Abstract
Optimal exposure is one of the key factors for a successful MV surgery. Because the left atrium is located at the back of the heart, MV exposure
may be very difficult. This article describes an approach which consists in sectioning the antrum of the pulmonary veins. By rotating and pulling out
the heart, the mitral valve can be fully exposed. This technique is highly recommended for those cases with small left atrium.
Keywords
Cardiac surgical procedures; Heart atria; Mitral valve; Pulmonary veins
Introduction
Perfect exposure of the mitral valve (MV) is crucial to perform any type of MV surgery. Small left atrium (LA), posterior location of the LA in the heart, a very deep thoracic cavity and median sternotomy as preferred usual approach are factors affecting the MV visualization. Sometimes, the conventional LA incision through Sondergaard’s groove does not give ideal exposure. Taking into account that the LA is located at the back of the heart, disconnection of the pulmonary veins (PV) antrum from the LA and twisting the heart by clockwise rotation offers an excellent solution for MV exposure.
Surgical Technique
Operation is performed through a full median sternotomy. Ascending
aorta and bicaval cannulation is used. Cardiopulmonary bypass is
established to moderate hypothermia. The aorta is cross-clamped and
cold anterograde cardioplegic solution is administered. The LA is opened
vertically from the right side in front of the right PV as usual. Two median
Deaver retractors are placed under the MV. This manoeuvre makes it
possible to identify the bulging between the PV antrum and the rest of
the LA. The incision is extended inferiorly through the mitral itsmus
until reaching the area between the base of the LA appendage and the
left PV. Then, the incision is prolonged behind the superior vena cava
and all around the LA roof encompassing the other end of this one. Two
landmark sutures are placed in both sides of the LA before its division
in order to facilitate the future anastomosis while preventing some
malalignment. PV are now completely isolated. At this point, Deaver
retractors are removed, and the heart is twisted by clockwise rotation.
By a translation of the sectioned plane of the LA to another one more
horizontal and anterior making a turn of almost 180 degrees, the surgeon
can work on both the MV and LA at ground level. A very exceptional
view of the MV is obtained (Figure 1). After MV surgery has been made,
the heart is repositioned into place and the LA is sewn with a 3-0 prolene
over-and-over running suture, begining at the most posterior point,
according to the two marking sutures.
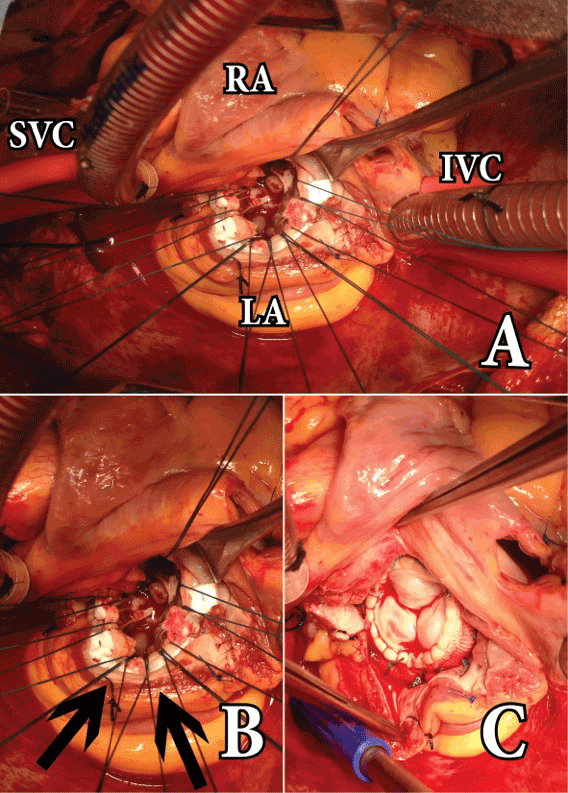
Figure 1. Different stages of operation. A: Panormic view of the mitral
valve approach. B: Once the pulmonary veins have been isolated, the
heart is twisted by clockwise rotation. With this maneuver, the posterior
border of the left atrium becomes the most anterior structure in the
operative field. The arrows indicate the sectioned posterior border of the
left atrium. C: Mitral valve bioprosthesis has been inserted under vision
of all the native mitral annulus.
IVC: Inferior Vena Cava, LA: Left Atrium, RA: Right Atrium, SVC: Superior
Vena Cava.
Discussion
Optimal visualization of the MV is required for any MV surgery. Several
factors such as the space orientation of the MV pointing backwards, the
location of the LA at the back of the heart and the median sternotomy
as preferred approach may adversely affect the correct visualization
of the MV. Moreover, a small LA and a very deep thoracic cavity can
exacerbate the lack of MV exposure. All these factors may make the
classic conventional LA incision inadequate to address the MV. Several
alternative MV approaches have been described [1-6].
We must keep in mind that the LA can be divided into two main parts,
viz, one section containing the MV and LA appendage, and another one
containing the PV (also called PV antrum). In this technique described here,
the surgeon totally cuts the LA into those two halves described above.
PV isolation approach for MV surgery proposed in this paper has the
advantage of working at ground level. This is thanks to the twisting of
the heart by clockwise rotation after the PV has been isolated. Making a
turn of almost 180 degrees, the sectioned plane of the LA is translated to
another more anterior and horizontal one. As a result, the surgeon can
work on the MV at floor level. A spectacular view of the MV is obtained
by this technique.
It is sometimes difficult to choose the most appropiate MV approach,
and opening the LA is mandatory. Most of the time, the LA is initially
opened in a conventional fashion parallel to the Sondergaard´s groove.
If additional exposure is needed, the original incision is simply extended
into the LA. This technique is also useful when a Cox-maze III procedure
is performed in addition to the MV surgery. An excellent surgical view
of both, the LA appendage as well as the MV itsmus is achieved with this
technique.
This approach described here was initially performed as a part of atrial
fibrillation surgery [7,8]. It has been successfully used by the author in
more than 150 cases of MV disease since 1998 (Table 1).
| Variable |
| Cases |
179 |
| Age |
62 ± 17 years |
| Gender, Female |
127(70.9%) |
| Mitral valve pathology |
| Pure Stenosis |
8 (4.5%) |
| Pure Regurgitation |
70(39.1%) |
| Combined stenosis and regurgitation |
101(56.4%) |
| NYHA |
2.7 ± 1.3 |
| LVEF |
0.51± 0.07 |
| Leftatrial diameters |
| Supero-inferior |
6.1 ± 2.3 cm |
| Antero-posterior |
7.6 ± 2.1 cm |
| Transversal |
5.8 ± 2.0 cm |
| PASP |
61 ± 13 mm Hg |
| LVESD |
39 ± 1.1 mm |
| LVEDD |
49 ± 0.7 mm |
| Sinus rhythm |
87(48.6%) |
| Atrial fibrillation |
86 (48%) |
| Other rhythm |
06(3.4%) |
| Intraoperative results |
| Operative mortality |
09 (5.02%) |
| In-hospital mortality |
08 (4.5%) |
| CBP time |
140 ± 15 min |
| Aortic cross-clamp time |
115 ± 18 min |
| Mitral valve procedures |
| Biological prosthesis |
116 (64.8%) |
| Mechanical prosthesis |
43 (24%) |
| Mitral valve repair |
20 (11.2%) |
| Associated procedures |
| Tricuspid valve repair |
35 (19.6%) |
| Tricuspid valve replacement |
02 (1.11%) |
| Aortic valve replacement |
12 (6.7%) |
| Coronary artery bypass grafting |
05(2.8%) |
| Left atrial reduction |
27 (15%) |
| Left atrial appendage removal |
136 (75.9%) |
| Postoperative results |
| Bleeding in 24 hrs |
480 ± 75 mL |
| Reoperation for bleeding |
9 (5.02%) |
| Definitive pacemaker |
6 (3.4%) |
| Use of vasoactive agents |
130 (72.7%) |
| Acute renal failure |
13 (7.3%) |
| Extubation in OR |
125 (69.8%) |
| Prolonged intubation > 8 hours |
42 (23.4%) |
| LOS in ICU |
3.4 ± 2.2 days |
| LOS in-hospital (postoperative) |
9 ± 5 days |
Table 1: Preoperative, intraoperative and postoperative data of all patients
undergoing mitral valve surgery by the pulmonary veins isolation approach.
In conclusion, the PV isolation approach for MV surgery is a good
solution for cases with not optimal MV exposure. It addresses the issue
of the posterior location of the LA and MV at the back of the heart. This
approach is highly recommended in cases with small LA.
Conflict of Interest:
None declared
Download Provisional PDF Here
Article Information
Article Type: Case Report
Citation: Garcia-Villarreal OA (2015) The Best
Exposure of the Mitral Valve: The Pulmonary
Veins Isolation Approach. J Surg Open Access 1(1): doi
http://dx.doi.org/10.16966/2470-0991.101
Copyright: © 2015 Garcia-Villarreal OA This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Received date: 17 August 2014
Accepted date: 22 August 2015
Published date: 30 August 2015