DXA were: Bone
Mineral Content (BMC; g) obtained for trunk, legs, arms, android, gynoid
and total; Bone Mineral Density (BMD; g/cm2); Body Fat Percentage
(BF%; %) obtained for trunk, legs, arms, android, gynoid and total; Total
Body Mass (TBM; kg); Fat Body Mass (FBM; g) obtained for trunk, legs,
arms, android, gynoid and total; Lean Body Mass (LBM; g) obtained for
trunk, legs, arms, android, gynoid and total; Z-score.
Clinical and Demographic Characteristics
The ones responsible for the individuals or the individuals themselves,
when they were 18 years old, answered an anamnesis containing the
following information: age, sex, type of MPS, school routine and physical
activity routine.
Statistical treatment
Analysis was performed using the Statistical Package for the Social
Sciences / SPSS 17.0 for Windows. The descriptive analysis of data
addressed frequency distribution, measures of central tendency (median)
and dispersion (minimum and maximum values and percentiles). The
intraclass correlation coefficient (ICC) was also calculated [12].
Results
Twenty-three individuals who met the inclusion criteria for study
participation were identified. Three individuals were excluded for
cognitive impairment that prevented measurements proposals. There were
five losses (5/20; 25%): four individuals who did not attend the proposed
schedule for evaluation and one who died during the study period. Fifteen
individuals (median = 10 [5 – 34] years) were evaluated: three with MPS
I, five MPS II with, one with MPS IV, and six with MPS VI. Of the total
sample, only four individuals were female, one with MPS I: one with MPS
IV and two with the diagnosis of MPS VI. For the DXA examination, due
to the difficulty of scheduling availability and suitability of participants,
only eight were included in this part of the study (median = 10 [5 – 34]
years), six in common for anthropometric assessment. Of this total, two
had MPS I (one of each sex), two had MPS II (male), one had MPS IV
(female) and three had MPS VI (male). This group showed similar clinical
characteristics, comparing to the total of individuals.
It was found that 40.0% (n = 6) of individuals practiced some kind of
regular physical activity, and almost the whole of that number (83.3%)
in school physical education. As to the school routine, it was found that
66.7% (n = 10) of individuals studied regularly and among these only one
in special class, while two had completed high school.
Table 1 shows the general characteristics of the individuals who
participated in the study. Participants with MPS II (n = 5) had a median
age of 14 years [5 – 34] years, with two adults in the group, and MPS VI
participants had a median age of nine years [5 – 19] years, with an adult
in the group. The two participants with MPS I were less than 18 years. The
average height of the group was 1.12 [0.94 - 1.35] m. Individuals with MPS
II had higher median value (median = 1.25 [1.16 - 1.35] m compared with
MPS VI individuals (median = 1.03; 0.96 - 1.08 m). Short stature (below
the third percentile) was observed in 10 participants (76.9%).
The median body mass in the group was 23.5 [15.4 - 41.2] kg.
Individuals with MPS II had higher median value (median = 37.4; 24.8 -
41.2 kg) compared with MPS I (median = 22.6 [15.9 - 29.2] kg and MPS
VI individuals (median = 21.2 [15.4 - 28.5] kg. The percentile ranking of
individuals up to 20 years old [13], which corresponds to 92.3% of the
sample (n = 12) indicated that these, 8.3% (n = 1) were underweight,
50.0% (n = 6) with normal weight, 16.7% (n = 2) were overweight, and
25.0% (n = 3) had obesity.
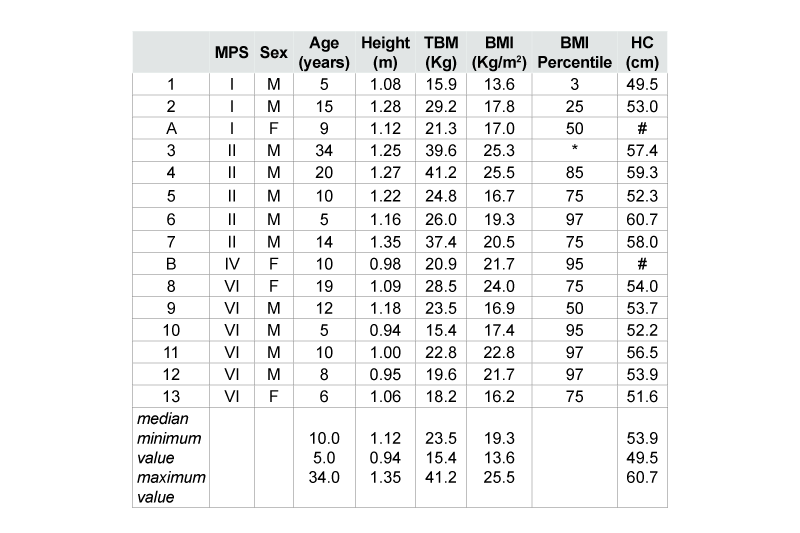
Note: MPS = Mucopolysaccharidosis; TBM = Total Body Mass; BMI = Body
Mass Index; HC =Head Circumference; m = meters; cm = centimeters; kg
= kilograms; kg/m2 = kilograms persquare meter; M = Male; F = Female; * =
individual > 20 years old; A and B = individuals who have made only DXA;
# = individuals do not have anthropometric measurements.
Table 1: General characteristics of individuals with MPS who participated
in the study
When comparing the classifications obtained by BMI and FBM data,
we obtained the following indices and mean BMI and FBM, respectively:
low weight = 1.9 kg (n = 1), normal weight = 3.4 kg (n = 6), overweight =
3.5 kg (n = 2), and obese = 4.7 kg (n = 3). This demonstrates that the mean
values of FBM had a tendency to increase linearly with the changes within
each group classified by BMI. Mean skinfold values in the three anatomic
sites were similar.
The BF% obtained by anthropometric method can classify individuals
over seven years of age [14,15] (69.2% of the sample; n = 9); of these,
22.2% (n = 2) were classified with excessively low BF%; 22.2% (n = 2) were
classified with low BF%; 33.3% (n = 3) with appropriate BF%; and 22.2%
(n = 2) with moderately high BF%.
Eight individuals were identified with head circumference above the
50th percentile (8/13; 61.5%), and among these, four had macrocephaly
(above the 98th percentile) [16]. No individual had microcephaly.
We found that bone lengths do not follow a pattern in relation to age
and type of MPS. The length increases with increasing age, but without the
same uniformity observed in perimeters’ measurements (Figures 1 and 2).
With the completion of DXA we could analyze the correlation between
this test and the anthropometric method for the following measurements:
TBM, BF%, FBM and MBM (Table 2). We calculated the ICC and the
obtained values for FBM and for MBM were 0.89 and 0.99 respectively,
both with statistical significance.
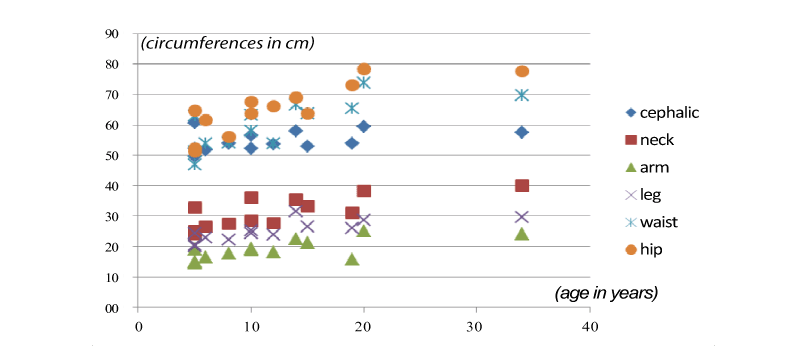
Figure 1: Distribution of body circumferences in relation to age
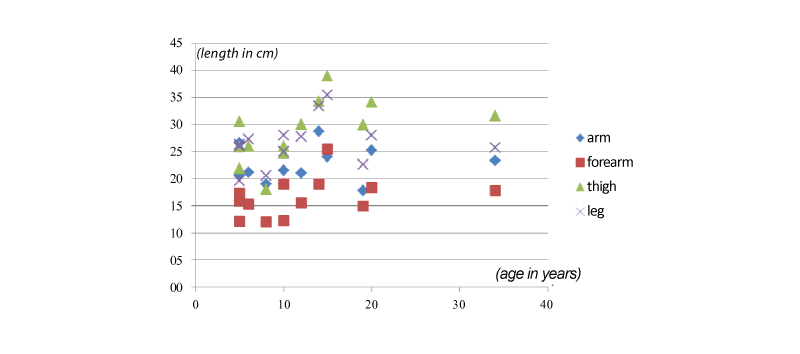
Figure 2:Distribution of the lengths of limbs in relation to age
Through the Z-scores obtained in DXA we observed that two
individuals (2/8; 25%) were classified with osteoporosis and none with
osteopenia.
Discussion
The knowledge of variables related to the growth and development of
children and adolescents, such as height, body mass, body fat and muscle
mass, is extremely important as these, among others, are health indicators
of such populations. Several factors are directly related to the growth and
development of children and adolescents, especially genetics, physical
activity level, dietary patterns, access to health services and the presence
of certain diseases [17].
Stature is a major indicator of the growth of a population and, therefore,
is recommended for systematic monitoring. MPS is a disease associated
with short stature due to dysostosis multiplex that affects, among other
body segments, the spine, long bones and the bones of the hands and feet
[18]. In this study, findings of short stature compared with that predicted
for age group and sex, observed in 76.9% of the study individuals,
corroborate other findings in the literature. The degree of impairment of
linear growth also appears to be influenced by the type and severity of
MPS [19]. In our study, individuals with MPS II had higher height values,
probably because they have minor clinical impairment, beside the fact
that MPS VI has greater osteoarticular involvement, which could also
lead to greater height reduction. In other studies, the effect of enzyme
replacement therapy also showed positive height trends, not only by the
capacity for growth, but also as the increased range of motion in lower
limbs [19,20].
A study conducted in mice with lysosomal storage diseases (MPS I, MPS
IIIB, MPS VII, Niemann-Pick types A and B, and child neuronal ceroid
lipofuscinosis) observed decrease of adiposity [21]. However, not only low
weight and low height were found in our sample; 25.0% of the samples
were classified as obese according to BMI, and according to BF%, 22.2%,
a moderately high rate. Two types of analysis, quantitative and qualitative,
may have shown increased caloric intake, with or without decrease in
energy expenditure. Although in practice we observe the presence of
obesity, we found no reports of its frequency in individuals with MPS.
It has been observed that the increasing prevalence of overweight and
obesity, particularly in children and adolescents, appears to be directly
linked to a lack of motor experience and participation in physical exercise
programs, as well as inadequate eating habits [22].
Most individuals (61.5%) had head circumference above the 50th
percentile, and among these, four individuals had macrocephaly, which is
an observed finding in MPS [23].
We found a 25% frequency of osteoporosis in this study, and it is
expected that this disease occurs in individuals with MPS [24]. The
Z-scores obtained in DXA present lower values in older individuals, which
may result from the disease progression, as changes occur in the bones
due to bone dysostosis and decreased joint motion. This is a characteristic
highly prevalent in all types of MPS [3,18] which can cause the decrease
of bone mass along with the physical decrease [25]. Our results are in
accordance with other study [26], which used DXA to assess 13 children
with MPS I, II, IV and VI, aged from five to 13 years: except for MPS I and
II, all had bone mineral density below the expected for their age group in
the spine region L1-L4.
A little reported fact is the frequency of school activities and
physical activity among MPS individuals. In our study there was a very
small percentage of attendance to physical activities (40.0%), which
may be explained by the clinical manifestations of MPS, such as the
musculoskeletal limitation that makes them less mobile and ultimately
leads to muscle atrophy [27]. School attendance was also considered
low (66.7%) among the participants, and may also be a reflection of the
aforementioned clinical manifestations and especially the neurologic
involvement associated with more severe forms of the disease [2].
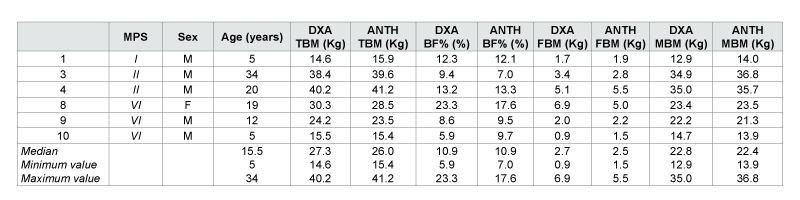
Note:MPS = Mucopolysaccharidosis; DXA = Dual energy X-Ray Absorptiometry; ANTH = Anthropometry; TBM = Total Body Mass, BF% = body fat
percent; FBM = Fat Body Mass, LBM = Lean Body Mass; M = Male; F = Female; The numbers of individuals were kept for further identification; The six
individuals who appear in this table were common between DXA and ANTH
Table 2: Comparison of body composition values obtained by DXA and anthropometry
No significant differences between anthropometry and DXA concerning
variables related to body composition were observed. Regarding the
ICC, statistical significance was found for FBM and MBM. We suggest
that anthropometry can be used without loss of accuracy for these data
[12]. In anthropometry, the acceptable technical error of inter-evaluators
measurement for skinfold for beginners is 10%, and experienced evaluators
is 7.5%, while for other measures it is 2% and 1.5%, respectively.10 DXA
provides more accurate data, as these are directly obtained [9]. It must be
emphasized that the accessibility of the anthropometric method is much
larger than the DXA, lower cost and valid for this type of individual. It
would be of great value training evaluators for this method as compared
to the purchase of large equipment.
Increased neck perimeter can be correlated to increased levels of
adiposity, including BMI [28]. It has been suggested checking the neck
perimeter as an indicator of cardiovascular risk in different populations
[29]. In this study, only one individual (MPS VI) presented the perimeter
above expectations, showing BF% rated “moderately high” and BMI
classified as “normal weight”.
Bone lengths are not always reduced, not following a pattern in relation
to age and type of MPS. Length increases with increasing age, but without
the same uniformity observed in perimeters’ measures, and this may
reflect the heterogeneous aspect and duration of the disease.
The current treatment approach in MPS is booming and is complex,
which has allowed some reduction in the severity of complications
and increased survival of individuals affected by the disease, but early
diagnosis and treatment seem to be fundamental. However, given the
great complexity of the MPS and the wide phenotypic variability within
and between types, knowledge of the characteristics of the disease should
be further explored for the effective management of these individuals [30].
The number of individuals included in this study (13 for anthropometry,
and eight for DXA) reflects the rarity of the disease and was a limitation of
this study, together with the lack of normality curves for some parameters,
leading to difficulties in comparing with the general population.
Conclusion
The study aimed to describe the body composition of individuals
with MPS and altered physical parameters were found, as described
in the literature. Some important changes were found in the sample,
with heterogeneity of results among different types of MPS and among
individuals of the same type. This may reflect the heterogeneity of the
disease stage. Short stature, head circumference above the 50th percentile
and macrocephaly were found and described. The importance of a
multidisciplinary approach to these individuals, who demand interaction
between the various health professionals, must be highlighted. The goals
of treatment are better understanding the disease and giving special
attention to each individual with MPS, respecting their own characteristics
and desires.





