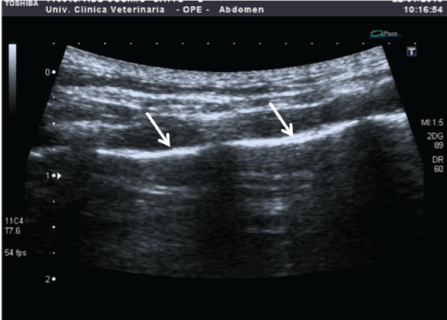
Figure 1: Ultrasound image of normal thoracic wall; hyperechoic line (arrows) corresponds to pleural line.


Citi Simonetta1* Daddi Valentina2 Mannucci Tommaso1
1Department of Clinical Science, University of Pisa, Italy*Corresponding author: Citi Simonetta, Dept Veterinary Science, University of Pisa, Via Livornese - 56122 San Piero a Grado, Pisa, Italy, E-mail: simonetta.citi@unipi.it
Diagnosing pleuro-pulmonary diseases causing acute dyspnea is a daily challenge for radiologists working in intensive care units. Ultrasonography for non-cardiac intrathoracic structures has recently been used as a first responder’s diagnostic method. The aim of this paper is to study the diagnostic accuracy of pleural and lung ultrasound (PLUS) exploiting the experience gained in the use of ultrasound along with X-rays performed on dogs and cats in emergency care. From January 2015 to December 2016 we considered 68 animals (50 dogs and 18 cats) with acute dyspnea, admitted to the “Mario Modenato” Teaching Hospital of the University of Pisa and subjected to thorax ultrasound and X-ray examination. We obtained the final diagnosis of diaphragmatic hernia (5 cases), pleural effusion (28), pneumothorax (6), lung consolidation (8), alveolar-interstitial syndrome (19), and tracheal rupture (2). Ultrasound diagnosis was carried out by directly visualizing the pathology in the case of a diaphragmatic hernia or pleural effusion, and by visualizing the artifacts that altered the physiologic ultrasound semeiotics, as in the case of pneumothorax, alveolar-interstitial syndrome by cardiogenic pulmonary edema, poisoning anticoagulants, acute respiratory distress syndrome (ARDS), pulmonary contusion and alveolar consolidation by aspiration pneumonia. The ultrasound allowed us to identify the disease and its location in most of the cases. The sensitivity and specificity were both 100% for pleural diseases and alveolar consolidation, 100% and between 87.5-95% for the alveolar-interstitial syndrome, respectively. The thoracic ultrasound examination is characterized by good sensitivity, rapid execution, and repeatability, a factor that make it an ideal tool for the management of patients with acute dyspnea; it allows to differentiate cardiogenic to non-cardiogenic edema. In addition, it could be used as an imaging method for clinical and therapeutic follow up of patients, and it reduces exposure to ionizing radiations.
Thoracic Ultrasound; Pleuropulmonary Diseases; Acute Dyspnea; Dogs; Cats
Diagnosis of pleuro-pulmonary diseases causing acute dyspnea is a daily challenge for radiologists working in intensive care units. Dyspnea is a very frequent clinical sign in patients with acute airway diseases. It can be attributed to many different causes and almost always requires stabilization and rapid hospitalization [1,2]. Differential diagnosis can be based on the results of the patient’s medical history, clinical examination, laboratory tests and conventional radiology [3-5]. Traditionally, the first approach to dyspnea has been radiology in both lateral recumbencies, followed, when possible, by dorsoventral (DV) or ventrodorsal (VD) recumbency [5,6].
Ultrasound (US) of non-cardiac intrathoracic structures is still infrequently in veterinary medicine. Studying intrathoracic structures is hindered both by the air content of the lungs and by the bones of the rib cage which block the ultrasound beam and cause artifacts.
For many years such obstacles, along with the frequent use of traditional radiology and the increasing use of computed tomography (CT), have discouraged the development of imaging ultrasound techniques for the lungs [3].
Until the mid-1980s, ultrasound in human medicine was mainly used for the diagnosis of pleural effusion or lung masses that create an acoustic window [7,8]. Since the 1990s thorax ultrasounds have been exploited leading to the identification of physiological and pathological artifacts, which are located in the pleural space and the lung parenchyma [9].
In veterinary medicine, Lisciandro et al. in 2008 carried out a study on Thoracic Focused Assessment with Sonography for Trauma (TFAST), thorax ultrasound examinations performed in critically traumatized patients. TFAST can reveal pleural and pericardiac effusion, pneumothorax and diaphragmatic hernia, but does not take into account lung pathologies [10]. In 2014 Lisciandro et al. joined TFAST at the Veterinarian Bedside Lung Ultrasound Exam (VetBLUE) for the study of lung pathologies [11]. Thoracic ultrasound is now used as a diagnostic method in patients with acute dyspnea in many intensive care units of human and veterinary medicine [1,6,10].
Pleural and pulmonary diseases can be identified with ultrasound by direct visualization of the lesion or by the identification of artifacts, which alter the physiological ultrasound semeiotics. There are three principle signs in PLUS: A-lines, lung sliding, and B-line.
A-lines are repetition artifacts that originate from the ultrasound beam meeting with a highly reflective surface caused by the physiological air lung content and are found in healthy patients. They appear as horizontal, parallel and hyperechoic lines that extend from the pleural line with regular intervals and tend to decrease their intensity with the depth of the scan [12,13,14] (Figure 1).

Figure 1: Ultrasound image of normal thoracic wall; hyperechoic line (arrows) corresponds to pleural line.
Lung sliding is a dynamic ultrasound sign, which can be observed on the pleural line and is generated by the sliding of the visceral pleura on the parietal pleura, during the patient’s breathing actions. This movement suggests the physiological contact of the two pleural tissues [12-15]. B-lines are represented by hyperechoic lines starting from the pleural line and perpendicular to it, which move simultaneously with the patient’s breathing and extend through the depth of the scan with the same intensity (Figure 2). These lines highlight the presence of an alveolar-interstitial syndrome, which can occur due to the presence of extra vascular water, as happens in pulmonary edema or an increase in thickness of the interstitium [9,16,17]. In human medicine, the number of B-lines increases with the severity of disease and consequently dyspnea and is directly related to signs of pulmonary congestion on a chest radiograph [18-20].
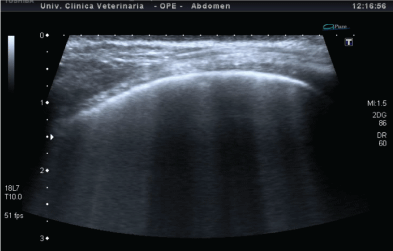
Figure 2: Thoracic wall; starting from the pleural line some hyperechoiclines (B-lines), due to ring down artefacts, are evident; pleura is regular and not thickened in a patient with cardiogenic pulmonary edema
Other characteristic artifacts can be identified in presence of pulmonary thickenings or alveolar consolidation, defined as the presence of material or non-physiological tissue in air spaces with a tissue-like image.
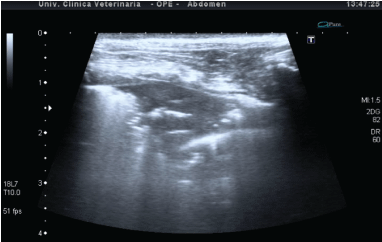
Figure 3: Shred sign image in a patient with pneumonia. It is possible to notice the peripheral pulmonary consolidation with irregular reverberation areas and central air bronchogram.
The aim of this work is to describe the ultrasound findings of Pleuro-pulmonary diseases causing acute dyspnea and to assess the value of PLUS compared with thorax X-rays.
This was a prospective study in emergency patients. All the owners gave informed consent for the performance of the thorax ultrasound, which is routinely carried out in our department. The study protocol was reviewed and approved by the Institutional Welfare and Ethics Committee of the University of Pisa (permission number 33472/2016).
This observational study included 68 patients, dogs and cats, admitted for acute dyspnea to the Veterinary Teaching Hospital “Mario Modenato”, Department of Veterinary Science, University of Pisa, during the period January 2015- December 2016. All dogs and cats were subjected to radiographic and ultrasound examination of the thorax; the imaging examinations were performed with no clinically relevant time delay and no additional medical interventions in between.
The evaluation of the X-rays and the execution of the ultrasound examinations were carried out independently by two radiologists (Citi S and Mannucci T), so that the physician assigned to the X-rays had no knowledge of the results of the ultrasound and vice versa.The X-ray was performed by a digital radiology system (Fuji Capsula) in right latero-lateral (rLL) recumbency or in several recumbencies (rLL, lLL, VD or DV) in accordance with the patient’s clinical condition.The ultrasound investigations were performed using a linear probe 12 MHz and a microconvex probe 7.5 MHz (Toshiba Xario XG) both were used for each study.
Ultrasound images and videos were taken with the patient awake and manually restrained. The patient preparation involved only the application of alcohol and ultrasound gel on the thorax area. The patient was placed in right recumbency and then in left recumbency, if it’s clinical condition allowed it. In cases of severe dyspnea, the examination was carried out in sternal recumbency or standing. In all cases, ultrasound included a longitudinal and transversal intercostal approach, moving the probe in a dorsoventral direction and then in a craniocaudal direction for both hemithoraces.
The ultrasound diagnosis was obtained through direct visualization of the pathology (diaphragmatic hernia and pleural effusion), or through the visualization of artifacts that altered the physiological ultrasound semeiotics, as in cases of pneumothorax, alveolar-interstitial syndrome and alveolar consolidation.
B-lines are identified rare (≤ 3 B-lines per hemithorax), numerous (>3 B-lines per hemithorax), confluent (multiple Blines blended together per hemithorax), and with lung (B-lines totally merged) [13,14,23].
The sensitivity, specificity, positive predictive values (PPV) and diagnostic accuracy (DA) of PLUS were calculated using standard formulas.
A total of 68 patients were included in this study: 50 dogs (73.5%) and 18 cats (26.5%). A variety of breeds was represented in both populations (dogs and cats) and no significant prevalence among breeds was noticed. Twenty three dogs (47%) were medium-sized. The dog population divided into 31 males, 6 females and 13 sterilized females. The feline population consisted of 3 males, 7 neutered males, 1 female, and 7 sterilized females. Age ranged from 4 months to 21 years with a greater incidence of patients (67%) aged between 6 and 8 years. The radiological exam was carried out in three recumbencies rLL, lLL and VD or DV in 11 patients, two LL recumbencies in 48 patients and only in rLL recumbency in 9 patients.
The PLUS was performed in all patients on right and left hemithorax, with an examination time of less than 5 min.
The final diagnosis was diaphragmatic hernia in 5 patients, pleural effusion in 28, pneumothorax in 6, alveolar-interstitial syndrome in 19, alveolar consolidation in 8 and tracheal rupture in 2 [Table 1].
| Pathologies | Cases |
Radiological Diagnosis | Ultrasound Diagnosis | Additional Ultrasound Information |
| Diaphragmatic Hernia | 5 |
3 certain 1 uncertain 1 not seen |
5 |
Herniated organs |
| Pleural Effusion | 28 | 28 |
28 |
Fluid echogenicity; Lesions not radiologically visible |
| Pneumothorax | 6 | 6 |
6 |
Lung point |
| Interstitial-Alveolar Syndrome |
19:
|
19 (seen as alveolar pattern) |
19 with 2 different patterns |
Layers of pleural effusion seen in: 3cardiogenicoedema, 3 ARDS e 1 poisoning by anticoagulants |
| Alveolar Consolidation | 8 inspiration pneumonia | 8 |
8 |
Shred sign; air bronchogram |
| Tracheal Rupture | 2 | 2 |
- |
- |
Table 1: Division of clinical cases in 6 categories based on final diagnosis, comparing radiological and ultrasound exams. Even additional ultrasound information is reported.
Ultrasound has highlighted pleural space disorders (diaphragmatic hernia, pleural effusion and pneumothorax) in all affected patients, demonstrating sensitivity, specificity, positive predictive value and diagnostic accuracy of 100%. Radiology was doubtful in 2 patients with unilateral diaphragmatic hernia. In some patients with pleural effusion, ultrasound has also led to the identification of the cause. In two subjects pleural nodular lesions were detected, attributable to primary neoplasia; in two cases millimetric subpleural lung nodules due to lung metastases were detected; in three patients with pyothorax, grass awns were identified.
Alveolar-interstitial syndrome was identified in 19 patients, for the presence of B-lines but with two different pleural patterns:
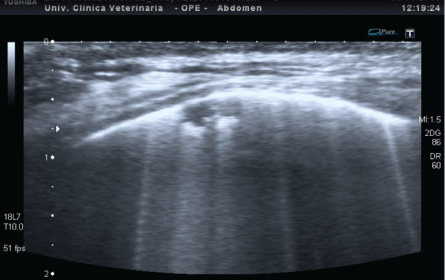
Figure 4: US detection of B-lines associated with irregular, thickened pleural line and sub-pleural consolidations in a patient with ARDS (compare with Figure 2).
Alveolar consolidation was revealed in eight patients and the final diagnosis was aspiration pneumonia in all subjects. Inspiration pneumonia appeared by ultrasound as an alveolar consolidation with pointed or linear dynamic air bronchogram and peripheral shred sign. The right middle lobe was involved in 7/8 cases, and the ventral portion of the cranial lobes in 4/8.
In two cats with tracheal rupture, ultrasound showed no alteration. The radiological suspect was confirmed by CT
Sensitivity, specificity, positive predictive value and diagnostic accuracy of the lung ultrasound in alveolarinterstitial syndrome are shown in Table 2.
| Sensitivity | Specificity | PPV | DA | |
| Cardiogenic edema | 100% | 95% | 72.7% | 95.5% |
| Anticoagulants Poisoning | 100% | 87.7% | 27.2% | 88.2% |
| ARDS | 100% | 93.7% | 50% | 94.1% |
| Lung Contusion | 100% | 93.7% | 50% | 94.1% |
Table 2: Sensitivity, specificity, positive predictive value (PPV) and diagnostic accuracy (DA) of lung ultrasound in alveolar-interstitial syndrome.
The aim of this study was to evaluate the diagnostic accuracy of PLUS, performed by radiologists at the time of initial evaluation of acute dyspnea. An US evaluation was feasible in all patients, with a very short examination time (lower than 5 min). PLUS was performed immediately after the patient’s initial evaluation to prevent the risk of obtaining a negative test like a consequence of appropriate treatment. Indeed B-lines, due to cardiogenic edema, are dynamic artifacts that can disappear rapidly after edema resolution [23].
For diseases of the pleural space, especially for diaphragmatic hernia and pleural effusion, ultrasonography has a higher diagnostic accuracy than radiology, as already demonstrated in the literature [13,24,25]. In our cases of diaphragmatic hernia, radiographic images provided definitive diagnoses in 3/5 patients: one cat was differential diagnosis of torsion of the right middle lobe, and in another cat unilateral pleural effusion was misdiagnosed. In pleural effusion, ultrasound detected the sonographic appearance of the fluid; in some cases US also identified the underlying cause of effusion, for example pleural or lung neoplasia and foreign bodies.
In all pneumothoraxes, ultrasonography highlighted the absence of lung sliding. In human medicine, this can be detected with 100% sensitivity, 100% negative predictive value, but with specificity between 60 and 90% [15]. This is because the absence of sliding can also be found in some cases of pulmonary fibrosis, pleural adhesions, or atelectasis massive [15]. The specificity achieves 94% if the absence of lung sliding is associated with the absence of B-lines [15]. In all six cases of pneumothorax, the absence of both artifacts was found, showing a sensitivity and specificity of 100%.
All cases of alveolar interstitium syndrome were characterized by the presence of B-lines. In the human and veterinary literature, the presence of bilateral B-lines with smooth and non-thickened pleura is generally associated with cardiogenic pulmonary edema [18,19,23]. B-lines and irregular, thickened and nuanced pleura are associated with the hyperacute phase of pulmonary contusion or non-cardiogenic pulmonary edema [25,26].
In the present study the PLUS has allowed to differentiate cardiogenic from non-cardiogenic edema in the 19 cases of alveolar interstitium syndrome. The presence of diffuse B-lines associated with regular pleural aspects had a sensitivity of 100% and a specificity of 95% for the diagnosis of cardiogenic dyspnea, with a positive predictive value of 72.7%. PLUS showed three false positive results for anticoagulant poisonings. B-lines associated with an irregular and thickened pleural aspect with the presence of subpleural thickening had a sensitivity of 100% and a specificity of 93.7% for the diagnosis of ARDS, with positive predictive value of 50%. PLUS showed 4 false positive results for final diagnosis of lung contusion.
The sensibility and sensitivity of PLUS for the detection of consolidation in critically ill patients have been reported in human medicine as 90% [22]. In the present study lung US showed, in identifying this abnormality, sensibility, sensitivity, positive predictive value and diagnostic accuracy of 100%. All eight cases presented a lobarconsolidation and were located in more than one region in three patients. Alveolar consolidation can result from several different pathologic conditions that include not only pneumonia but also ARDS, lung contusions, lung lobe torsion and some lobar neoplasia [13,14,27]. Finally, medical history and information obtained by clinical examination, radiology, and clinical and ultrasound follow up have been useful to get the final diagnosis of aspiration pneumonia.
US in cats with tracheal rupture did not provide any information, except for the absence of artefacts associated with lung or pleural diseases. In both cases reported in this study, the suspected diagnosis was confirmed by CT.
Thoracic radiology remains the primary diagnostic imaging method used in patients with acute dyspnea. The fast thoracic movements and the poor cooperation of the animal due to forced recumbence can lead to a poor quality radiogram. In critically ill patients three complete radiographic projections are difficult to be carried out. One or two recumbencies may be insufficient for an accurate diagnosis, especially without the projection VD/DV. The exposure to ionizing radiation both for the patient and for the operator is the other disadvantage of radiography, especially if several radiographic checks are needed over time.
In our study, PLUS proved to be an efficient, safe, feasible method. The highly diagnostic accuracy aided the diagnosis of pleuro-pulmonary diseases in acute dyspnoic patients. Finally, thoracic US are easily repeatable, allowing the patient to be closely monitored several times a day while in the intensive care unit. The real time ultrasound image evolves rapidly, and ultrasound can be used to monitor treatment responses during patient follow-up. The patients enrolled in this study with cardiogenic pulmonary edema were treated with diuretic therapy and underwent a second ultrasound examination after a few hours.This showed a reduction of B-lines. The ultrasound examinations in cases of poisoning by anticoagulant and pulmonary contusion showed a temporal evolution over the following days with a change in the pulmonary consolidation associated with air bronchograms (Figure 5).
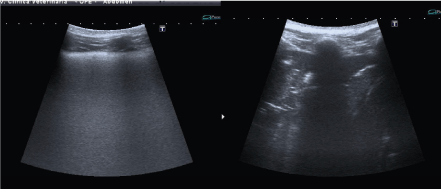
Figure 5: Anticoagulants intoxication in a dog; (left) day one, note the presence of confluents B-lines that provides white lung aspect. (right) day two, modification of the image with pulmonary consolidation and air bronchogram.
The absence of thoracic ultrasound findings in patients with acute dyspnea should address the clinician to focus on diseases localized to tracheobronchial tract.
In conclusion, thoracic ultrasound could be used at the intensive care unit for dogs and cats in dyspnea as supplementary information to the medical history, clinical examination and radiology in order to obtain as many details as possible.
Download Provisional PDF Here
Article Type: RESEARCH ARTICLE
Citation: Simonetta C, Valentina D, Tommaso M (2017) Thoracic Ultrasound: A Method for the Work-Up in Dogs and Cats with Acute Dyspnea. J Anim Sci Res 1(1): dx.doi.org/10.16966/2576-6457.104
Copyright: © 2017 Simonetta C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access