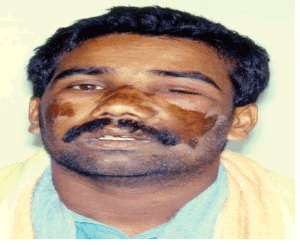
Figure 1: Left side orbital cellulitis at the time of presentation (Front view)


Khalid Abdelwahab Ahmed*
Consultant Oral and Maxillofacial Surgery, Department of Dentistry and Oral and Maxillofacial Surgery, Prince Sultan Military Medical City, Riyadh, Kingdom of Saudi Arabia*Corresponding author: Khalid Abdelwahab Ahmed, Consultant Oral and Maxillofacial Surgery, Department of Dentistry and Oral and Maxillofacial Surgery, Prince Sultan Military Medical City, Riyadh, Kingdom of Saudi Arabia, Tel: +00966 501991155; E-mail: dr.k_ahmed@hotmail.com
Orbital cellulitis and subsequent orbital abscess are fortunately uncommon sequelae of the spread of odontogenic infection to adjacent maxillary sinuses or to distant sites such as the orbits. The spread of such infection once happen can be of serious complication such as complete blindness or even more serious and life threatening situations as cavernous sinus thrombosis, intra-cranial abscess, or even death. Two cases are presented to demonstrate the differences between the two conditions and the necessary management in either case.
Orbital cellulitis; Orbital abscess; Odontogenic infection; Spread of dental infection
Orbital cellulitis and orbital abscess is an uncommon condition previously associated with severe complications. If untreated, these conditions can be potentially sight and life threatening such as cavernous sinus thrombosis, intra-cranial abscess, and death. Fortunately enough, with current advances in antibiotic therapy, surgical techniques and investigations the morbidity and complications are greatly reduced. Orbital cellulitis cases are characterized by initial eyelid edema, erythema, chymosis, proptosis, blurred vision, fever, headache, and double vision, while the orbital abscess cases show eventually pus discharge through the medial canthus of the affected orbit. Odontogenic etiology due to progression of infection to the adjacent maxillary sinuses into to the orbital tissues through orbital floor defects and fissures had been reported. These dental infections may arise from infected maxillary molars [1-4] or maxillary premolars [5] either following periapical dental infections, [1,5] maxillary molar extraction [6], maxillary third molar surgery, [7] root canal treatments, [8] or infected periodontal pockets [9]. Odontogenic etiology of orbital abscesses had also been reported associated with deciduous teeth [10]. Fortunately enough only few cases of orbital abscesses of odontogenic origin were reported to progress to more serious situations where patients lost their sight on the affected side [5,11-13] or even progress to a more serious complications such as cavernous sinus thrombosis, intra-cranial abscesses and death [4,12,14,15].
Two cases of orbital infection of odontogenic origin are reported below with the first case presented with orbital cellulitis while the infection in the second case progressed to orbital abscess and cavernous sinus thrombosis.
A 28 years old Indian male patient attended the emergency clinic of the dental college, King Saud University, Riyadh, Saudi Arabia complaining of marked facial swelling involving the left side of the mid-face and the left eye. On examination, the facial swelling was brawny hard with marked cellulitis. The skin of the lateral side of the nose and over the cheek area bilaterally was burned by Tiger oil which was placed by the patient in a trial to relief his pain (Figures 1 and 2).

Figure 1: Left side orbital cellulitis at the time of presentation (Front view)
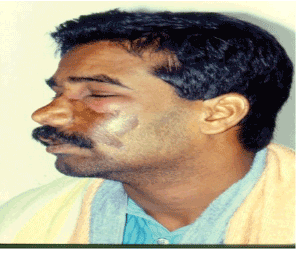
Figure 2: Left side orbital cellulitis at the time of presentation (Lateral view)
Intra-orally, obliteration of the left buccal sulcus by a flatulent swelling was noted extending from the midline to the second molar region. Dental examination revealed a non-vital upper left central incisor which received an uncompleted root canal therapy (Figure 3).
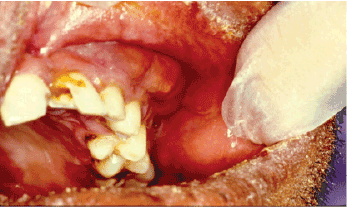
Figure 3: Intra-oral view showing buccal sulcus obliteration with pointing area. Upper left central incisor tooth was broken with uncompleted root canal treatment
Under topical anesthesia with ethyl chloride spray the intraoral abscess cavity was incised and drained and a corrugated rubber drain was inserted. The left central incisor root canal was left open to aid in drainage. A per oral course of ampiclox and metronidazole was prescribed and the patient was discharge to come for a daily out-patient follow up visits. The swelling subsided down rapidly and the drain was removed on the third day. Total recovery commences by the seventh day and root canal therapy of the involved tooth was carried over thereafter (Figure 4).

Figure 4: Postoperative view of the left orbital cellulitis case a week after treatment
A 19 years old Saudi patient was seen in the emergency clinic of the dental college, King Saud University, Riyadh, Saudi Arabia with a history of a swelling of one week duration of the right side of the face following toothache involving a maxillary right molar tooth. Prior to referral the patient had been under treatment at a primary care unit with ampicillin, cephalosporin, eye wash and gel, and mouth wash, but no improvement was noted.
On examination, the patient looked very ill, irritable and uncooperative. The swelling around the right eye was tender and diffuse extending into the infra-orbital regions. Proptosis of the right eye with pus discharge from the medial canthus was also noted (Figure 5). Intraoral examination revealed erythema, and swelling of the right cheek and maxillary buccal sulcus. The right first molar tooth was carious and tender to percussion. An orthopantomo-graphic and periapical x-ray views showed diffuse periapical radiolucency in relation to the first molar tooth and opacification of the right maxillary sinus (Figure 6).
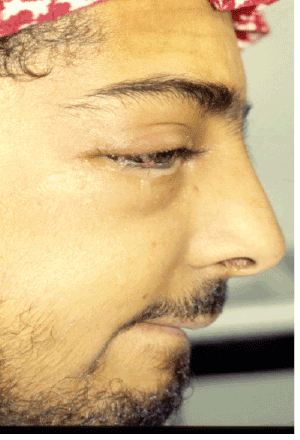
Figure 5: Right side orbital abscess case at the time of presentation, note the pus discharge from the medial canthus (Lateral view)
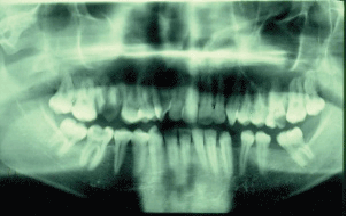
Figure 6: Ortho-pantomo-graphic x-ray view of the orbital abscess case at the time of presentation, note the infected remaining roots of the upper right first molar
Under local anesthesia, the right first molar tooth was extracted and pus was drained through the extraction socket. On the next day the patient reported with worsening of right eye proptosis and the upper and lower eyelid became more edematous with brawny indurations on palpation (Figure 7). The patient was then immediately referred for ophthalmologic consultation at King Khalid Eye Specialist Hospital, where confirmation of the diagnosis of right orbital abscess and right maxillary and ethmoid sinusitis was made with a query cavernous sinus involvement. The patient was then rushed to the operating room, where under general anesthesia the right orbital abscess was drained and right maxillary antrostomy was performed. A drain was left in the right orbital abscess for four days. Energetic antibiotic therapy of Keflex 500 mg orally 6 hourly in addition to heparinization to prevent intra-cranial thrombi formation was carried over.
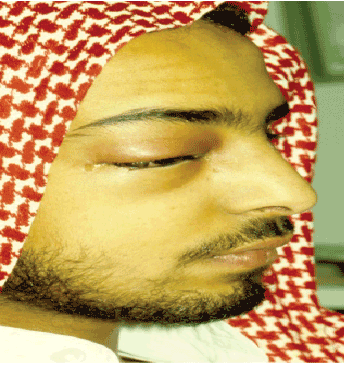
Figure 7: Right side orbital abscess case at the second day following tooth extraction and pus drainage. The patient looks very sick and shows more periorbital in duration
The proptosis decreased rapidly from 13 mm to 6 mm on the fourth day and by the tenth day there was complete resolution of the condition and the drug therapy was discontinued after another four days (Figure 8). Follow up examination of the patient a month later showed that the patient was fully recovered with no residual after effect (Figure 9).
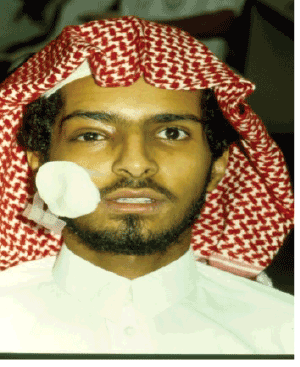
Figure 8: Right side orbital abscess case one week after orbital incision and drainage
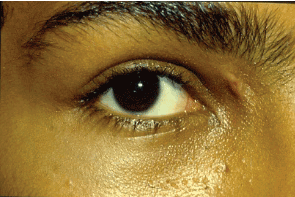
Figure 9: Right side orbital abscess case one month after orbital abscess incision and drainage, note total recovery and the scar of the medial canthus incision
Orbital cellulitis and discrete abscess formation aroundthe orbit is mainly a sequel of spread of infection from the neighboring paranasal sinuses in about 70-80% of the cases [16]. Odontogenic etiology of orbital infection constitutes a lesser percentage of about 10% of the cases [17]. Maxillary teeth are usually the source of odontogenic infection of the obit although it was reported that infection from the mandibular teeth can also reach the orbital content and induce orbital involvement [1,18- 20].The Odontogenic infection can reach the orbit directly by spreading backwards into the pterygopalatine and infratemporal fossae then via the inferior orbital fissure to reach the orbital tissues. On the other hand spread of odontogenic infection into the maxillary sinuses can eventually reach the orbit either by direct continuity or via the venous system as a thrombophlebitis resulting in a purulent orbital infection [20]. Delay in irradication of orbital infection may result optic neuritis and permanent blindness as a result of extreme congestion and edema of the orbital content and obstruction of blood flow through the retinal artery. In addition, even more serious complications as a results of its further spread into the cranium such as cavernous sinus thrombosis, intra-cranial abscess, and eventually death may occur [11,12].
The cavernous sinus directly communicates with the posterior orbit via the superior ophthalmic vein with the normal direction of venous flow from the orbital veins to the cavernous sinus. In addition, the superior and inferior ophthalmic veins having no valves allow extensive two way communication between the face, nasal cavity, pterygoid region and paranasal sinuses. Since both veins communicate with the cavernous sinus, extension of odontogenic infection either into the orbit or direct through the rich venous may result in cavernous sinus thrombosis [12,15,21]. The clinical signs of cavernous sinus thrombosis include marked eye lid edema and discoloration as well as early onset of complete internal and external ophthalmoplegia from palsies of cranial nerves III, IV, and VI. Paresthesia in the distribution of V1 and V2 is also seen. Bilateral orbital involvement was also being reported, indicating spread of infection to the contralateral side through the connecting venous channels. Evidence of meningeal irritation, with altered states of consciousness as well as generalized sepsis, nausea and vomiting, are signs indicating intracranial extension of the infective process [21]. Treatment of cavernous sinus involvement includes hospitalization, broad spectrum parental antibiotic therapy, close monitoring by ophthalmologist and neurosurgeon, and surgical intervention via incision and drainage of the orbital abscess, exploration of the involved paranasal sinus, intraoral incision and drainage, and extraction of the offending tooth. In addition, heparinization may be indicated to avoid development of septic thrombi [21].
The two cases reported clearly demonstrated the various signs of spread of odontogenic infection to the orbital tissues. While the first case presented orbital cellulitis, the second case presented a more serious involvement of the orbit in the form of orbital abscess with purulent discharge from the medial canthus and the possible progression of infection to the cavernous sinus with early signs of cavernous sinus thrombosis and intra-cranial irritation. Early surgical intervention to drain accumulated pus together this aggressive antibiotic therapy yielded control of the active and serious odontogenic infection and prevented a more serious and possible lethal sequlae.
The management of orbital infections is basically the same as other types of infection, and includes vigorous antibiotic therapy and surgical intervention for drainage of the abscess cavities and extraction or root canal treatment of the offending tooth. In addition, it is also equally important to carefully monitor the patient’s vital signs in order to detect any possible intra-cranial complications.
Download Provisional PDF Here
Article Type: Case Series
Citation: Ahmed KA (2016) Orbital Cellulitis and Orbital Abscess of Odontogenic Origin: Two Case Reports and Literature Review. Int J Dent Oral Health 2(7): doi http://dx.doi.org/10.16966/2378-7090.206
Copyright: © 2016 Ahmed KA. This is an openaccess article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access